5 Mistakes When Diagnosing Adult-Onset Still’s Disease Save
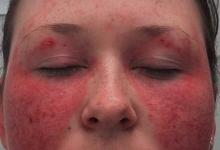
Adult-onset Still's disease is a rare systemic inflammatory disorder of unknown etiology and pathogenesis. AOSD is likely to be the adult continuum of systemic-onset juvenile arthritis and hence, frequently affects young men and women below the age of 35 years. The diagnosis is suggested by the classic triad of quotidian/spiking fevers (> 39oC), evanescent "salmon-pink" rashes, and arthritis. Other characteristic manifestations include a prodromal sore throat, arthralgias, myalgias, weight loss, serositis, hepatomegaly (often with elevated hepatic enzymes), splenomegaly and generalized lymphadenopathy. Laboratory tests support the inflammatory nature of the disorder with leukocytosis, anemia of chronic disease, hypoalbuminemia, and hyperferritinemia. Serum rheumatoid factor and antinuclear antibodies are absent.
The clinical course is marked by sporadic exacerbations of systemic inflammation and/or chronic inflammatory arthritis. There are no diagnostic clinical manifestations, serologic tests or histopathologic findings and thus, the diagnosis is one of exclusion. It may be necessary to observe persistence of fever and other characteristic manifestations for at least 6 weeks to confirm the diagnosis of AOSD.
Management of AOSD has been revolutionized in the biologic era. Inhibition of IL-1 (anakinra) or IL-6 (tocilizumab) has proven highly effective when NSAIDs, steroids and DMARDs have failed.
The scarceness of this condition may cause some difficulty in diagnosing it. I have diagnosed and managed many patients with AOSD in the last 30 years; during this span, I have seen a pattern of mistakes made when diagnosing or treating AOSD. Here are my top five:
- Making an AOSD without the requisite triad of high fever, evanescent rash and polyarthritis (never monarthritis). While few will manifest all three at presentation, the triad will be revealed in the first 3-6 months of symptoms in nearly all. All too often clinicians will diagnosis “Still’s disease” when there is an undiagnosed febrile case with several features associated with the syndrome. These patients seldom if ever have AOSD. The proper course would be to utilize the Yamaguchi or Cush Criteria for the diagnosis. My Criteria require 10 points: 2 points each for major features – quotidian fever >102F; evanescent JRA rash; simultaneous elevation of WBC >12.5 and ESR >40; seronegativity and carpal ankyloses. Minor criteria get 1 point each and include: Onset age < 35 yrs.; prodromal sore throat; serositis; RES involvement (lymphadenopathy, hepatosplenomegaly or increased LFT’s); polyarthritis; and cervical or tarsal ankyloses.
- Failure to observe/document a daily quotidian fever > 102oF. AOSD and SoJIA are circadian cytokine syndromes. Patients will reproducibly manifest the same fever (prodrome, magnitude, duration) at the same time of day – usually late night or late afternoon and never in the morning.
- Intermittent Fever History. As stated above, this is a daily febrile disorder that is distinctly different from other autoinflammatory diseases. The duration of fever is telltale and may last 1-3 days (familial Mediterranean fever, CAPs, Muckle Wells) or 5-21 days (TRAPS) or daily (AOSD, SoJIA, Schnitzler syndrome). Fevers that are intermittent, unpredictable or low grade are never due to AOSD.
- Over-emphasis on ferritin levels for diagnosis. While hyperferritinemia may be caused by iron overload, vasculitis or the macrophage activation syndrome, there is nothing specific about this finding and AOSD. Ferritin is an acute-phase reactant that is only elevated in half of patients with AOSD. In contrast, the ESR or CRP is elevated in 90% of AOSD patients. 50% of AOSD patients have an ESR >90 mm/Hg and 90% have ESR > 50 mm/Hg.
- Treatment with TNF inhibitors. There are reports of TNF inhibitors being beneficial in AOSD, but this is in the management of the chronic inflammatory arthritis that develops in up to one-third of patients. At the outset and during the inflammatory stages of the disease, features like fever, rash, serositis, LFTs, hepatomegaly and others will only be controlled by either high dose corticosteroids (1-2 mg/kg/day) or anakinra or tocilizumab. There are no head-to-head trials to instruct us which is the better agent in new onset, active inflammatory Still’s. In my experience both work, and when they don’t the other will.
REFERENCES
Cush JJ. Medsger TA Jr. Christy WC. Herbert DC. Cooperstein LA. Adult‑onset Still's disease. Clinical course and outcome. Arthritis & Rheumatism. 30(2):186‑94, 1987 Feb.
Yamaguchi M. Ohta A. Tsunematsu T. Kasukawa R. Mizushima Y. Kashiwagi H. Kashiwazaki S. Tanimoto K. Matsumoto Y. Ota T. et al. Preliminary criteria for classification of adult Still's disease. Journal of Rheumatology. 19(3):424‑30, 1992 Mar.