All News
Glucocorticoids-free zone in SLE?
For over 70 years, glucocorticoids, (GC) have been a part of standard therapy in SLE. They are classically used to not only induce remission or treat an acute flare, but also as maintenance therapy. They are a valuable 'friend' if used wisely, and can become a 'foe' if used excessively.
Read Article
Abs#518 @RheumNow #ACR23
Deodhar: TOFA in AS, by b/l CRP levels
30% nml CRP (<5 mg/L) v 70% Elevated
At wk 12, TOFA >> PBO regardless of b/l CRP
Difference in response: greater in pts w elevated CRP
Safety rates: elev. CRP c/w PBO, but nml CRP had trend of high AEs for tofa v PBO https://t.co/b9NRNkU8ub
Eric Dein ( View Tweet)
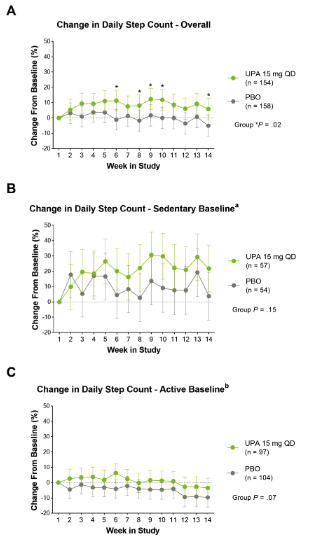
Upadacitinib on wearable device-measure activity
SELECT-AXIS 2
Abs#0530 #ACR23 @RheumNow
UPA had numerically higher mean daily step counts than PBO
11% improvement v PBO at wk 14 (diff of 345 steps/day)
Sedentary pts: 22% improvement in daily step count from b/l on UPA (4% PBO) https://t.co/Gq91TmvfZC
Eric Dein ( View Tweet)
Good Treatment review of biologics (IL-1, IL-6) in systemic JIA (Stills) including complications of #MAS and lung disease; also info on horizon therapies like JAK inhibitors and IL-18 targeting and novel biomarkers (calgranulins, IL-18 and CXCL9) https://t.co/Cbd7bKdIbb https://t.co/d9tn9fmSAy
Dr. John Cush RheumNow ( View Tweet)
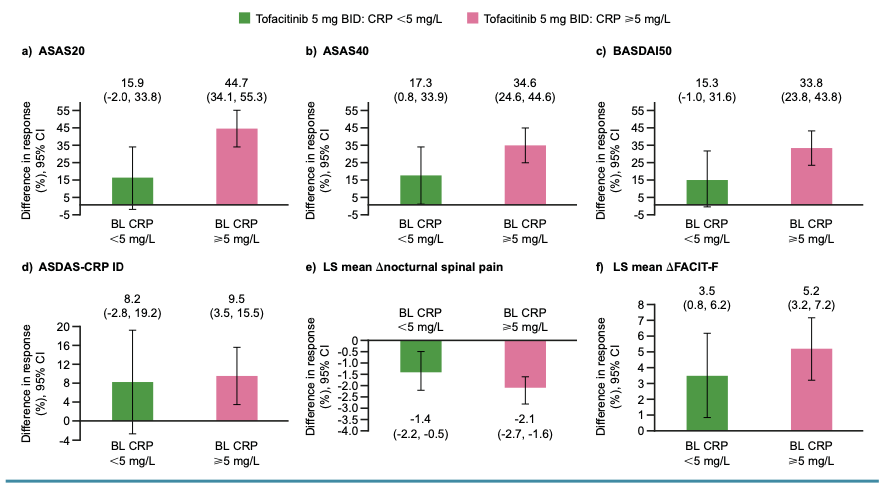
Tofacitinib efficacy and safety in axSpA pts by baseline CRP levels
Elevated CRP pts with higher response in ASAS20, ASAS40, BASDAI50, etc.
AE trended higher in normal CRP pts taking Tofa compared to placebo
@RheumNow #ACR23 Abs#0518 https://t.co/nbiD36x1Pa
Robert B Chao, MD ( View Tweet)
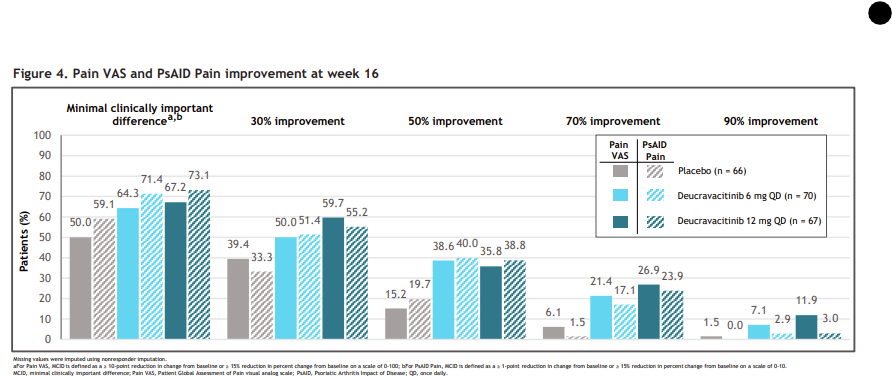
Deucravacitinib (TYK2) data has been surprisngly good in SLE
Strong rationale in PsA as well; I liked this poster & the focus on pain scores / patient QOL
Probably my #1 draft pick for "drugs I'm buying right now"
@RheumNow #ACR23 Abstr0508 https://t.co/FHNvgUrYxp
Mike Putman EBRheum ( View Tweet)

Year in Review: Dr. P Seo
Novel PsA therapy on the horizon:
⭐️Brepocitinib
➡️ Tyk-2 inhibitor: IL12/23 & type I IFN
➡️ Phase Ib, 218 pts, 8% TNFi failure
➡️ 71% on concurrent MTX
➡️ Wk 16: ACR 50/70 & PASI75/90 improved, maintained through week 52
#ACR23 @RheumNow
Meral K. El Ramahi, MD MeralElRamahiMD ( View Tweet)
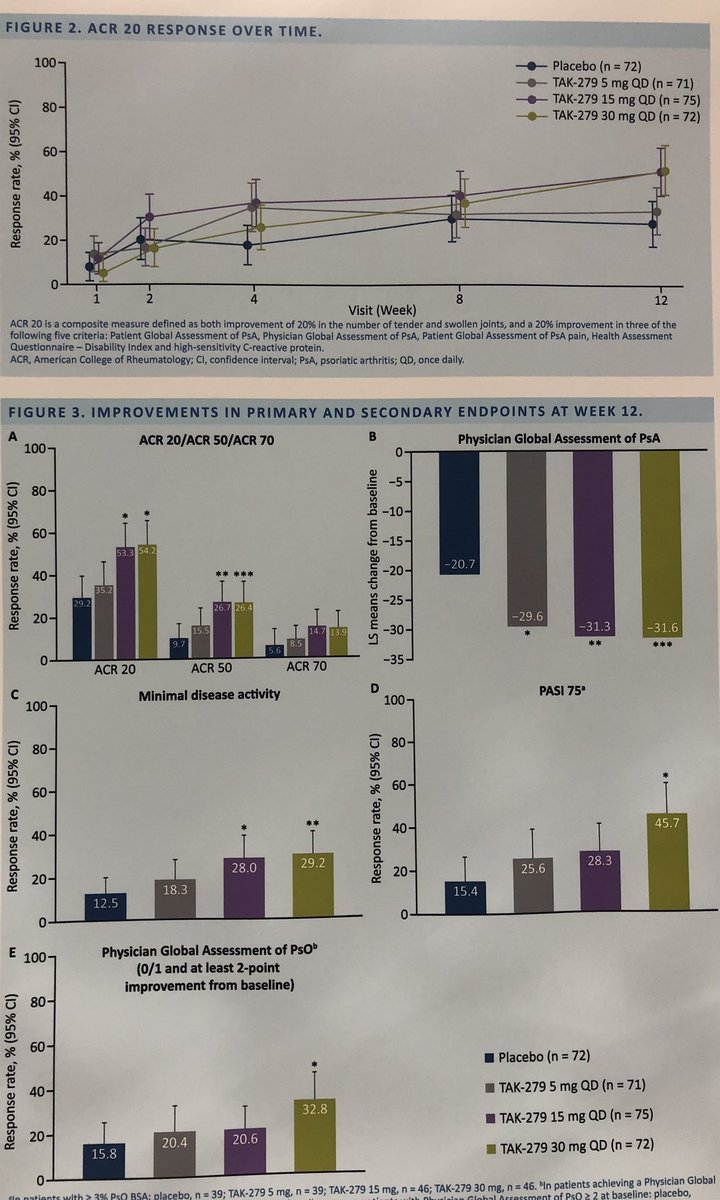
I’m not TYK’ed! Another TYK2 #TAK-279 in #PsA RCT. Yup it works in ballpark of other PsA #Rx. #PASI75 45.7%. No obvious dose response w 15 and 30 mg daily but more #acne at higher dose. #ACR23 @ACRheum @RheumNow poster L12 Where to use vs #Deucravitinib? Too early to say as Ph2 https://t.co/nMkgOlUf6s
Janet Pope ( View Tweet)
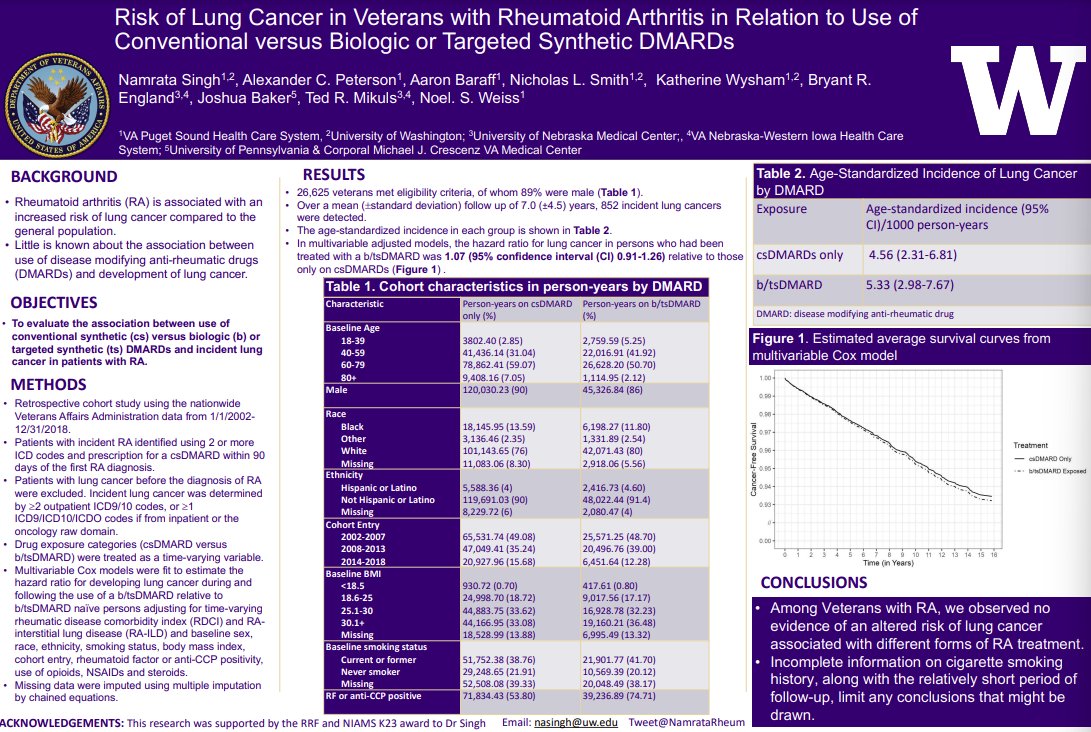
Nice VA study evaluating risk of lung cancer w/respect to RA treatment strategies
Take home? No association. Aside from the (small risk) w/JAKi's, I think malignancy risks have been mostly overblown
@NamrataRheum @RheumNow ABST0453 #ACR23 https://t.co/lDz0nV1KHt
Mike Putman EBRheum ( View Tweet)
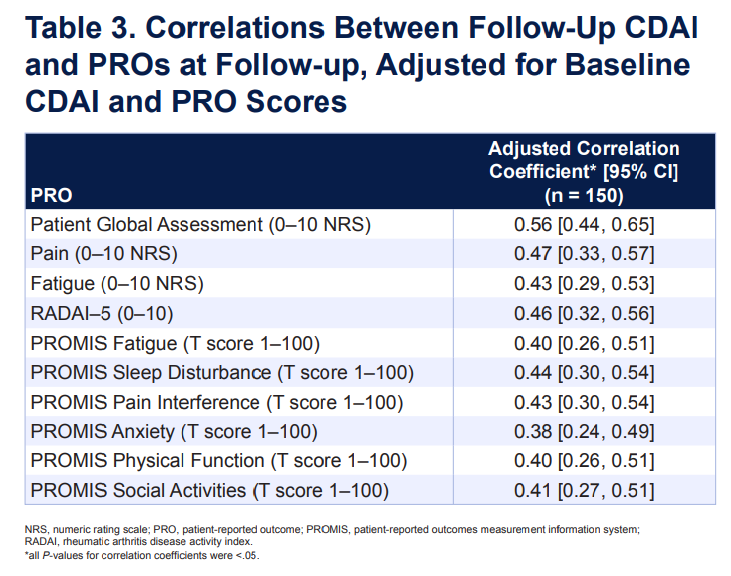
Patient reported outcomes between clinic visits: worth doing?
RA pts starting ADA/UPA, n=150
ArthritisPower/PatientSpot app for PROs between visits
52% of CDAI change explained by PROs
Maybe a helpful tool in prioritising RA clinic reviews?
@RADoctor #ACR23 ABST0380 @RheumNow https://t.co/oTttAlIxQR
David Liew drdavidliew ( View Tweet)
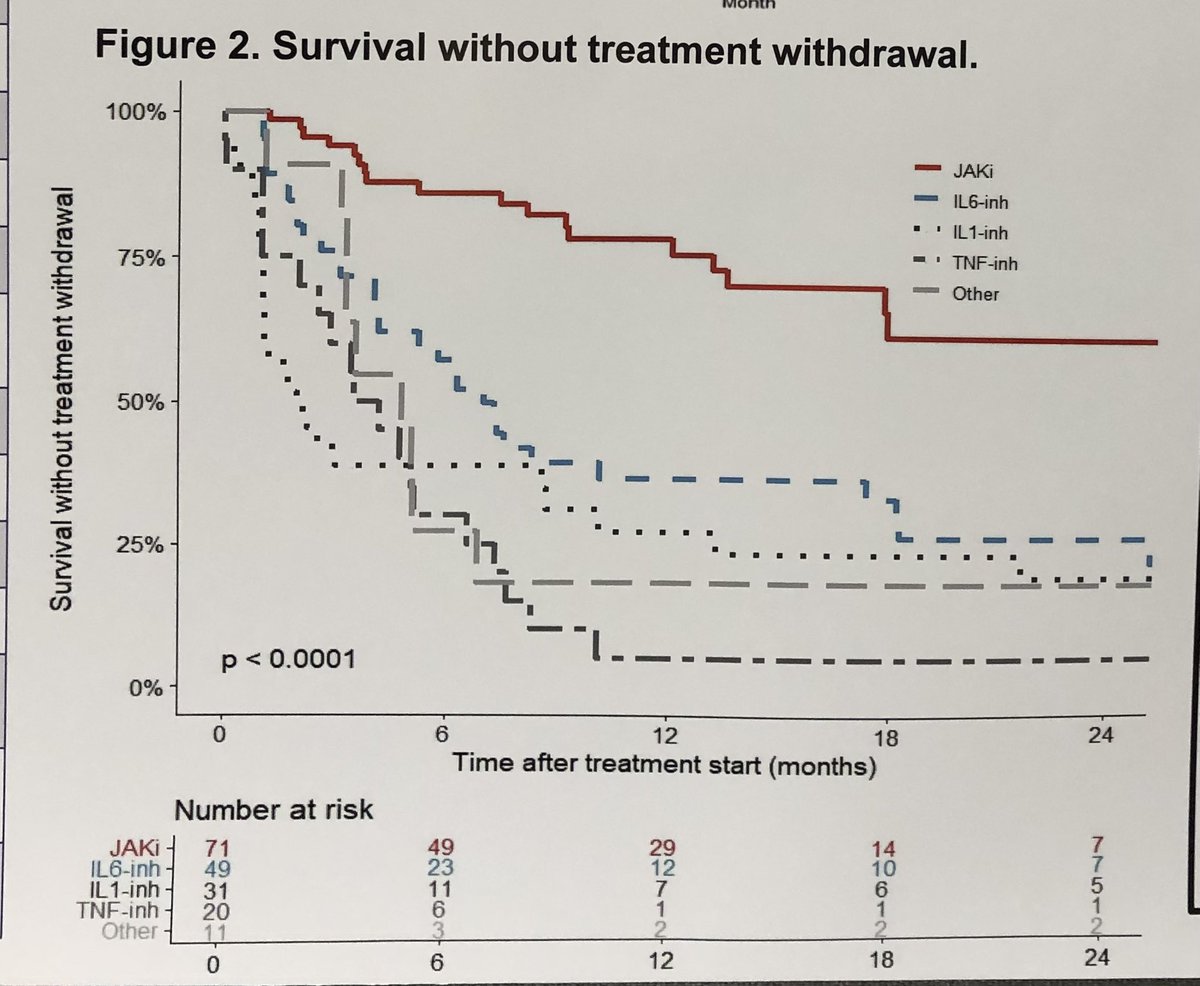
Who knew? VEXAS =cluster of findings from a somatic mutation N=110 studying retention of advanced Rx. #JAKi had far better retention than other #Rx. Although there could be channeling bias, I am impressed! Access for off label is a different issue #L03 #ACR23 @RheumNow @ACRheum https://t.co/RE4BVdZeWt
Janet Pope ( View Tweet)
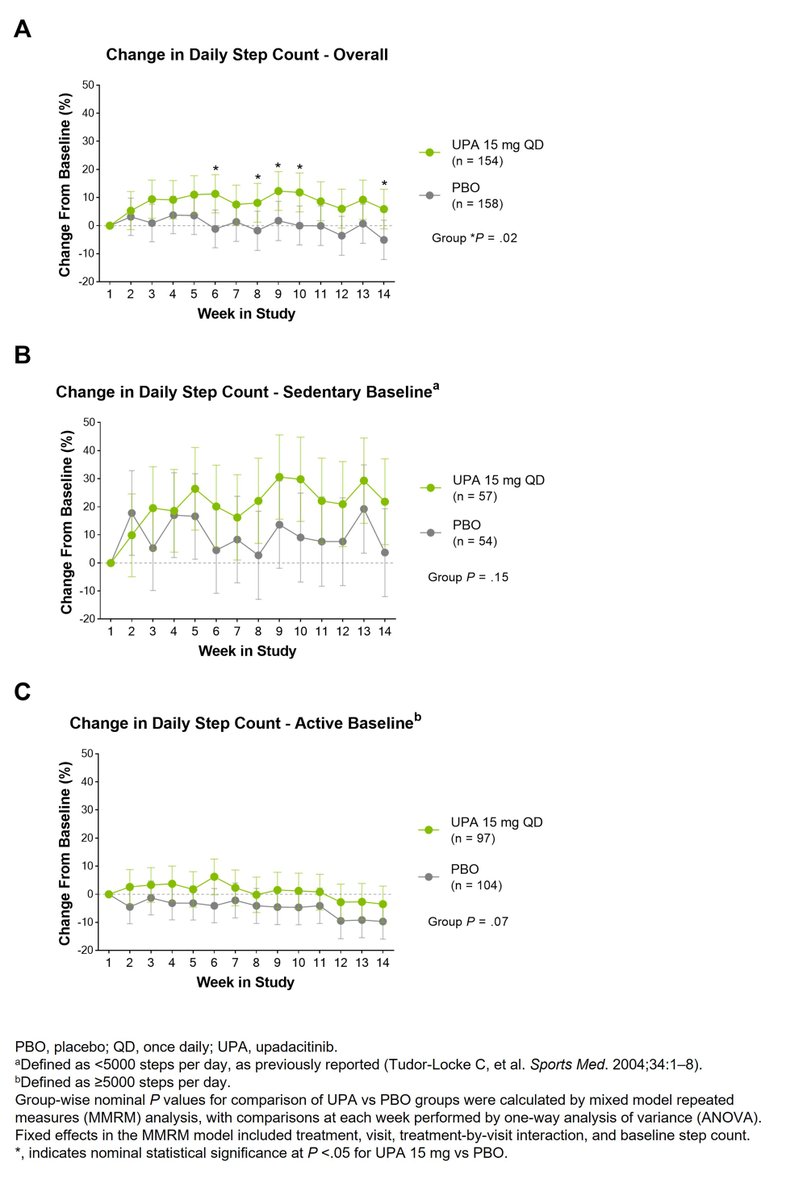
In bDMARD-IR AS patients, UPA led to numerically greater improvements vs PBO in physical activity as measured by a wearable device over 14 wks, especially in sedentary patients. #ACR23 Abs #0530 https://t.co/6Me2XctK6D @rheumnow https://t.co/c6E2GfAGt4
Dr. Rachel Tate ( View Tweet)

Join us tonight at 6pm PT/ 9pm ET for our daily #ACR23 recap. https://t.co/0RDwTdzhwS
Dr. John Cush RheumNow ( View Tweet)
Good Treatment review of biologics (IL-1, IL-6) in systemic JIA (Stills) including complications of #MAS and lung disease; also info on horizon therapies like JAK inhibitors and IL-18 targeting and novel biomarkers (calgranulins, IL-18 and CXCL9) https://t.co/ACe7nDDwop https://t.co/lV66WerkAp
Dr. John Cush RheumNow ( View Tweet)

Oral Surveillance Study Alters Practice at VA
Safety risks found in a postmarketing trial with the JAKi tofacitinib (Xeljanz) appear to have influenced prescribing patterns across the class for RA patients in the VA health system, researchers found.
https://t.co/6WktHCkrI1 https://t.co/8wpAeLsBbw
Dr. John Cush RheumNow ( View Tweet)
H. Zoster Subunit Vaccine Efficacy with JAK Inhibitor Therapy
Two recent reports suggest variable efficacy when JAK inhibitor (JAKi) treated patients are vaccinated with the recombinant herpes zoster subunit vaccine (RZV).
https://t.co/QEPQJkfSjE https://t.co/pFk2mF22ex
Dr. John Cush RheumNow ( View Tweet)

Analysis of German RABBIT registry did not show more MACE events in pts w/ JAK inhibitors compared to other DMARDs. 154 MACE w/ 14203 Rx episodes (21218 Pt-Yrs). IRs were 0.68 JAKi, 0.62 TNFi, 0.76 bdMARDs and 0.95 csDMARDs; higher in CV risk pts https://t.co/luUK9M9IM9 https://t.co/z8lxjWscCR
Dr. John Cush RheumNow ( View Tweet)
Metanalysis of 26 studies (2252) pts w/ HBsAg-/HBcAb+ RA treated with b/tsDMARDs, shows the pooled HBV reactivation rate was 2.0%
HBV reactivation higher w/ RTX (9%), ABA (6%), JAKi (1%); none w/ IL-6i or TNF-i
More reactivation if pt is HBsAb- (OR=4.56) https://t.co/V60nkUSpjj https://t.co/jnZKnY0Zuk
Dr. John Cush RheumNow ( View Tweet)
Late Should Not Be Less (11.3.2023)
Dr. Jack Cush reviews the news, journal reports and regulatory approvals from the past week on RheumNow.com.
Read Article
Cardiovascular and VTE Risk w/JAKi Treatment of Skin Disorders
A JAMA systematic review and meta-analysis has shown the use of JAKi in immune-mediated inflammatory skin diseases was not associated w/ increased risk of all-cause mortality, MACE, or VTE.
https://t.co/XYAeLnFvHr https://t.co/tGRNEUEZj9
Dr. John Cush RheumNow ( View Tweet)


