Knee Replacement and the Physical Terrorist Save
In June 2011 I had both knees replaced by a wonderful team of health care specialists. Below is a reprise of emails that I distributed weeks after my surgery. I believe these recollections to be instructive to both rheumatologists and patients considering joint replacement.
I had the proverbial "bone-on-bone" osteoarthritis knee damage for nearly 20 years. Pain, limited mobility and time convinced me that bilateral knee replacement surgery was smart thing to do. I selected a great team – a highly experienced orthopedist, a very smart internist/hospitalist, a great hospital and physical therapy department and a home physical therapist. I underwent uneventful and expedient surgery (was on the operating table for 2 hours). I awoke in the recovery room, disoriented and mumbling incoherent curses. However within hours they had me standing bedside, with two burly therapists holding me up on my two new magic legs (like Lieutenant Dan) - I felt like a marionette, but I had no pain. I knew immediately, this was a good move. I joined the chorus of other inmate knee replacers in proclaiming, "Damn, I should have done this years ago". 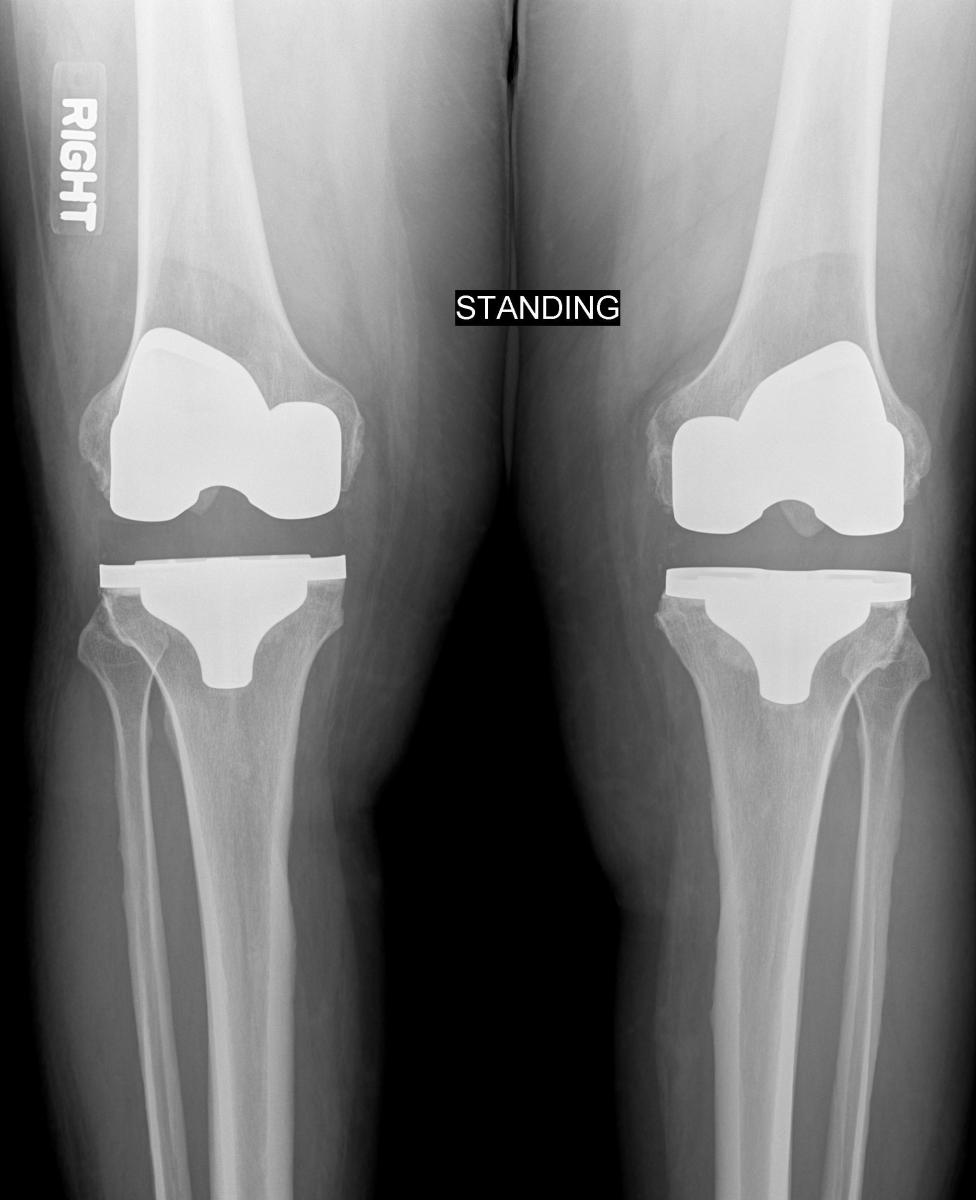
I was in the hospital for three days, during which I struggled with blood loss, anemia and a whiter shade of pale along with narcotic meds that turned me into a pet rock. Early on, I was hardly a good hospital visit - people came, spoke, joked and questioned - yet I was oblivious and only capable of cartoons and NBA playoffs. Once my crack-staff “A” team physicians noticed I was unable to distinguish between Labron James and Wylie Coyote, a much-needed transfusion and change to tramadol allowed me to resume my inpatient rehabilitation.
A week in the rehab unit taught me that hard work, pain, a goniometer and a team of nurse Ratchet physical therapists could be the new formula for Guantanamo progress. I was standing the day after surgery, walking with a walker on post-op day two, and left the rehab unit with 100 degrees of flexion and quarter-mile (400 yards) snail speed endurance on a walker. I was discharged home 10 days after surgery.
The elation of going home was quickly squelched by my new nemesis, the Darth Vader to my recovery quest - my home physical therapist. Her name was PT Pam, with PT standing for physical terrorist. I actually chose her based on the recommendation of my orthopedist and her reputation. Pam was the real deal, the best at what she does. She daily declares she loves her job, love for her patients and even more, love for having invincible doctors as the focus of her attention. As best I can tell, it appears that her job is to turn rusty, broken windmill beings like me into Gumby or Spiderman with a mere 4 weeks of reimbursable home PT. She took no prisoners and daily had me whimpering like I did when I learned that Wham broke up. After her first day, she had my knee flexion up to 115 degrees, with her goal being >150 degrees and no crying. Apparently there is no crying in physical therapy. I told her, I’m a rheumatologist; I’m in the “biz” and argued such a goal was "insane and impractical". However, these were words of inspiration to Pam, words I probably should not have uttered.
The first week I used a walker. The second week I was on crutches and then a cane for a few days. Soon after, walking without assistance was achieved and my knee flexion did surpass 150 degrees. She did this with a set of floor pedals (to mimic a bike), a wall or fridge to slide up and down on and a roll log of towels that, when strategically placed, can bend the knee in either direction and to unnatural extremes. Hence I was ecstatic at 150 degrees, but that wasn't enough for my physical terrorist. She upped the target of my IQ and knee flexion to 160 degrees. Most would agree that neither of these were likely.
Home physical therapy yielded shocking and painful progress. But it was my saving grace and dwarfed the progress achieved during inpatient PT. Humbling home PT has taught me how difficult self-care can be – the shower, toilet, couch, car and many modern amenities were enemies as we started PT. Physicians don't make good patients. We know too much (and too little), we don’t like taking orders (the best advice money and insurance can buy) and we too hate taking medicines. However, as KevinMD says, becoming a patient may be the best kind of medical education.
Through surgery and physical therapy, I earned my mobility and lost my pain. Sure I had pain while doing PT designed to make prisoners confess, but most of the time I had little pain. (Editor’s note: pain after surgery is actually common for most and may be related to other damage to that not replaced or repaired by the surgery, such as tendons and ligaments). Twenty-five days after surgery I went to a concert and sat in a balcony box. I enjoyed the wonderful show and performance. During the show, I was able to get up, stand and stretch. I stood upright in the dark, without cane or crutch and without moving for almost 10 minutes. I stopped enjoying the show and instead enjoyed the fact that I could stand without pain and without moving, shifting, fidgeting, etc. This is one of many moments that reaffirmed my knee replacements were a life-changing decision. I returned to work five weeks after surgery, flew on an airplane at 8 weeks, danced at 12 weeks and walk/jogged a 5K Turkey Trot at Thanksgiving (22 weeks later).
My knee OA dates back to my high school football knee injury and meniscal removal and has been x-ray bad since 1992. Hence, I've had nearly 20 years of compensating for structural damage and adopted some very funky ways of walking, using stairs and getting around. One of the untold post-operative challenges was UN-learn these protective but awkward habits. Again, PT Pam was there to teach and guide as I figured out how move, climb and two step like normal folk.
The process begins when pain and immobility collides with the loss of control and fear of surgery. This is the time to step forward, not backward. This is when you need to seek knowledge, clarity and the right people to turn your knees and life around. My advice to my patients is 1) talk to others who have had the surgery; 2) Pre-Hab: months of (lower extremity) exercise are needed to ensure that your rehab is productive (if you can’t walk before surgery, you won’t be able to walk after surgery); 3) consult an orthopedic surgeon long before you even think surgery is necessary (because your pain will escalate to unbearable; when is unknown but in most, it comes quickly and unexpectedly); and 4) you must have a physical therapist who will guide and teach you after surgery. The number of weeks and frequency of sessions may vary, but the person(s) who will make you achieve your unthinkable goals is your physical therapist, not the doctor. Lastly, you need to appreciate the love and support of family and friends who will cheer, sustain and listen to you as you learn how to rebuild a new you.









