Throw Me Rope Save

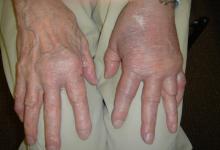
A gal with rheumatoid arthritis moved to my town and has transferred her care to me. Despite having RA for 3 years and swollen joints at the last three visits, she has taken surprisingly few effective drugs thus far.
On this visit I declared my concerns for her future health, especially if we didn’t make significant changes in therapy. So I recommended she start a new drug. She asked several good questions about how it’s taken, the side effects, and the long term effects. After mulling this over, she said she wanted to go home and think about this further and she would get back to me with her decision.
But wait, that’s what she said at her last visit 2 months ago! The modern caring physician is supposed to educate and engage in shared decision making to ensure patient satisfaction or commitment. While that may work well with many, there may be some who want the physician to choose for them. But there are many who will delay decision making out of fear of what they don’t know or understand.
It’s quite natural to not act when you don’t know what to do. The problem is that in many such circumstances, doing nothing is likely to be the wrong choice.
Why?
First, the fork in the road exists for this reason. The sage catcher Yogi Berra once said, “When you come to a fork in the road, take it”.
Second, as the one responsible for guiding good decisions and ensuring optimal outcomes, it would be wrong for the physician healer to allow an intellectual timeout or declare a draw until the next visit.
The no-choice, wrong-choice easily stands out, as it usually portends a downward turn for most; and RA is a progressive disorder in most.
Imagine you’re boating and come up on a man whose boat has capsized. He is stranded in the lake and treading water to stay afloat. He's obviously struggling, looks to you for help and you are there, able and capable of throwing him a rope. So you throw the rope, and await his grasp that will pull him from the sinking waters.
But wait, you’re a total stranger! He anguishes if he can trust you? He panics, reconsiders, over thinks, and under acts. Maybe he should wait or maybe he could try and swim to the distant shore.
How does he know that your rope is a sure thing? Are you ready to spell out the guarantees to your guidance?
This is indecision gone wrong.
Indecision is often fueled by fear of the unknown, past indecisions or past mistakes, and doom and gloom television advertisements. The waffling patient’s best defense is to declare something from the faceless “they said” people.
It would be good to know if this inner voice represents uncertainty, anxiety or fear. Uncertainty cannot be solved by Dr. Google, anxiety is an anchor tied to wrong choice and fear is only useful if you’re about to take flight. Education, reassurance and speaking from your strengths and experience may engage the disengaged patient.
Patients may come to you for the answer (a rope) or specific guidance (a map). It’s not enough for you to know the solution, be the answer man and write the prescription. First, you will always need to establish trust, set goals and offer hope.
If you don't first establish trust and provide the map (guidance, goals, hope), throwing the rope may be what the doctor ordered but not what the patient buys into.
It's impossible to read a patients mind or motivations, especially early in their care. But it is possible to understand their apprehensions through effective listening and communication,
Nevertheless, there may come a point when you will need to challenge the indecisive patient and say that not making the decision is certainly more harmful than choosing one of the options offered.
Put another way, the indecisive patient is more likely to be harmed by fear, than from what they are most fearful of.
“He who deliberates fully before taking a step will spend his entire life on one leg.” ~Chinese Proverb




If you are a health practitioner, you may Login/Register to comment.
Due to the nature of these comment forums, only health practitioners are allowed to comment at this time.