CRP in SSc: Identifying a Severe Phenotype Save
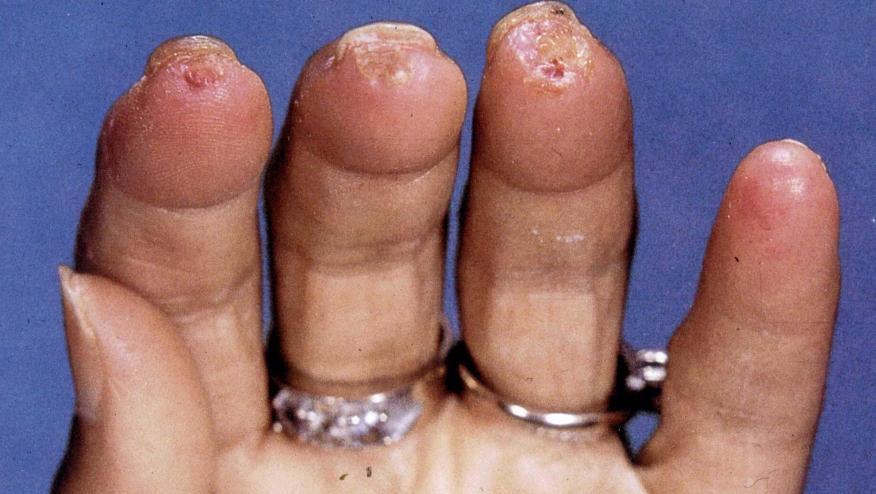
Patients with systemic sclerosis (SSc) who have persistent inflammation -- characterized by consistently elevated levels of C-reactive protein (CRP) -- have more severe disease and worse outcomes, a retrospective study confirmed.
In a cohort of 131 patients, those with the inflammatory phenotype of SSc had significantly higher rates of pulmonary fibrosis than those with noninflammatory SSc (83% vs 42%, P<0.001), reported Florian Kollert, MD, of University Hospital Bern in Switzerland, and colleagues.
Patients in the inflammatory group also more often had cardiac arrhythmias (25% vs 5%, P=0.048), according to the team's study online in Arthritis Research & Therapy.
"The pathogenesis of SSc is thought to involve an initial inflammatory phase, characterized by a Th1- and Th17- immune response, which is followed by a switch to Th2, leading to irreversible fibrosis and a 'burn-out' of the disease," the researchers wrote. However, they found, a subgroup of SSc patients have persistently high levels of the acute-phase reactant CRP and severe disease, whereas others never show elevations of the inflammatory marker.
Treatment for SSc remains challenging, particularly for those with worse disease, who are susceptible to adverse effects with powerful immunosuppressives. There have been reports of treatment-related mortality of up to 10%, the team noted.
Therefore, to investigate the patterns of CRP longitudinally and examine whether the inflammatory marker correlates with disease features, comorbidities, and responses to treatment, the researchers reviewed the charts of all patients seen at University Medical Center Freiburg in Germany from 1997 to 2015.
Patients were classified as inflammatory if their CRP levels were 5 mg/L or higher at more than 80% of clinic visits (18.3% of the patients) and noninflammatory if CRP levels were normal at all visits (29%). All other patients (52.7%), whose CRP levels were elevated at fewer than 80% of visits, were considered intermediate.
During 7.6 years of follow-up, the 131 patients had 1,815 consecutive clinic visits.
Compared with the noninflammatory subgroup, the inflammatory group more often were older and male, and had these disease features:
- Anti-Scl-70 antibodies: 67% vs 32% (P=0.009)
- Diffuse cutaneous SSc subtype: 67% vs 37% (P=0.036)
- Higher Rodnan skin scores: 18 vs 7 (P<0.001)
- Lower forced vital capacity: 76% vs 102% (P<0.001)
- Lower total lung capacity: 76% vs 92% (P=0.001)
- Lower diffusing capacity: 57% vs 83% (P=0.008)
In addition, the annual decline in forced vital capacity was more pronounced in the inflammatory subgroup.
The patients with the inflammatory phenotype also were more likely than the noninflammatory group to have received immunosuppressive treatment (79% vs 37%, P=0.002).
While there was no difference in CRP levels between the first and last treatment visits in the noninflammatory group (3.2 vs 3.1 mg/L), CRP levels actually were slightly higher at the last visit in the inflammatory group (13.2 mg/L vs 9.5 mg/L, P=0.017), the researchers said.
When they compared the intermediate phenotype patients with the noninflammatory group, they found higher body mass index, more coronary artery disease, and a more rapid decline in forced vital capacity.
And when the investigators compared the intermediate group with the inflammatory group, they found lower Rodnan skin scores (10 vs 18), less pulmonary fibrosis (42% vs 83%), higher forced vital capacity (92% vs 76%), higher total lung capacity (86% vs 76%), and a lower frequency of anti-Scl-70 antibodies (36% vs 67%, P≤0.05 for all).
As in the noninflammatory group, there were no differences in CRP levels between baseline and the final visit for the intermediate group (3.4 vs 3.5 mg/L).
A total of 29 patients received treatment with cyclophosphamide during follow-up. Among those patients overall, no changes in CRP levels were seen (4.7 vs 7.6 mg/L), and even for cyclophosphamide recipients with the inflammatory phenotype, no decrease was apparent (18 vs 17.7 mg/L).
The authors called the finding that cyclophosphamide treatment failed to lower CRP levels "surprising, as cyclophosphamide is one of the mainstays of SSc treatment, and theoretically, CRP levels should decline after such a potent B and T cell-targeted treatment."
"Presumably, other cell types less affected by cyclophosphamide, like macrophages, might explain these findings," Kollert and colleagues continued, noting that macrophages play a central role in the inflammatory and fibrotic processes of SSc.
"These findings underscore the heterogeneity of the disease and emphasize the importance of defining subgroups in SSc, which potentially can guide treatment decisions," the team concluded.
Limitations of the study, the researchers said, included its retrospective design and the relatively small sample sizes in the subgroups.
The authors reported no financial conflicts.









If you are a health practitioner, you may Login/Register to comment.
Due to the nature of these comment forums, only health practitioners are allowed to comment at this time.