Hepatitis C-Related Cryoglobulinemic Vasculitis Save
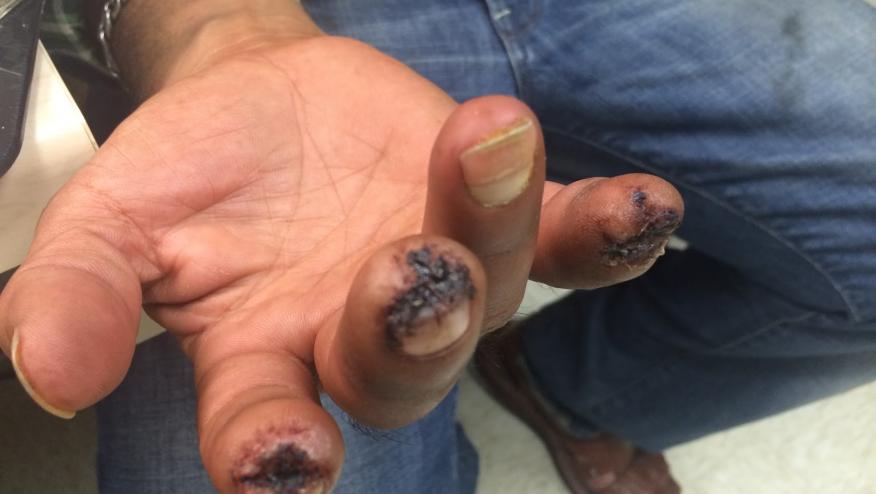
Flares of vasculitis can still be a problem after hepatitis C-related cryoglobulinemic vasculitis patients are cured of their hepatitis C by direct-acting antivirals, as demonstrated by data from four registries presented at ACR 2019 in Atlanta, Georgia.
Direct-acting antiviral therapy has raised the prospect of a safe and effective cure for millions of hepatitis C patients worldwide. Many of these patients have suffered from cryoglobulinemic vasculitis as a consequence of their viral hepatitis, and there had been understandable hope that a cure for their hepatitis C might mean a cure for their vasculitis.
Mohamed Tharwat Hegazy, of Cairo University in Egypt, presented combined data addressing this from four large hospital registries: two from Cairo University, Hopital La Pitié Salpêtrière in Paris, and Sapienza University in Rome. This examined 1019 cryoglobulinemic vasculitis patients who received directly-acting antiviral therapy only for their hepatitis C between 2015 and 2019, and followed them for 24 months.
While all of these patients achieved a sustained viral response (SVR), during the follow-up period 116 patients (11.4%) had flares of vasculitis despite remaining negative for hepatitis C by PCR. Of these, 98 had renal flares, with purpura and peripheral neuropathy also common.
This result casts doubt over any hope that cryoglobulinemic vasculitis might be cured after the corresponding hepatitis C is. It also follows work from the some of the same authors published last year, which concerningly showed that cases of de novo vasculitis can develop even after SVR induced by directly-acting antiviral therapy. The authors postulated that this is most likely due to autonomous B cell proliferation, evidenced by increased expression of BAFF and APRIL continuing several months after successful hepatitis C therapy finishes. Alternatively, they suggested that B cells might be triggered by environmental factors, or that persistence of low numbers of intracellular HCV RNA might be sufficient to cause vasculitic relapse.
Whatever the mechanism, this result appears to mandate that hepatitis C-related cryoglobulinemic vasculitis patients are monitored under the direction of their rheumatologists for many months after their hepatitis C is cured.
Nephron. 2018;140(4):275-281. doi: 10.1159/000493807. Incidence and Characteristics of de novo Renal Cryoglobulinemia After Direct-Acting Antivirals Treatment in an Egyptian Hepatitis C Cohort. Fayed A, El Nokeety MM, Samy Abdelaziz T, Samir HH, Hamza WM, El Shabony T. https://www.ncbi.nlm.nih.gov/pubmed/30359992
EBioMedicine. 2018 Sep;35:106-113. doi: 10.1016/j.ebiom.2018.08.007. Increased genomic instability following treatment with direct acting anti-hepatitis C virus drugs. Hegazy MT, Allam WR, Hussein MA, Zoheir N, Quartuccio L, El-Khamisy SF, Ragab G; Mediterranean Consortium for the study of Cryoglobulinemic Vasculitis https://www.ncbi.nlm.nih.gov/pubmed/30139628










If you are a health practitioner, you may Login/Register to comment.
Due to the nature of these comment forums, only health practitioners are allowed to comment at this time.