Inflammatory Arthritis Variants with Checkpoint Inhibitors Save
Two recently published studies have demonstrated distinctive patterns of rheumatic complaints in patients treated wtih immune checkpoint inhibitors (ICIs).
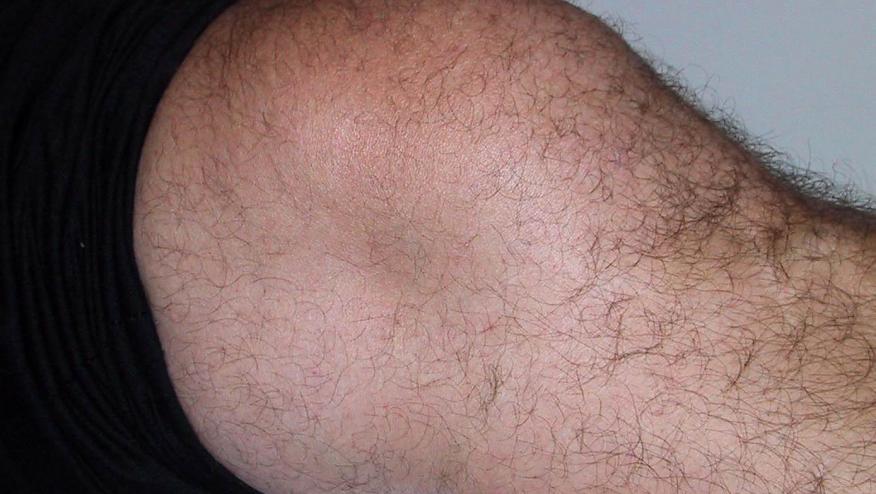
Capelli and colleagues have studied patients treated with ICIs and found two variants of inflammatory arthritis (IA) - a reactive arthritis like large joint arthritis with combination ICI therapy or a small joint IA with ICI monotherapy.
Inflammatory arthritis (IA) is of several immune-related adverse event (irAE) seen with ICI therapy.
They identified 30 patients with combination ICI therapy who primarily presented with knee arthritis, with high C-reactive protein levels, a prior irAE, and show a a reactive arthritis-like phenotype.
By contrast, those treated with ICI monotherapy were more likely to have initial small joint involvement and to have IA as their only irAE.
Ten patients required additional immunosuppression beyond corticosteroids, with TNF-inhibitors and/or methotrexate. Those on TNF inhibitors did not show tumor progression.
Another French cohort study described the two rheumatic variants in 35 (6.6%) of their 524 ICI treated patients. (Citation source: https://buff.ly/2HV9msa)
All but one of the rheumatic irAEs occurred with anti-programmed cell death protein 1(PD-1)/PD-1 ligand 1(PD-L1) antibodies, with a median exposure time of 70 days.
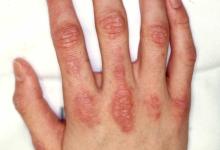
Patients either exhibited IA that mimicked rheumatoid arthritis (n=7), polymyalgia rheumatica (n=11) or psoriatic arthritis (n=2) or they demonstrated non-inflammatory musculoskeletal conditions (2.8%; n=15).
IA patients required glucocorticoids, and methotrexate was started in two patients.
Non-inflammatory disorders were managed with non-steroidal anti-inflammatory drugs, analgesics and/or physiotherapy.
They noted that those with rheumatic irAEs had a higher tumour response rate compared with patients without irAEs (85.7% vs 35.3%; P<0.0001).









If you are a health practitioner, you may Login/Register to comment.
Due to the nature of these comment forums, only health practitioners are allowed to comment at this time.