Lower Mortality Results from Lower Activity in Lupus Save
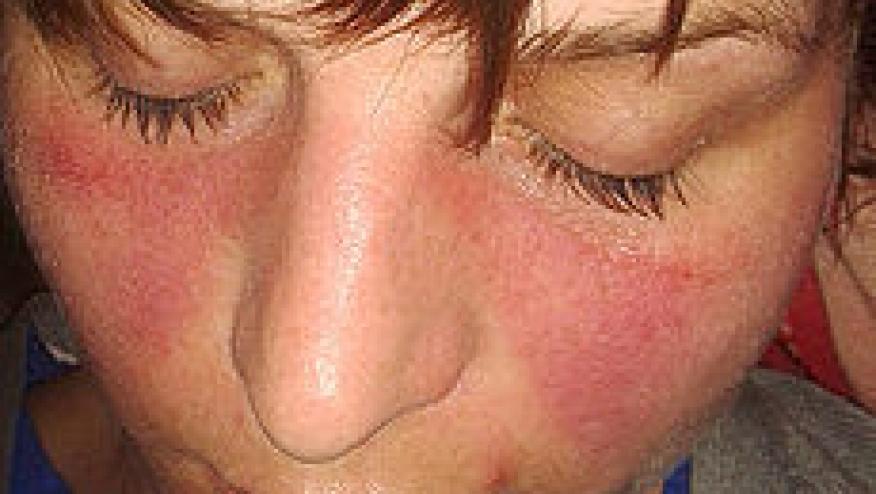
Data from the longitudinal Tromsø Lupus Cohort study has shown that lupus patients who achieve a Lupus Low Disease Activity State (LLDAS‐50) were shown to have significantly less severe damage, and a reduction in mortality.
This was a population‐based study of SLE patients in the northern‐most counties of Norway.
They collected data on the LLDAS; defined as:
- SLEDAI‐2K ≤4, with no activity in major organ systems
- no new features of lupus disease activity
- current prednisolone (or equivalent) dose ≤7.5 mg daily, and,
- well tolerated standard maintenance doses of immunosuppressive drugs.
They followed a total of 206 SLE patients 84% female) with a median follow up of 125 months. Overall there were 46 (22%) deaths.
Prednisolone (89%) and hydroxychloroquine (59%) were the most common drugs used and only 3.4% required cyclophosphamide or rituximab. A positive anti-nuclear antibody (ANA+) was evident in nearly all (96%).
LLDAS (any duration) was achieved by 74% of the cohort. The median time in LLDAS was 34 months and 69 patients (33.5%) spent at least half of their time in LLDAS.
Lower mortality rates and a lower risk of severe damage was seen in the 69 patients (33.5%) who spent at least half of their follow up time in LLDAS.
The LLDAS‐50 was associated with a significantly lower in risk of having severe damage (HR 0.37; 95%CI 0.19 – 0.73, p < 0.01), and also a reduction in mortality (HR 0.31; 95%CI 0.16 – 0.62, p < 0.01).
Treat to target and measure of low activity can have a powerful effect on lupus outcomes.










If you are a health practitioner, you may Login/Register to comment.
Due to the nature of these comment forums, only health practitioners are allowed to comment at this time.