Serum Interferon Predicts Lupus Flares Save
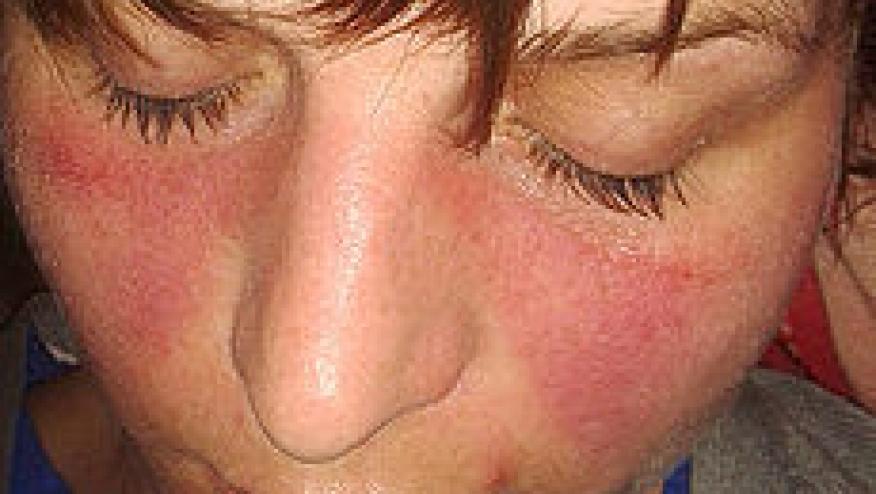
Elevated serum levels of interferon-α among patients whose systemic lupus erythematosus (SLE) was in remission helped predict future disease flares, European researchers found.
Among 254 SLE patients who were in remission, 26% had abnormally high serum levels of interferon-α at baseline, according to Alexis Mathian, MD, of Pitié-Salpêtrière Hospital in Paris, and colleagues.
In a multivariable analysis, those abnormal levels were independently associated with a fourfold higher risk of a disease flare within the following year (HR 4.0, 95% CI 1.7-9.6, P=0.002), the researchers reported in their study online in Annals of the Rheumatic Diseases.
The achievement of remission has become a primary goal of treatment for SLE, as this has been demonstrated to help decrease disease damage and minimize the risk of relapse. Many definitions of remission have been proposed in SLE, with one international consensus group having suggested a definition that includes an SLE Disease Activity Index (SLEDAI) score of zero plus normalization of laboratory features such as anti-double stranded (ds)DNA antibodies and complement. However, those laboratory measures of disease activity have not been found to be reliable for prediction of flares.
"Many authors consider the dysregulation of interferons, especially interferon-α, to be a central cause of the immunological abnormalities observed in SLE," Mathian and colleagues explained.
Previous efforts to include measurements of interferons in disease assessment have been hampered by the need to rely on the expression of interferon-stimulated genes, but the required technology has not been standardized and is not routinely available in clinical practice. However, a new digital immunoassay that permits direct quantification of interferon-α has been developed to address those obstacles.
Accordingly, to explore the possibility of improving disease prognosis by including interferon measurement in remission assessment, the researchers conducted a study from 2014 to 2017 at the National Referral Center for SLE in Paris.
For the purposes of analysis, patients were categorized as follows:
- Complete remission off treatment, which required a SLEDAI score of zero, no use of corticosteroids or immunosuppressives, and no anti-dsDNA autoantibodies or decrease in complement present, whereas clinical remission off treatment was defined as a SLEDAI score of zero and no steroids or immunosuppressives being used, but anti-dsDNA antibodies and/or low complement were present
- Complete remission on treatment required a SLEDAI score of zero and no anti-dsDNA or low complement, but prednisone in dosages of 1-5 mg/day and immunosuppressives were used, while clinical remission on treatment was similar except anti-dsDNA and/or low complement was detected
Among the 254 patients in remission, 33.9% were in complete remission off treatment, 23.2% were in complete remission on treatment, 18.5% were in clinical remission off treatment, and 24.4% were in clinical remission on treatment.
The duration of remission was less than a year in 26.3% of patients, 1-5 years in 39.8%, and more than 5 years in 33.9%.
The highest rate of elevated levels of interferon-α was observed in patients in clinical remission on treatment (41.9%) and in clinical remission off treatment (38.3%) vs 16.3% of those in complete remission off treatment.
A total of 250 of these patients in remission were followed for a year and were included in the analysis. Flares developed in 9.6% of patients, at a median time of 141 days, and 37.5% of the flares were considered severe.
On an unadjusted analysis, with the cutoff for interferon-α positivity being 136 fg/mL, the following factors were found to be associated with risk of relapse:
- High interferon-α, HR 5.5 (95% CI 2.4-12.5, P<0.0001)
- Low complement, HR 3.7 (95% CI 1.6-9.1, P=0.003)
- Prednisone dosages of 1-5 mg/day, HR 3.2 (95% CI 1.4-7.5, P=0.007)
- Positive anti-ribonucleoprotein antibodies, HR 3.1 (95% CI 1.4-7.0, P=0.006)
Factors associated with a decreased risk included age below 40 (HR 0.4, 95% CI 0.2-0.9, P=0.02) and disease duration less than 10 years (HR 0.2, 95% CI 0.1-0.6, P=0.003). Duration of remission also appeared protective, with an HR of 0.6 (95% CI 0.5-0.8, P=0.0002) for each year of remission, which was "not surprising," Mathian and co-authors noted.
In the multivariate analysis, only abnormal interferon-α levels and duration of remission remained independently associated with flare risk.
The persistent presence of interferon-α may not merely be a marker of disease activity during apparent remission, but also may play a pathologic role in the disease. "Interferon-α overexpression could be an explanation of chronic fatigue, depression, and reduction of sleep secondary to the stimulation of the dopamine metabolism by interferon-α in the central neurological system," the authors suggested.
Interferon-α also may participate in some of the processes linked with the accelerated atherosclerosis seen in SLE, such as endothelial cell damage. "These data suggest that for patients in clinical remission, return of serum interferon-α to normal values could become one of the objectives of treatment," the team concluded.
A limitation of the study was the lack of information on patients' ethnicity, which can influence interferon-α levels, the researchers said, adding that the findings also need to be confirmed in other cohorts.
The study was funded by the Assistance Publique-Hopitaux de Paris, Institut National de la Sante et de la Recherche Medicale, Sorbonne Universite, the French Arthritis Foundation, the Societe National Francaise de Medecine Interne, and the Fondation pour la Recherche Medicale.
The authors reported no financial conflicts.





If you are a health practitioner, you may Login/Register to comment.
Due to the nature of these comment forums, only health practitioners are allowed to comment at this time.