Tumor Necrosis Factor Inhibitors Do Not Increase the Risk of Cancer Recurrence Save
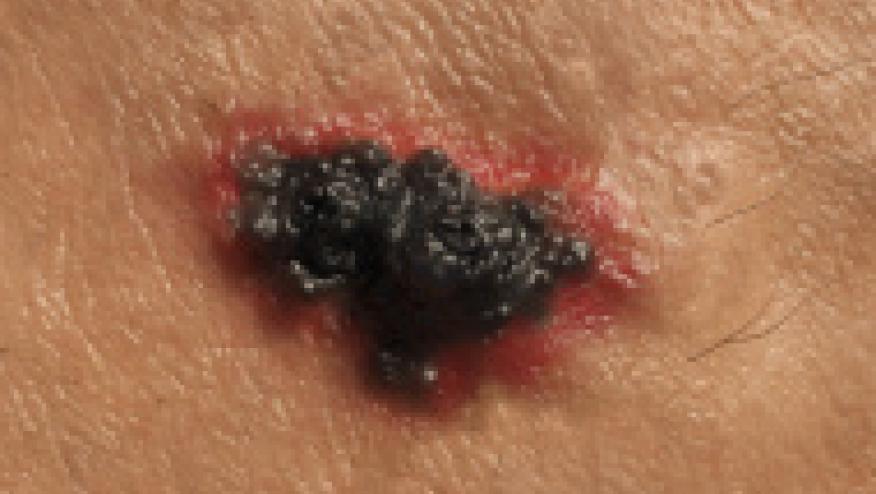
There is a large body of data that shows tumor necrosis factor inhibitors (TNFi) use in rheumatoid arthritis (RA) confers the same risk as that seen in RA - meaning there is no increase over and above that incurred by inflammation and RA itself. There are fewer studies about whether it is safe to use a TNFi in someone with a pre-existing history of cancer.
Raaschou and colleagues have performed a cohort comparison of RA patients, in a prospective Swedish database, who were diagnosed with cancer between 2001 and 2015 and were either treated with a TNFi or were never given a biologic agent. The primary outcome was the first recurrence of cancer.
Among the 467 RA patients who started TNFi treatment (a mean of 7.9 years after a cancer diagnosis), the recurrence of cancer was seen in 42 TNFi treated patients (9.0%).
Among 2164 matched patients with the same cancer history but were biologic naive, 155 had a cancer recurrence (7.2%).
Thus, while there were a few more numerically, these results were not significantly different (HR, 1.06 [95% CI, 0.73 to 1.54).
The authors speculate that channeling bias was possible if patients with a better index cancer prognosis were more likely to receive TNFi, but there is no data to corroborate this.
The authors conclude that while TNFi treatment is not associated with increased risk for cancer recurrence in RA, they speculate that meaningful risk increases could not be ruled out completely.
These data are similar to that these authors have previously published showing no increased risk of dying from cancer if TNFi was given to someone with a history of cancer. What is encouraging about this data is that this is one of the largest cohorts examined for cancer recurrence and no risk was proven. Moreover, these patients with a long past history of cancer went on to safely receive a TNFi without added cancer risk.
Rheumatologists should treat the arthritis as aggressively as is necessary and leave cancer management, monitoring and screening to the oncologists.









If you are a health practitioner, you may Login/Register to comment.
Due to the nature of these comment forums, only health practitioners are allowed to comment at this time.