IL-17
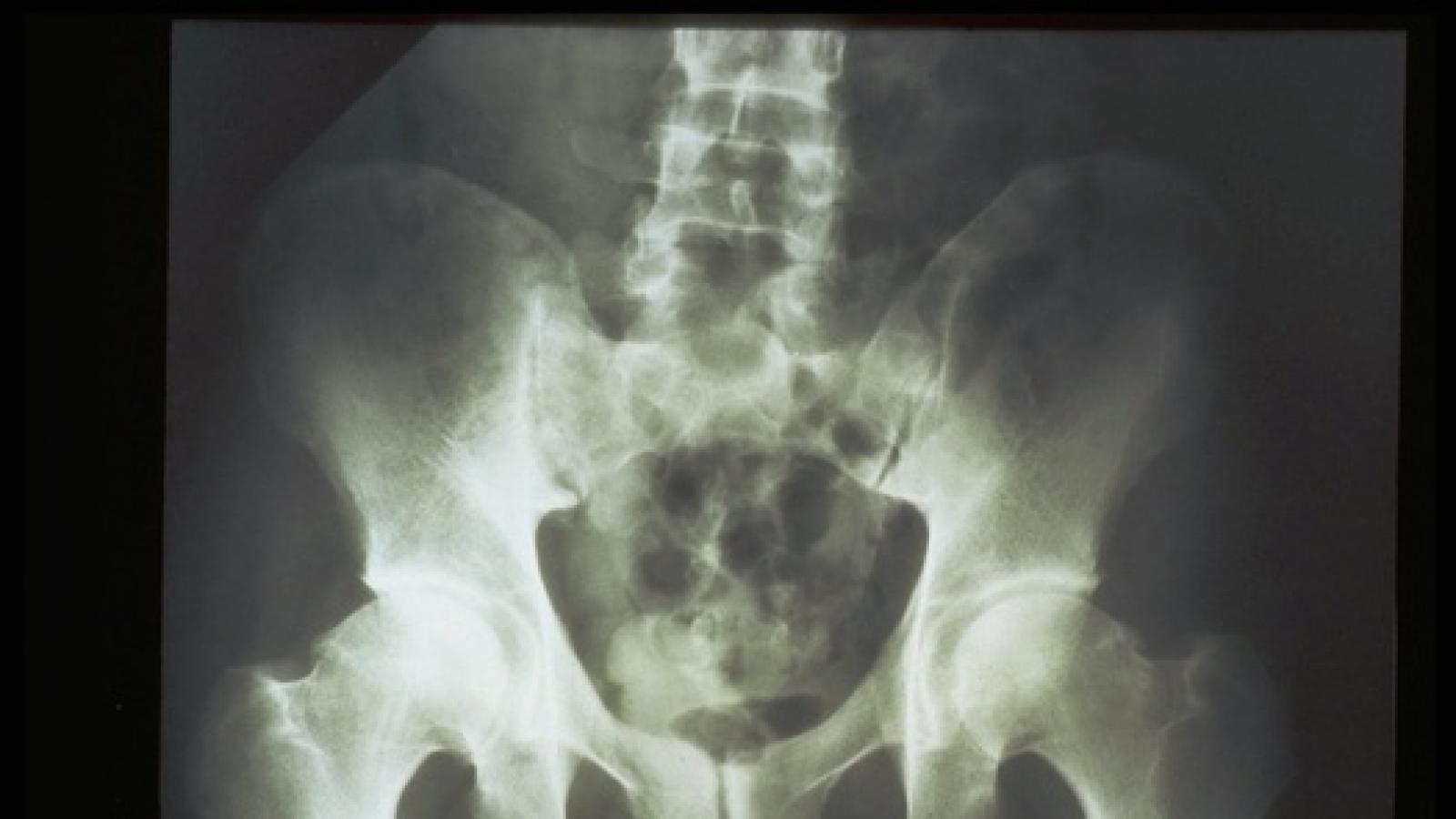
Most patients with early, active axial spondyloarthritis (axSpA) who quickly received a tumor necrosis factor (TNF) inhibitor experienced remission, and it didn't matter whether or not they had intestinal inflammation at baseline, a small single-arm study found.
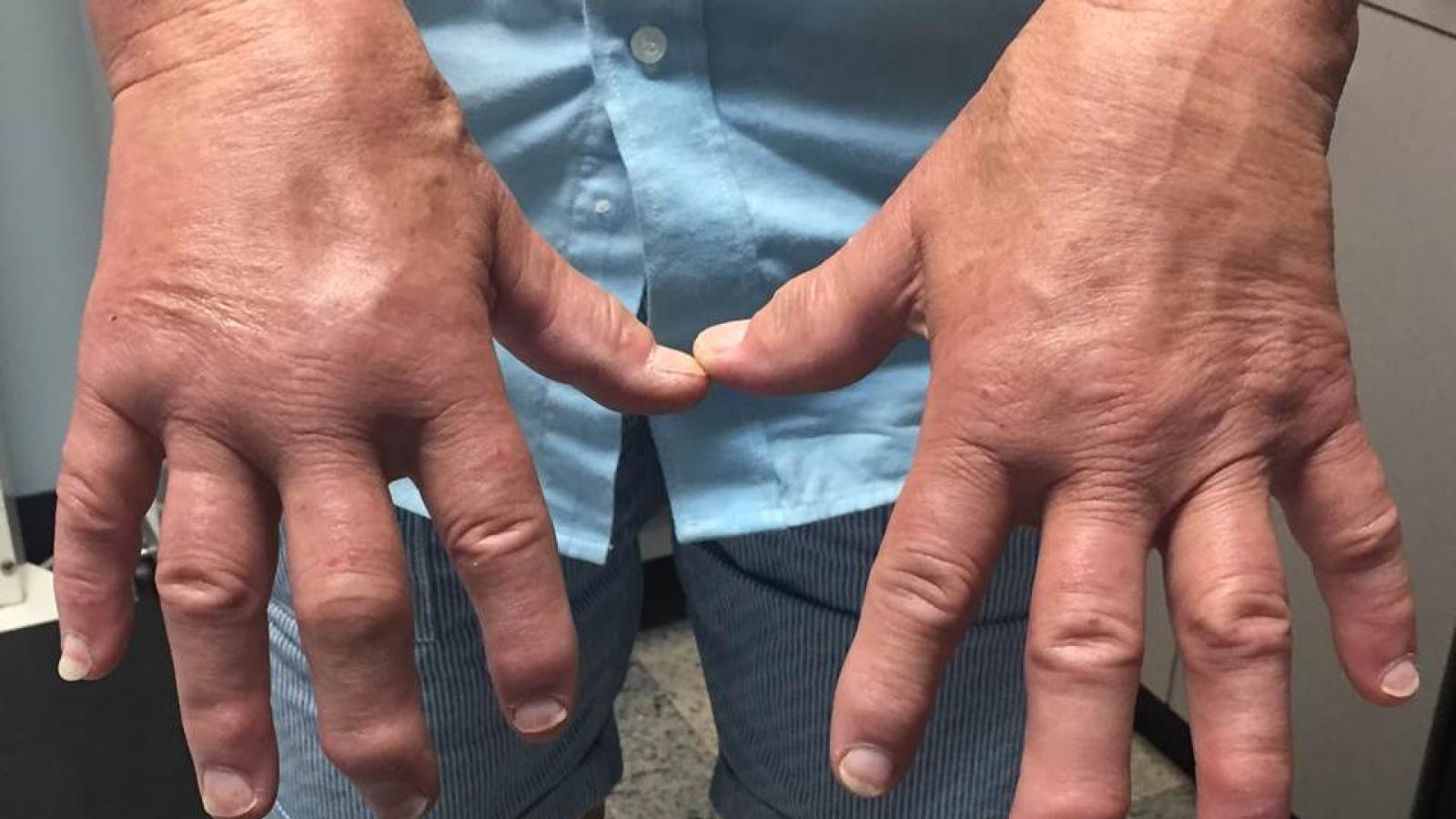
At EULAR 2025, Dr. Laura Coates (Oxford) took the plenary stage to reframe how we think about treating psoriatic arthritis. The message was clear: in 2025, PsA treatment is no longer about following a linear algorithm; it’s about understanding the unique constellation of domains, comorbidities, and patient factors that shape each clinical decision.
IL-17 inhibitors are an effective therapeutic for a broad spectrum of inflammatory and autoimmune diseases and its blockade has revolutionized management of diseases such as psoriasis, psoriatic arthritis and SpA. Is there a need for more medications within the same therapeutic class?
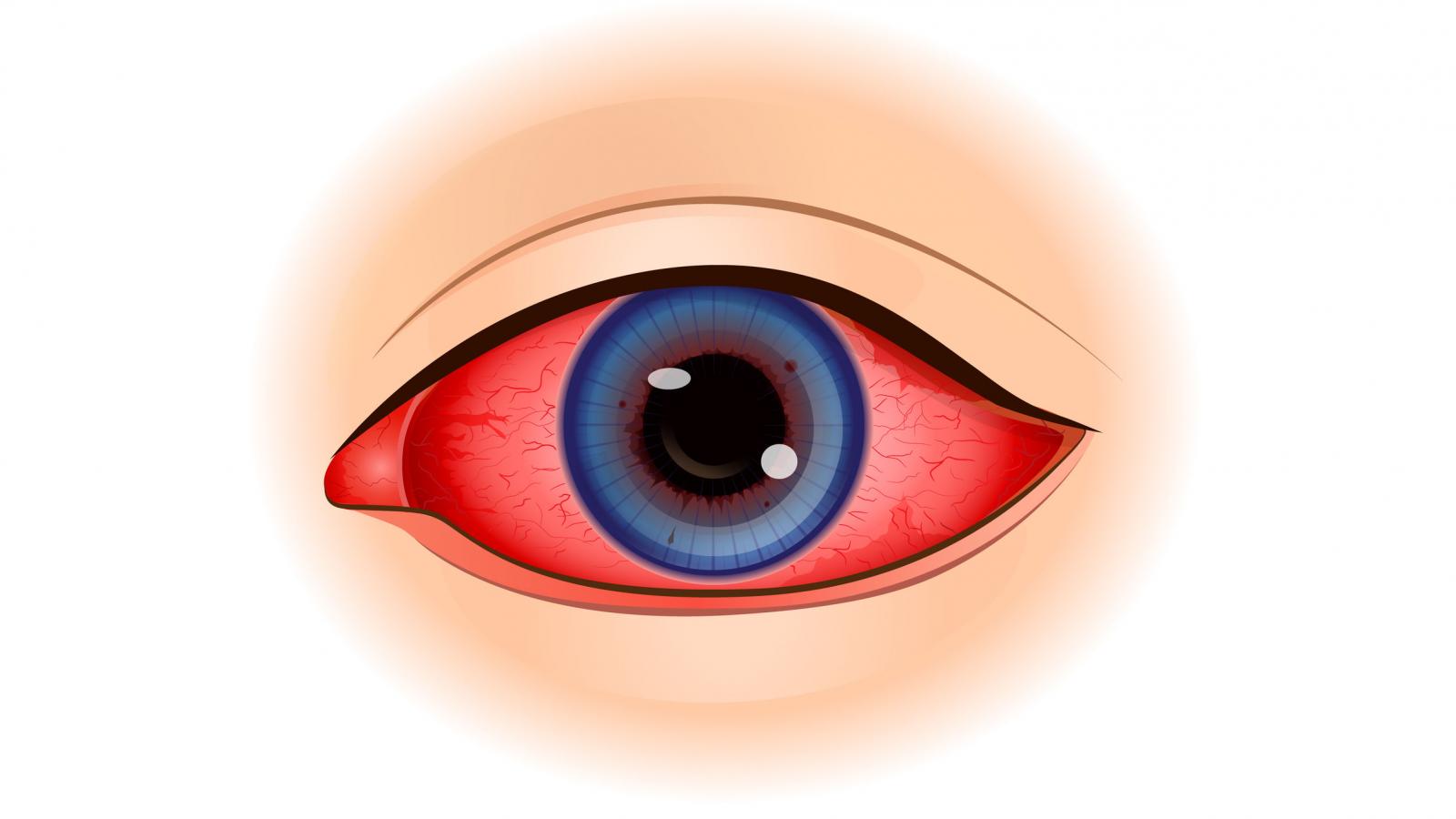
The longest studied drug for uveitis in SpA has been monocolonal TNFi Abs. Reductions of acute anterior uveitis have been found with etanercept but less impressively than adalimumab, infliximab, and in my opinion less than golimumab and certolizumab pegol.
Other data have emerged for JAKi and IL17i, with respect to acute anterior uveitis.
Despite the advances in the treatment of PsA with biologic (bDMARD) and targeted synthetic (tsDMARD), less than half of patients with this condition achieved remission or low disease activity. Combination DMARD treatment is often used in order to achieve remission or minimal disease activity. The standard practice is to use a conventional synthetic (csDMARD) with a bDMARD. The use of the combination of bDMARD with a tsDMARD such as a JAKi or
Choice is not just good, it is often necessary, and secukinumab promises just that in both PMR and GCA.