All News
Telemedicine Studies: A Trainee’s Perspective
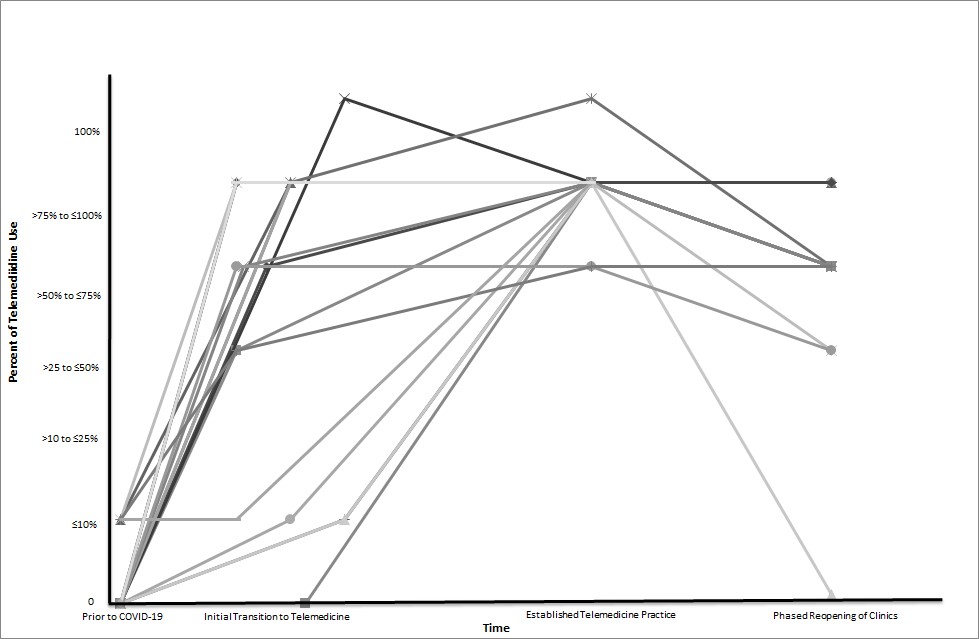
The shift from face-to-face consultations to telemedicine has been immense for clinicians and patients. Given the numerous challenges and nuances in practising telemedicine, it is apt that ACR 2020 has been packed with abstracts and presentations on this topic.
Read ArticleACR Best Abstracts - Day 1
The RheumNow faculty reporters have been glued to their monitors all day, viewing video, reading and listening to abstract presentations and I charged them to earmark those presentations were the “Best” they saw today. Below is the list of most often noted #ACRbest abstracts from Day 1.
Read ArticleIndustry Abstract Previews - ACR2020
Each pharmaceutical company has spent months and years preparing to present and highlight their featured clinical trials and abstracts at ACR 2020. This is our selection of their best studies for you to review and evaluate as part of your to-do list.
Read Article

Robert B Chao, MD doctorRBC ( View Tweet)

Mrinalini Dey DrMiniDey ( View Tweet)

Dr. Rachel Tate uptoTate ( View Tweet)

Meral K. El Ramahi, MD MeralElRamahiMD ( View Tweet)

Dr. Antoni Chan synovialjoints ( View Tweet)

Dr. Antoni Chan synovialjoints ( View Tweet)





sheila RHEUMarampa ( View Tweet)

Dr. Rachel Tate uptoTate ( View Tweet)


k dao KDAO2011 ( View Tweet)






