All News
Hydroxychloroquine Fails as Pre-exposure Prophylaxis for COVID-19
Numerous previous studies have questioned the efficacy or protection afforded by hydroxychloroquine (HCQ) for COVID-19 and studies have show that HCQ has failed when given as post-exposure prophylaxis to health care workers (HCWs). A new randomized controlled trial has shown that HCQ failed when given as 8 weeks of pre-exposure prophylaxis in hospital-based HCWs exposed to patients with COVID-19 patients.
Read ArticleRheumNow Podcast – Cardiovascular Risk in Psoriatic Disease (9.25.20)
Dr. Jack Cush reviews the news and Journal articles from the past week on RheumNow.com.
Read ArticleYoung Adults are Driving Up COVID-19 Rates
CDC reports that since June 2020 individuals infected with COVID-19 have largely been young adults in the 20-29 year age bracket. Moreover, younger adults appeared to be driving community transmission of COVID-19.
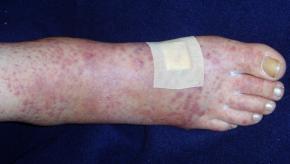
Read ArticleLivedo, Purpura and Coagulopathy in Severe COVID-19
JAMA Dermatology expands the spectrum of complications seen with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection describing cutaneous purpura and livedo lesions in patients with severe COVID-19.
Read ArticleCDC Reverses Guidance for Asymptomatic COVID Contacts
Asymptomatic people who have been exposed to COVID-19 should be tested, the CDC said on Friday, in a reversal of controversial guidance the agency introduced in late August.
Read ArticleRheumNow Podcast – Lupus Delights (9.18.20)
Dr Jack Cush reviews the news and journal reports from the past week on RheumNow.com:
Read ArticleCOVID-19 Risks in Pregnant Women
There has been little science or evidence regarding the effects of COVID-19 infection on pregnancy and vice versa; and now the recent MMWR addresses the subject with two new reports
Read ArticleRheumNow Podcast – To Celiac Test or Not? (9.4.20)
Dr Jack Cush reviews the news, journal articles and takes a few Back Talk questions this week:
Read ArticleCOVID and the Multisystem Inflammatory Syndrome in Children
Lancet Infectious Disease has reviewed the epidemiology, causes, clinical features, and current treatment for the multisystem inflammatory syndrome in children (MIS-C) and adolescents associated with COVID-19, noting severe organ damage can occur pediatric COVID-19 patients who are severely ill.&
Read ArticleCDC: COVID Seroprevalence in Health Care Workers
CDC reports that gmong 3,248 healthcare personnel (HCP) observed, 6% had antibody evidence of previous SARS-CoV-2 infection; 29% of personnel with SARS-CoV-2 antibodies were asymptomatic in the preceding months, and 69% had not previously received a diagnosis of SARS-CoV-2 infection.
Read ArticleHepatitis C Anti-Viral Drug-Induced Arthritis
Curative direct-acting antiviral therapy (DAAT) for hepatitis-C virus (HCV) infection has been revolutionary, but a novel report shows that nearly one quarter of DAAT treated patients developed new onset or significant worsening of MSK symptoms, despite being negative for hepa
Read ArticleRheumNow Podcast – The Bad News That’s Fit to Print (8.21.20)
Dr Jack Cush reviews the news and journal reports from the past week on RheumNow: filgotinib rejection, delays in diagnosis, metformin benefits COVID, Abx and IBD, and UPA beats MTX.
Read ArticleIncreased Lupus Anticoagulant Activity in COVID-19 Infection
JAMA Network Open reports that after adjusting for inflammation, lupus anticoagulant (LA) is significantly increased (positive) in COVID-19 patients and that LA positivity was associated with incidence risk of thrombotic events.
Read ArticleRheumNow Podcast - The SARS-CoV-2 Update (8-14-20)
Dr. Jack Cush updates the news and journal articles from the past week on RheumNow.com, with information on enthesitis, nr-Ax-SpA, UAB, Blockbuster Rheum Drugs and use of ACE inhibitors.
Read ArticleRheumatic Diseases, Drugs and COVID-19 Guidelines
Several recent publications have focused on the risk and outcomes of rheumatic disease (RDD) and autoimmune patients who become infected with SARs-CoV-2.
Read ArticleLatest COVID-19 Numbers from CDC
Following are the latest CDC numbers for COVID-19 in the U.S., including total cases and deaths; the states with the highest number of COVID-19 deaths; and COVID-19 healthcare case numbers.
Read ArticleInfliximab Use Near Surgery is Safe
Risk factors for perioperative infections include age, comorbidity, rheumatoid arthritis and steroids to name a few; whether concurrent use of TNF inhibitor (TNFI) therapy adds to this risk has been debated. In a study of elderly patients receiving infliximab infusions, infliximab use prior to surgery did not change the risk of post-operative infections.
Read ArticleDMARD Use Does Not Increase COVID Hospitalization
An observational study of patients with systemic autoimmune inflammatory rheumatic diseases (AIRD) who also had COVID-19 disease shows that AIRD increased the risk of hospitalization, but that the use of disease-modifying antirheumatic drugs (DMARDs) were not associated with hospitalization.
Read Article
Links:
Dr. John Cush RheumNow ( View Tweet)

Links:
Dr. John Cush RheumNow ( View Tweet)