All News
Is exercise the missing medicine in lupus?
For lupus, sedentary lifestyle may be a driving force of disease activity. Today, the final day of ACR, Sarah Patterson, MD from UCSF will present
Read ArticleACR Best Abstracts - Day 2
Day two at ACR 2022 was full of great sessions on imaging, vasculitis, lupus, vasculitis, spondyloarthritis, COVID, pregnancy, microbiome, economics and more.
Here are the RheumNow faculty selections for #ACRbest abstracts today:

What’s new w #classification for #APS? You don’t have to have 2 positive tests disseminated in time. BUT remember the the labs for anticardiolipin are shockingly variable btwn centres. @RheumNow #ACR22 https://t.co/NTqQ6h7fws
Janet Pope Janetbirdope ( View Tweet)
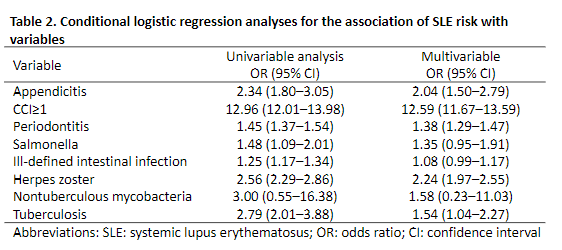
Chen et al. Appendicitis associated increased risk incident SLE in population-based case-control study from Taiwan. HR 2.04 @RheumNow #ACR22 Abstr#1750 https://t.co/L9dTpMdHNP https://t.co/mEHeL6JnuE
Richard Conway RichardPAConway ( View Tweet)
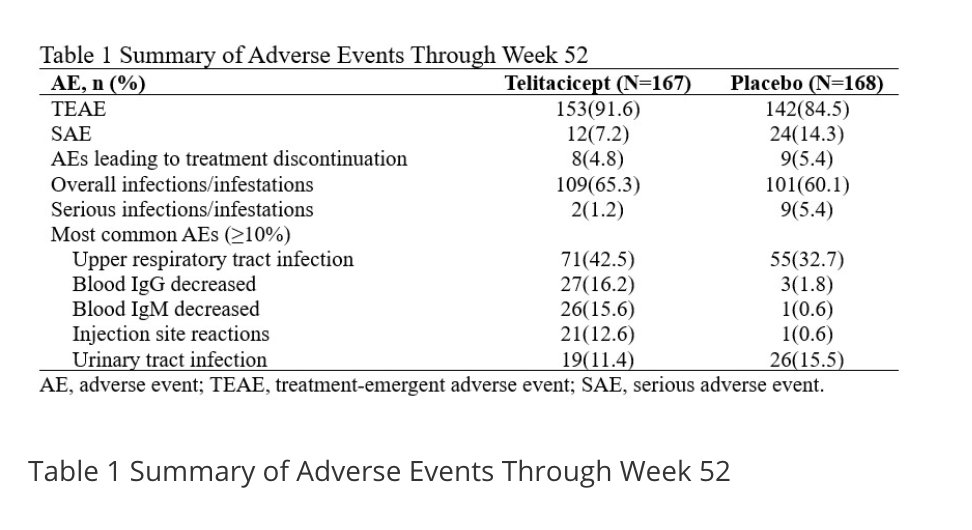
#ACR2022 L07: Telitacicept - anti-BlyS and APRIL in SLE
335 pts P3 52 wk study TEL 160 mg SQ q7d vs PBO
83% SRI4 response in TEL vs 38% PBO (p<0.001)
As early as w4, sustained to w52
Most common AEs: URIs, decr IgG/IgM, injxn site rxn, UTI
@RheumNow #ACRBest https://t.co/UpEwEaonDO
Eric Dein ericdeinmd ( View Tweet)

A Novel Treatment Response Measurement Tool for Lupus
Dr. Dao discusses abstract 2054 with Dr. Morand at the #ACR22 Convergence. Abstract 2054: Towards a Novel Clinician-Reported Outcome Measure for SLE – Outcomes of an International Consensus Process.
https://t.co/iqqyI953Vz https://t.co/taUjTHsrJ2
Links:
Dr. John Cush RheumNow ( View Tweet)
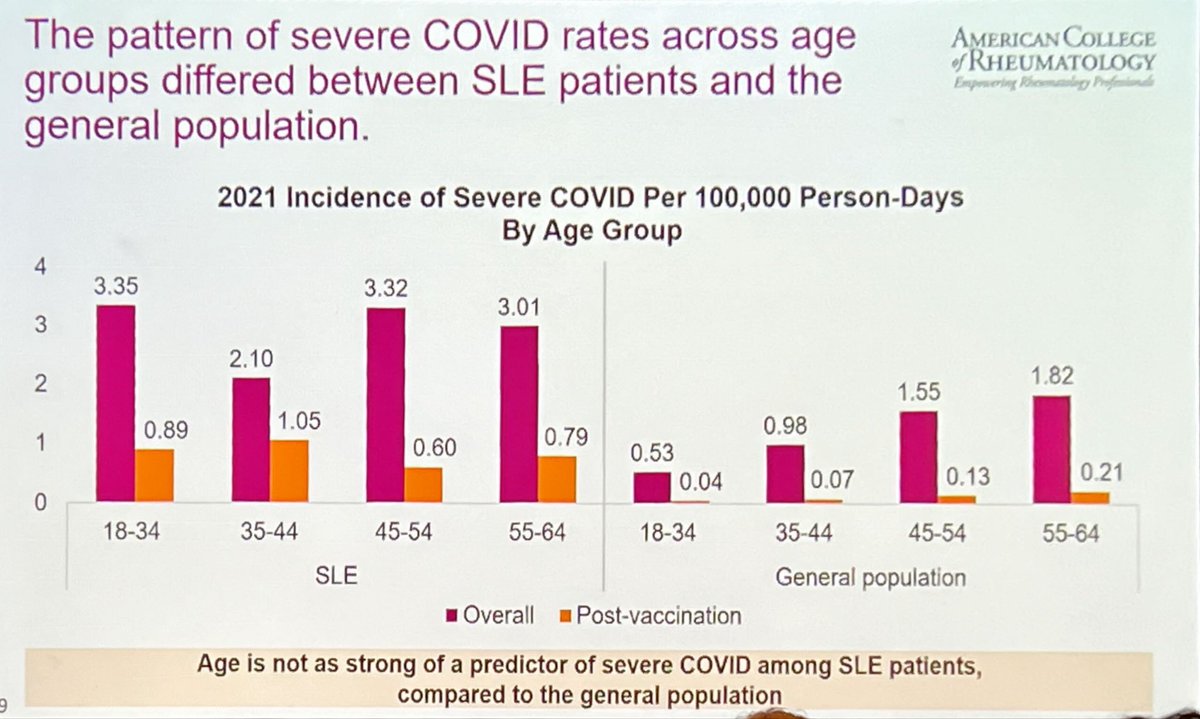
Even young SLE patients are still at high risk of severe COVID:
- in general pop, age is key factor
- in SLE, risk is high across age groups (maybe due to both meds & disease)
- vaccination makes a big diff but SLE pts still at high risk
ABST1591 @CCalabreseDO #ACR22 @RheumNow https://t.co/ra1F79ITn3
David Liew drdavidliew ( View Tweet)
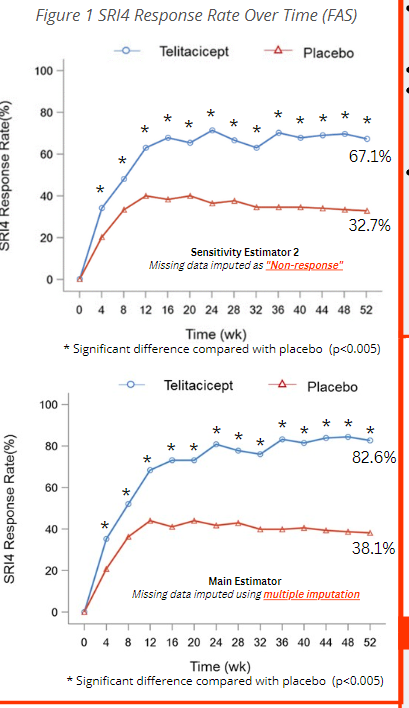
Wu et al Phase 3 RCT of Telitacicept (targets BlyS and APRIL) in SLE. Primary endpoint met at week 52! SRI(4) 67% vs 33% or 83% vs 38% (P<0.001 for both) depending on how you want to slice it. @RheumNow #ACR22 Abstr#L07 https://t.co/nnKr4AU8Jk https://t.co/9BVF6OljFQ
Richard Conway RichardPAConway ( View Tweet)
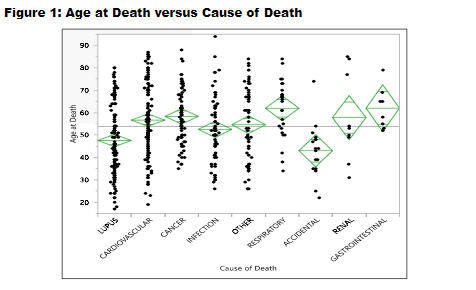
#ACR22 Abstr#2068 Data from John Hopkins showed leading cause of deaths (1985-2019) in #lupus were #SLE & Cardiovascular (both 23%), then cancer & infection.SLE deaths common in younger. African-American died younger vs White. Need to improve with therapies we now have @RheumNow https://t.co/4tDhr1Eodm
Md Yuzaiful Md Yusof Yuz6Yusof ( View Tweet)
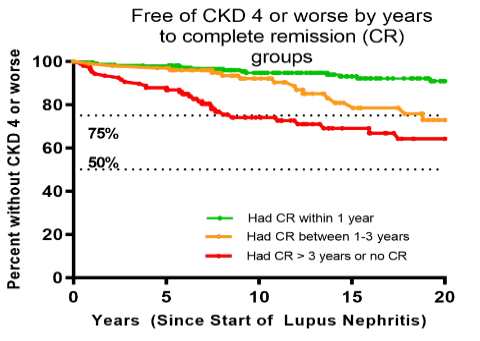
#ACR22 Abstr#2061 It's time to tight control newly diagnosed #lupus nephritis patients. In a cohort study which 16% developed advanced CKD, risk was reduced if remission achieved by 12 mths of diagnosis. =>1 flare & shorter time-on-therapy increased risk
@RheumNow #ACRBest https://t.co/swYn2g4hqe
Md Yuzaiful Md Yusof Yuz6Yusof ( View Tweet)
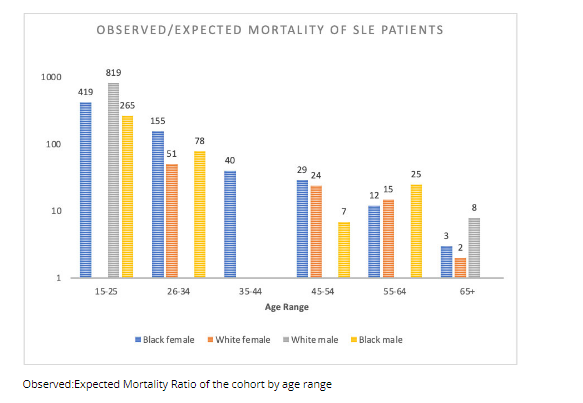
#SLE mortality in South Carolina Lupus Cohort
Standardized mortality ratio (SMR) is higher in blacks
Higher SLICC scores in blacks
abst#2106 #ACR22 @rheumnow https://t.co/NAdNhUHsbc
Bella Mehta bella_mehta ( View Tweet)
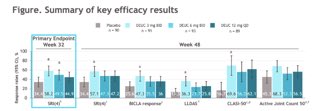
New SLE Rx. Deucravitinib a TYK2i phase 2 RCT showed SRI4 endpoint. Subset of 3 mg bid was best vs 6 mg bid and 12 mg OD. Skin via CLASI-50 & other endpoints also positive. Awaiting phase III. Abst1117 #ACR22 @RheumNow https://t.co/fZI3AV5pML
Janet Pope Janetbirdope ( View Tweet)
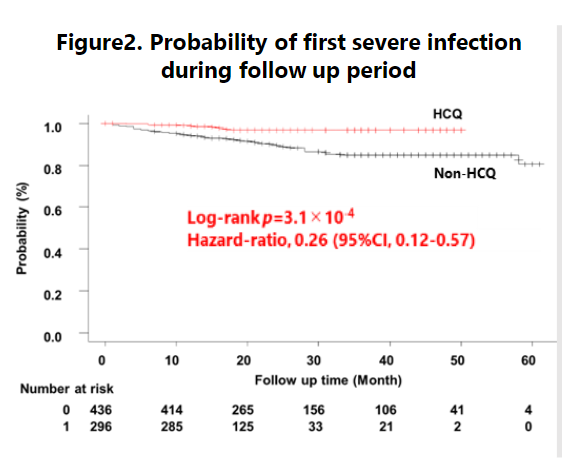
Hidekawa et al. HCQ use assoc reduced severe infection in LUNA SLE registry, HR 0.26. ?due to better disease control rather than anti-infectious role, but HR 0.32 in multivariable model including SLEDAI. @RheumNow #ACR22 Abstr#2059 https://t.co/EgTJOAymoF https://t.co/gmchk9ZS5L
Richard Conway RichardPAConway ( View Tweet)
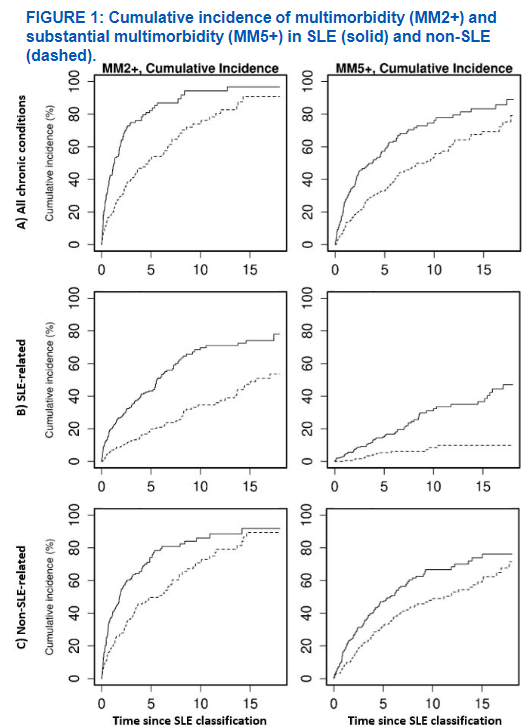
Figueroa Parra @AliDuarteMD et al. Multimorbidity in SLE. Higher at classification - due to non-SLE assoc. SLE-assoc drive increased accumulation over time but non-SLE assoc also increased @RheumNow #ACR22 Abstr#2091 https://t.co/6IyhovSNYA https://t.co/qmYfoqCTtz
Richard Conway RichardPAConway ( View Tweet)
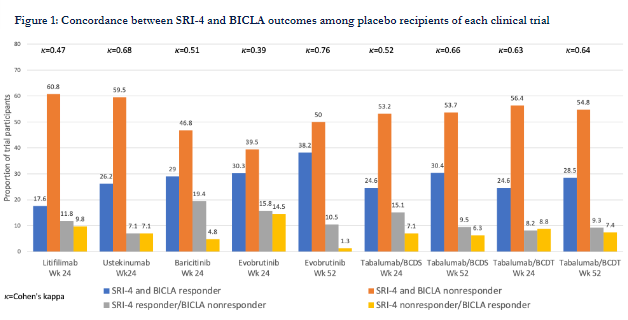
#ACR22 Abstr#2055 SRI-4 and BICLA: how do they converge and diverge? Analyses of 6 x Non-Renal #Lupus RCT showed discordance (12-30%).When discordant, SRI-4 classified more pts as responders vs BICLA. Concordance higher at 52 vs 24 wks. Vital to interpret both outcomes @RheumNow https://t.co/prSfTrv0E8
Md Yuzaiful Md Yusof Yuz6Yusof ( View Tweet)
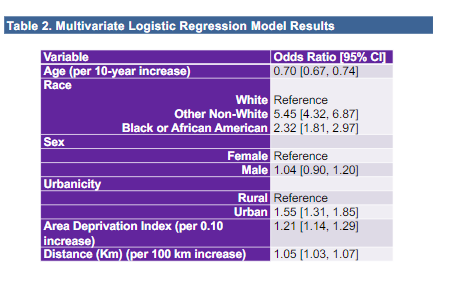
#ACR22 Abstr#1764 In addition to race, what social health aspect to consider when assessing #lupus epidemiology? A study identified urbanicity and area deprivation index were associated with SLE diagnosis. Could those living in the city = better access and diagnosis? @RheumNow https://t.co/PsNt8vQufs
Md Yuzaiful Md Yusof Yuz6Yusof ( View Tweet)

Urine Proteomics in SLE with Dr. Michelle Petri
Dr. Michelle Petri discusses abstract 0536, Change in Urinary Biomarkers at Three Months Predicts 1-year Treatment Response of Lupus Nephritis Better Than Proteinuria, being presented Saturday at #ACR22.
https://t.co/rBDnbSqQCI https://t.co/WfERf1k5VB
Links:
Dr. John Cush RheumNow ( View Tweet)
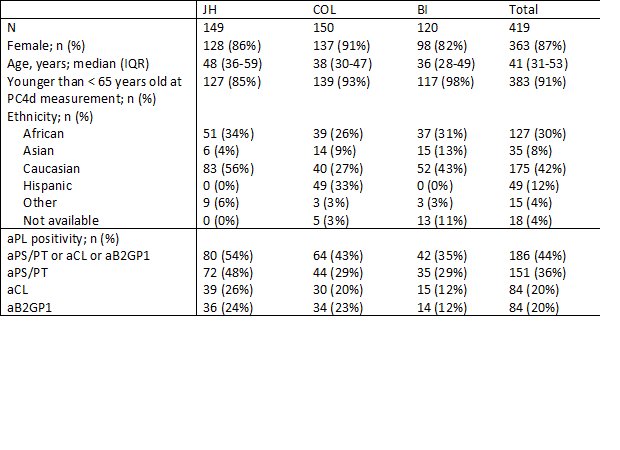
PC4d≥10 MFI is associated with thrombosis in SLE and predicts future arterial thrombosis. Abs 1442 #ACR22 @RheumNow https://t.co/zg7rrOSALs https://t.co/Hs2eOa2vxJ
Dr. Rachel Tate uptoTate ( View Tweet)
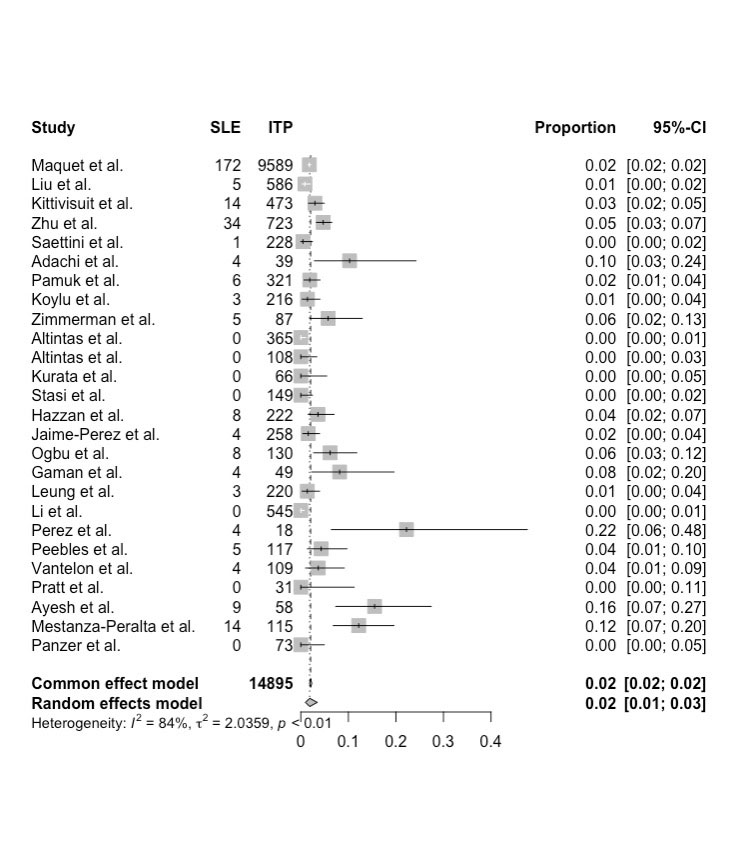
Numerically, SLE was more common in cITP patients. Risks include +ANA and female sex. Abs 1461 #ACR22 @RheumNow https://t.co/0kyqlVphac https://t.co/HfYKCMybdL
Dr. Rachel Tate uptoTate ( View Tweet)
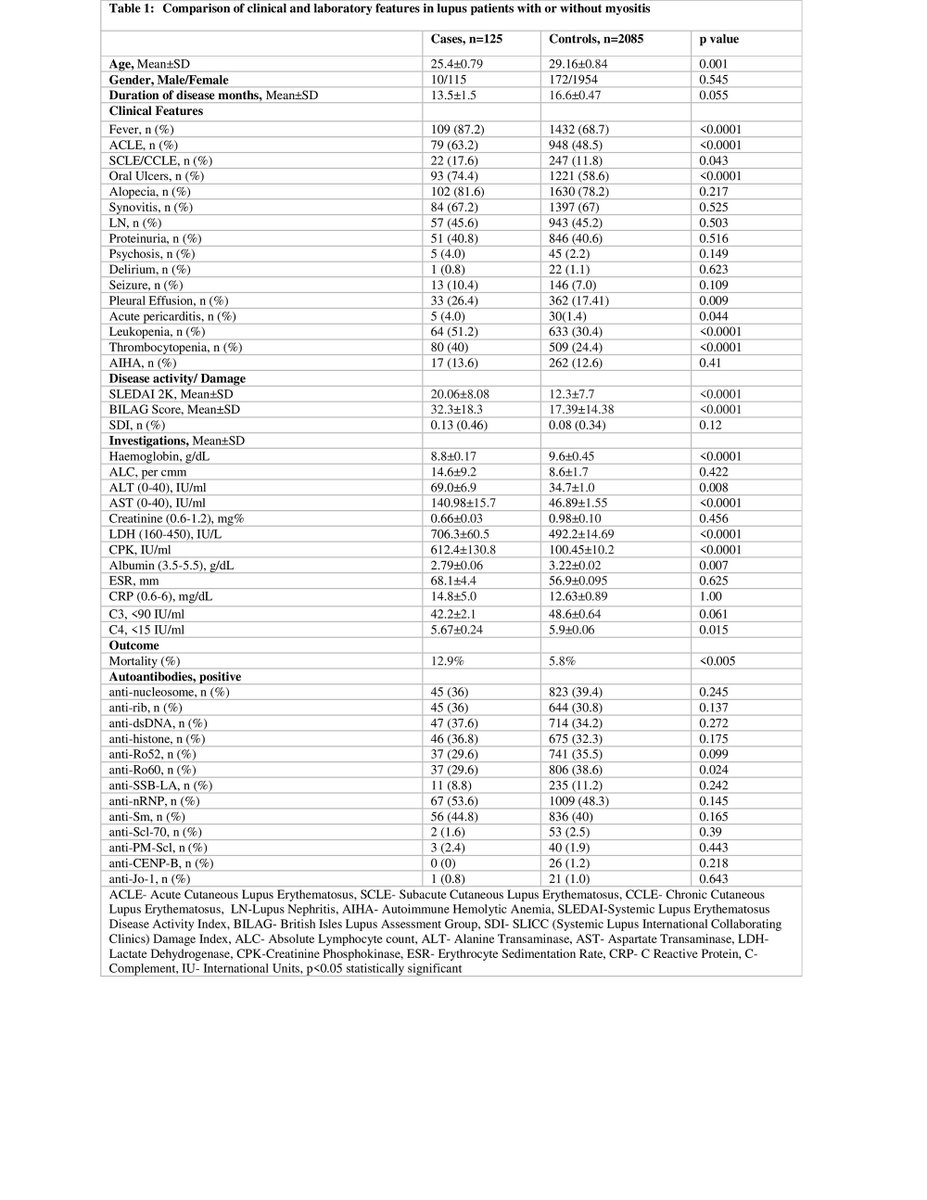
While myositis in the setting of SLE was found to be around 5% in Abs 1453, it was not associated with mortality. #ACR22 @RheumNow https://t.co/hLLuYoXsCv https://t.co/44XGhbPxzW
Dr. Rachel Tate uptoTate ( View Tweet)





