All News
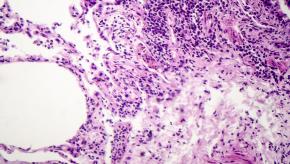
Mortality Risk in Rheumatoid Lung Patients
A Medicare claims analysis of rheumatoid arthritis (RA) patients showed that RA-associated interstitial lung disease (RA-ILD) was seen in nearly 5% of patients and was found to increase mortality risks, including respiratory and cancer mortality not explained by other factors.
Read ArticleFactors Predictive of SLE Flare After HCQ Taper/Discontinuation
The benefits of hydroxychloroquine in lupus are many, but if you were to withdraw HCQ? A recent study of five Canadian cohorts, suggests that certain baseline variables, including age, race, and steroid use, were predictive of flare in patients with SLE who tapered or discontinued treatment with hydroxychloroquine.
Read ArticleInequities in Telemedicine During COVID-19
Health equity in the telehealth age has assumed added importance since the COVID-19 pandemic began. The Federal Communications Commission estimates that about 21 million Americans don't have access to the Internet in their homes. Other sources estimate it is closer to 162 million.
Read Article2020 Rheumatology Year in Review
2020 was historic, memorable and game-changing. Under the cloud of COVID-19, there were many significant and memorable advances and setbacks for the rheumatology world. In our accounting of most read articles for 2020, (not surprisingly) 17/20 were COVID-related.
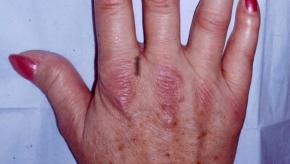
Read ArticleProDERM Study: IVIG in Dermatomyositis
The ProDERM study design and outcomes are previewed in Medicine; and as promised the results were revealed at ACR Convergence in November 2020 showing that IVIg is safe, effective and superior to placebo i(PBO) in patients with dermatomyositis (DM).
Read ArticleLong Term Safety and Efficacy of Tacrolimus in Lupus Nephritis
Takeuchi et al has published their large experience with long-term tacrolimus use in lupus nephritis patients showing its real-world safety and efficacy.
Read ArticleAdipose Transplants as a New Regulator of Osteoarthritis
A novel report from PNAS suggests that in osteoarthritis (OA), the damage is not entirely from body weight and mechanics, instead it may be from adipose tissue itself.
Read ArticleCorticosteroid Use Hikes CV Risks in Rheumatic Patients
UK Clinical Practice Research Datalink population study shows that patients with immune-mediated inflammatory diseases, such as RA, PMR, GCA and IBD, have an augmented risk of CV outcomes with glucocorticoid use; even lower doses had a near doubling of their underlying CVD risk.
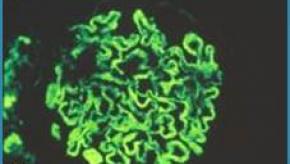
Read ArticleAdherence to Hydroxychloroquine Lowers Lupus Mortality
A lupus cohort study from British Columbia, Canada has shown that medication adherence with hydroxychloroquine (HCQ) is associated with a 71% to 83% lower mortality.
Read ArticleRhapsody Study: IL-1 Inhibition in Recurrent Pericarditis
Recurrent pericarditis is a rare, probable autoinflammatory disorder mediated by interleukin-1 (IL-1); and is often refractory to glucocorticoids and colchicine.
Read ArticleEULAR Guidance on Patient Adherence to Meds
Non-adherence may be the single most untold risk to suboptimal outcomes in the care of musculoskeletal disease. It has been estimated that 30-80% of patients with rheumatic and musculoskeletal diseases (RMDs) are nonadherent to prescribed regimens. EULAR has commissioned a task force
Read ArticleSpinal Benefits Seen With Cosentyx in PsA
Secukinumab (Cosentyx) was effective for axial manifestations of psoriatic arthritis in a 52-week multicenter phase III study, investigators reported.
Read ArticleTelemedicine Less Utilized in the South and Urban Areas
MMWR has reported on a July 2020 survey study from 1,009 Health Resources and Services Administration–funded health centers showing that urban Health centers were more likely to provide virtual visits than those in rural areas.
Read ArticlePlaquenil Does Not Protect Lupus Patients from COVID-19 (Best of 2020)
Annals of Rheumatic Disease reports on an analysis of lupus (SLE) patients that shows COVID-19 infection rates were similar between those lupus patients who were taking hydroxychloroquine (HCQ) and those not taking HCQ.
Read ArticleUpdate on Polymyalgia Rheumatica and Giant Cell Arteritis (Best of 2020)
JAMA has published a clinical update of recent studies on GCA. While PET/CT scanning are novel means of demonstrating activity, they have not changed the diagnostic approach to GCA or PMR and although there are no new proven treatment strategies for PMR beyond glucocorticoids, the FDA has approved tocilizumab as a first-line glucocorticoid-sparing agent.
Read ArticleACR 2020 Reproductive Guidelines - Medication Use with Pregnancy (Best of 2020)
The ACR has published guidelines to manage reproductive health issues in rheumatic disease (RMD) patients before, during and after pregnancy. In this second excerpt from their guidelines articles, we present recommendations (and good clinical practice statements) for paternal rheumatology medication use by men with RMD and on conventional rheumatology medications and biologic use in pregnancy for women with RMD.
Read ArticleACR 2020 Reproductive Guidelines - Lactation Guidance (Best of 2020)
In this third excerpt from the ACR guidelines on managing reproductive health issues in rheumatic disease patients, we present recommendations regarding the use of glucocorticoids and guidance on lactation and medication use post-partum.
Read ArticleBest of 2020: New EULAR/ACR Classification Criteria for SLE
The European League Against Rheumatism (EULAR) and the American College of Rheumatology (ACR) have jointly developed new classification criteria for systemic lupus erythematosus (SLE); prompted by the need for criteria that were both highly sensitive and specific. The net result is improved sensitivity and specificity, but the use of positive ANA requirement along with a longer list of weighted criteria ensures its utility in SLE research (including early or latent SLE), but not clinical practice.
Read ArticleBest of 2020: The COVID-19 Global Rheumatology Registry
What started out as online tweets and sharing newsfeed and case reports, has progressed to the formation of the COVID-19 Global Rheumatology Alliance, whose mission is to create an international rheumatology registry of patients affected by the disease in order to better understand the disease and guide clinicians in assessing and treating patients.
Read ArticleBest of 2020: Rheumatic Disease Drugs and COVID-19
We are in the early stages of trying to limit the morbid and mortal consequences of the corona virus pandemic of 2020. Not surprisingly, the recommendations designed to limit exposure and damage continually highlight the fact that the elderly and immunosuppressed may be amongst the most severely affected should they become infected with this virus.
This has led to a great deal of uncertainty by patients and providers about how rheumatic diseases and their treatments need to be specifically addressed.