All News
Vitamin D and Lupus Outcomes (11.21.2025)
Dr. Jack Cush reviews the news and journal reports from this past week on RheumNow.com.
Read ArticlePulse Steroids and Mycophenolate in Juvenile Dermatomyositis
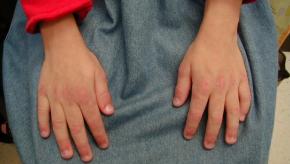
JAMA Dermatology has published a pilot study demonstrating the safety and efficacy of intermittent intravenous methylprednisolone pulse (IVMP) therapy plus mycophenolate in 28 patients with juvenile dermatomyositis (JDM).
Read ArticleTreating During Pregnancy (11.14.2025)
Dr. Jack Cush reviews the journal articles, news and guidelines from this past week on RheumNow.com
Read ArticleHospital Mortality in Dermatomyositis
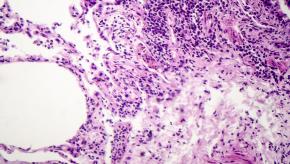
A cohort study shows that hospitalized patients with dermatomyositis have higher in-hospital mortality in the presence of active rash, interstitial lung disease, and elevated neutrophil to lymphocyte ratio at admission.
Read ArticleMore on Methotrexate and ILD Risk
To assess the progression of the interstitial lung disease related to Methotrexate (MTX) exposure, and to evaluate the lung involvement in RA non-ILD patients with MTX exposure, a systematic review was performed to assess whether RA patients receiving methotrexate (MTX) are at greater risk f
IL-1 Inhibition in CPPD
Controlled clinical trials in patients with calcium Pyrophosphate Deposition Disease (CPPD) are scant. Now a metanalysis provides evidence that anakinra, an interleukin-1 inhibitor, is a promising alternative for patients with acute CPPD flares.
Read Article

Dr. John Cush RheumNow ( View Tweet)

Dr. John Cush RheumNow ( View Tweet)







Dr. John Cush RheumNow ( View Tweet)