All News
What should head-to-head studies in inflammatory arthritis teach us?
The multimillion dollar question for inflammatory arthritis prescriptions is: which drug should I use next?
Read ArticleACR 2025 Rheumatology Round Up
Drs. Jack Cush & Arthur Kavanaugh, two of rheumatology’s most trusted voices, provide a breakdown of the latest breakthroughs and hottest topics in rheumatology from the 2025 ACR Convergence meeting in Chicago.
Read ArticleIL-23 Blockade Goes Oral
A new player is entering the IL-23 arena — and it’s a tablet! Icotrokinra (ICO), a first-in-class peptide that binds and blocks the interleukin-23 receptor (IL-23R), is showing encouraging efficacy and safety across a range of psoriasis (PSO) and psoriatic disease (PsD) studies.
Read Article
Psoriatic Arthritis: Which biologic agent is the best first choice?
A growing arsenal of therapeutic targets in psoriatic arthritis (PsA) has enhanced the landscape of treatment in patients with this disease.
https://t.co/pRMyPCvMrN https://t.co/nOgnf5F3Pw
Dr. John Cush RheumNow ( View Tweet)

Should we be using JAKi more in female SpA patients?
In recent years, data has emerged suggesting that female patients with spondyloarthritis, both psoriatic arthritis and axial spondyloarthritis, may have worse outcomes than male patients. A number of post-hoc analyses of https://t.co/smLao0q2hv
Dr. John Cush RheumNow ( View Tweet)

Early Peripheral SpA: Is it okay to stop treatment sometimes?
Dr. Richard Conway reports on abstract 0568 "Drug-Free Remission in Early Peripheral Spondyloarthritis: 10-year follow-up from the CRESPA-trial," presented at #ACR25
https://t.co/FtI2o90v9O https://t.co/jUAEDZhDW5
Dr. John Cush RheumNow ( View Tweet)

💬 #ACR2025 Topic Panels — LIVE!
Nov. 2 join RheumNow at 7 PM ET for a deep dives into the hottest topics in rheumatology:
👉 PsA
Join Us Live on:
X Live • Facebook Live • YouTube Live • LinkedIn Live • https://t.co/V10S4oVFsv
Top experts. Real clinical insight. Don't miss https://t.co/A4pUjZG3Dr
Links:
Dr. John Cush RheumNow ( View Tweet)

Psoriatic Arthritis Imaging
Dr. Arthur Kavanaugh talks about imaging in psoriatic arthritis at #ACR25
https://t.co/l6MKTgEJXu https://t.co/sKhoQWCPli
Dr. John Cush RheumNow ( View Tweet)

GLP-1 Receptor Agonists in PsA: Mortality and MACE https://t.co/GtTGHY7j5g
@synovialjoints discussed TriNetX data base looking at GLP-1 medications effect on MACE in PsA patients.
@RheumNow
#ACR25
Nouf Al hemmadi NoufAhmedAlham2 ( View Tweet)

What happens if you have #axSpA & concomitant #FM?
Pts with both have less TNFi retention,
-residual pain may lead to d/c Rx.
Need to determine if axSpA pt has #fibromyalgia as there may not be objective findings if no peripheral arthritis in axSpA.
#ACR25 @RheumNow abst#534
Janet Pope Janetbirdope ( View Tweet)

In a PsA cohort (n=1291), higher BMI was independently linked to lower odds of achieving MDA—especially in TNFi-treated patients. Impact was strongest in pain, skin, enthesitis, and PRO domains, not swollen joints. Each unit increase in BMI reduced MDA odds by 4–7%. Highlights https://t.co/TxO3HP51uk
Antoni Chan MD (Prof) synovialjoints ( View Tweet)

#2686 Using HR-pQCT, researchers tracked bone changes in RA & PsA. Seropositive RA showed worst bone density & microstructure, worsening with disease activity. TNFi, RTX & BARI improved MCP bone density, highlighting the impact of inflammation and treatment. @RheumNow #ACR25
Mrinalini Dey DrMiniDey ( View Tweet)

GLP-1 RA vs DPP4i & risk of rheumatic disease: propensity score matched cohort study using TriNetX
🔹 Lower incidence of OA, RA & gout w/ GLP-1 RA
🔹 No significant differences for PsA, SSc, axSpA, or SLE
@RheumNow #ACR25 https://t.co/BIVw3ajrFZ
Akhil Sood MD, MS AkhilSoodMD ( View Tweet)

#Deucravacitinib #Tyk2i in active #PsA to 52weeks
#PBO was crossed over at 16weeks
Ongoing improvement for high bar outcomes ex % in #minimal #disease #activity #MDA
#Xray #progression was reduced with real data (not imputed)
#ACR2025 @RheumNow @ACRheum https://t.co/kAMym2x8HQ
Links:
Janet Pope Janetbirdope ( View Tweet)
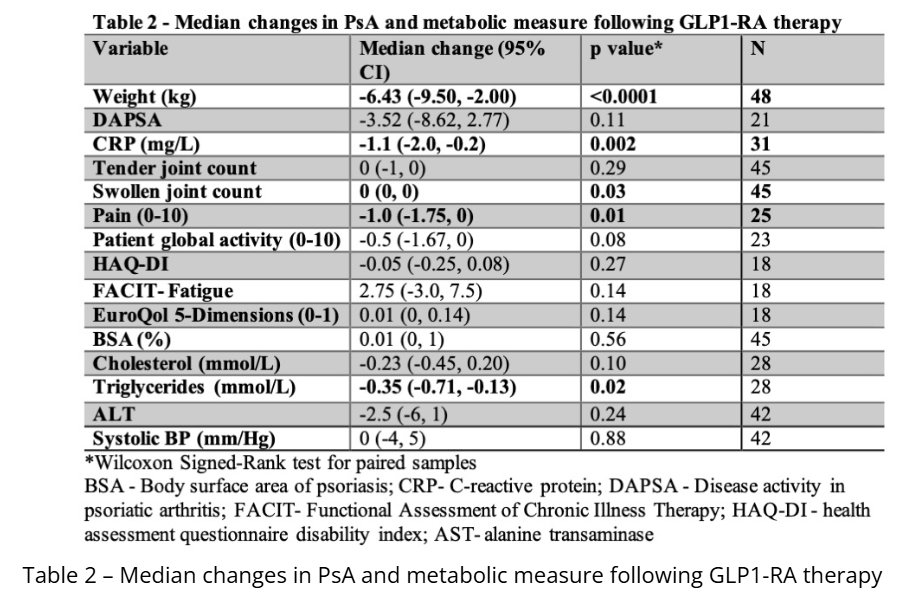
Abstract 2687: GLP-1 RA in PsA
In combined Toronto + NYU cohort, GLP-1 RA significantly associated with reduced:
- Weight, CRP, and pain scores
- Each 1% reduction in body weight associated w/ TJC, DAPSA, EQ-5D (QoL), LDL, Systolic BP
@RheumNow #ACR25 https://t.co/30lPDkALKs
Akhil Sood MD, MS AkhilSoodMD ( View Tweet)

Biologic choice in PsA: consider factoring in obesity ⚖️
Abstract 2691: In a longitudinal cohort study, obesity associated with ↓ odds of achieving minimal disease activity (MDA) among pts on TNFi, but not with other DMARDs
@RheumNow #ACR25 https://t.co/p4KaH6HKYj
Akhil Sood MD, MS AkhilSoodMD ( View Tweet)

Abstract 2690: Food as a Medicine
Mediterranean vs low-calorie DASH vs control diet in PsA (multicenter RCT):
🔹 All 3 groups showed significant weight loss & DAPSA by wk 24
🔹 Weight loss not diet type may be the driver of clinical improvement
@RheumNow #ACR25 https://t.co/rBS3HR1HXl
Akhil Sood MD, MS AkhilSoodMD ( View Tweet)

In a 5-year EHR-based cohort, PsO patients initiating IL-17i had significantly lower incidence of PsA/IA vs IL-23i, IL-12/23i, or TNFi. IL-17i reduced time with PsA/IA by 45% vs IL-23i, 61% vs IL-12/23i, and 74% vs TNFi. Further research need investigate if IL-17i may delay https://t.co/0PTbXZpLbu
Antoni Chan MD (Prof) synovialjoints ( View Tweet)
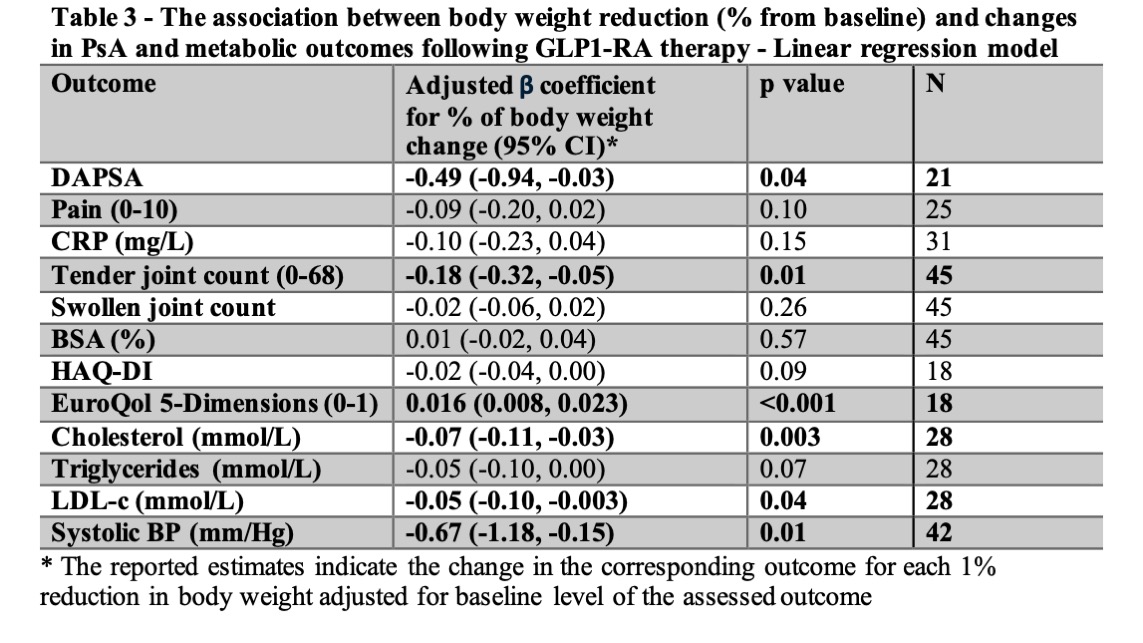
In PsA patients, GLP-1 RA therapy led to significant weight loss and improvements in CRP, pain, lipids, and blood pressure. PsA outcomes improved proportionally with weight loss. Regression analyses revealed that each 1% reduction in body weight was associated with significant https://t.co/Pph1PjfOve
Antoni Chan MD (Prof) synovialjoints ( View Tweet)

Deucravacitinib (TYK2) in PsA from POETYK trials
Improved ACR20 at wk16 (NNT ~5), less benefit for ACR70 (NNT ~20)
Steady improvements during open label extension (all pts received drug)
Would expect approval for PsA soon... where will this fit in your approach?
@RheumNow https://t.co/325h2hf0AE
Links:
Mike Putman EBRheum ( View Tweet)