All News
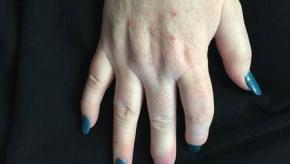
How early is early in psoriatic arthritis?
Guidelines (ACR/EULAR/GRAPPA) for the management of psoriatic arthritis (PsA) recommend the early referral of patients with the suspected condition for early assessment and treatment.
Read Article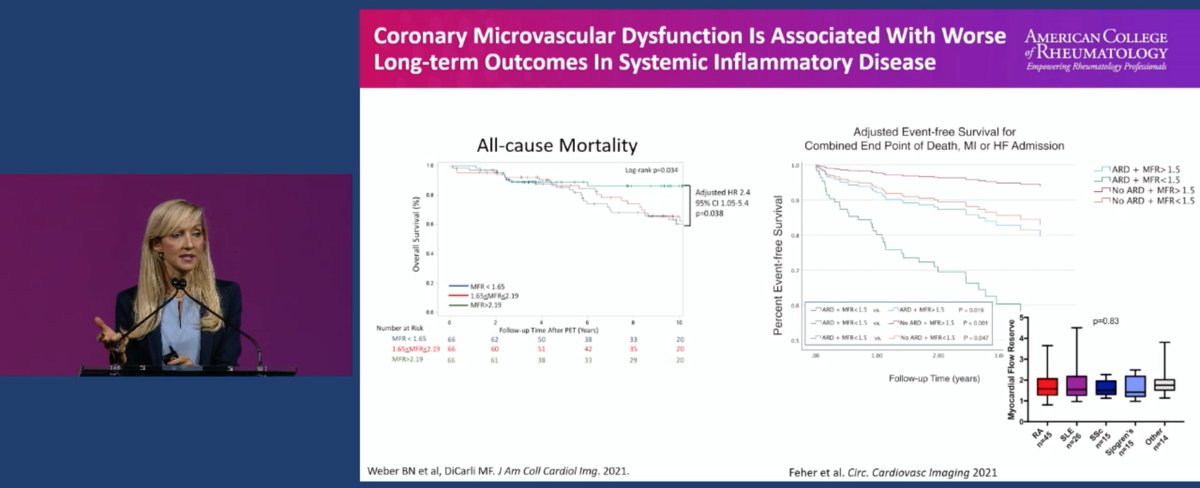
Always refreshing to hear from another specialist's point of view
Cardiologist @Bweber04 on CVD and rheumatologic diseases
Increased risk of death, MI and HF exacerbation in our pt population
Increased all cause mortality
@RheumNow #ACR23 https://t.co/yOkPOmxU4N
Robert B Chao, MD ( View Tweet)

Watch: Ultrasound for PsA Stratification: Are We There Yet?
Dr. Aurelie Najm reports live from #ACR23
https://t.co/TnDVbKXcd4 https://t.co/RTbjL2wbUj
Dr. John Cush RheumNow ( View Tweet)
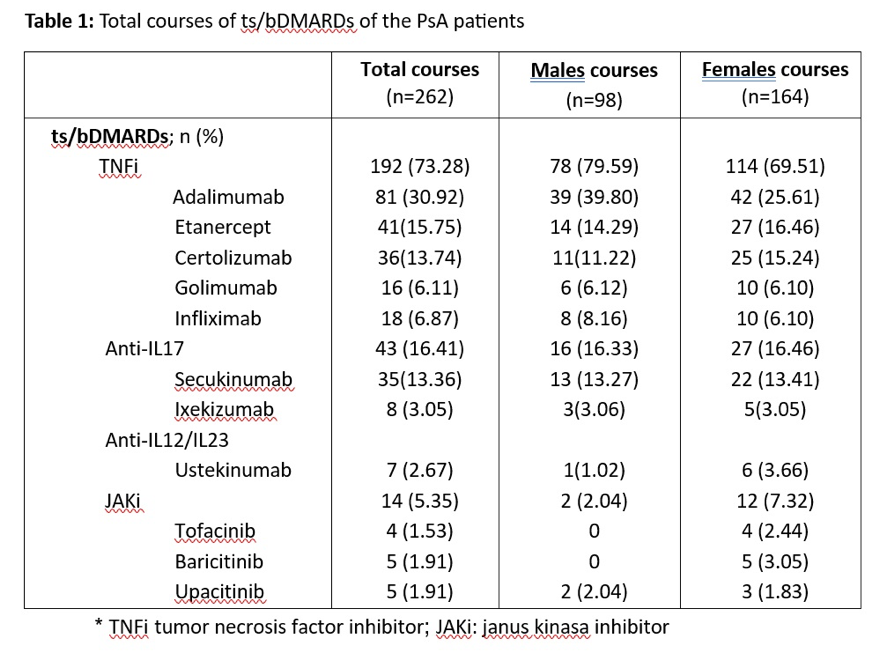
Gender differences in switching biologics in PsA pts
Women had higher biologic switch rates, mainly due to lack of efficacy
Other gender specific factors include gestational reasons and different sociodemographic features
@RheumNow #ACR23 Abs#2247 https://t.co/mLm183fCBw
Robert B Chao, MD ( View Tweet)

Be a SpA (and PsA) Sleuth! My article is your call to arms for better understanding and discovery of IBD in our inflammatory back pain patients. Consider fecal calprotectin AND robust ROS as your magnifying glass! #ACR23 @rheumnow https://t.co/OnQDEWgIWM
Dr. Rachel Tate ( View Tweet)
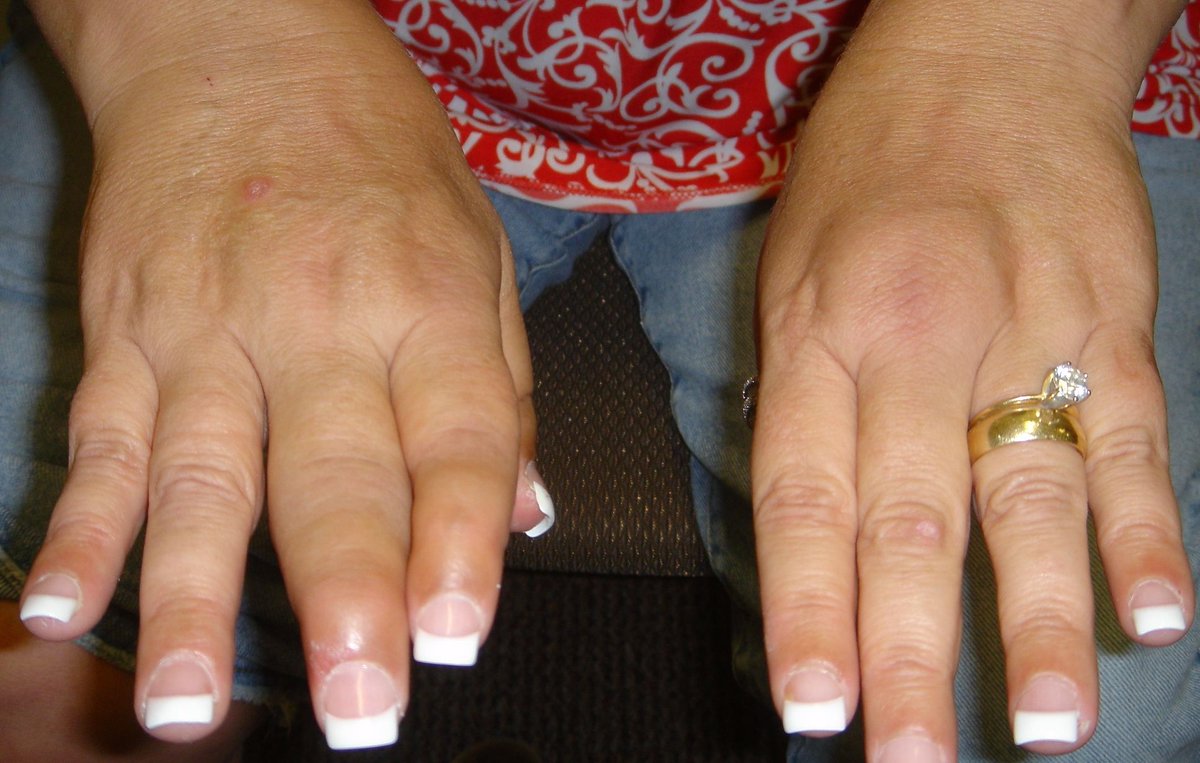
Bimekizumab is Coming… in 3rd Place
Nearly two dozen bimekizumab abstracts will be featured at #ACR23 and it recently received authorization in Europe and the US for psoriasis.
https://t.co/i2ptDnGr4a https://t.co/rZC6IORm5E
Dr. John Cush RheumNow ( View Tweet)
#irAE Baseline immune suppression does NOT protect against worsening synovitis flares when using check point inhibitors in Pts with established #inflammatory #arthritis #ACRbest #ACR23 @ACRheum @RheumNow abst1075 Data from #CanRIO database https://t.co/lOCf8Tbgta
Janet Pope ( View Tweet)
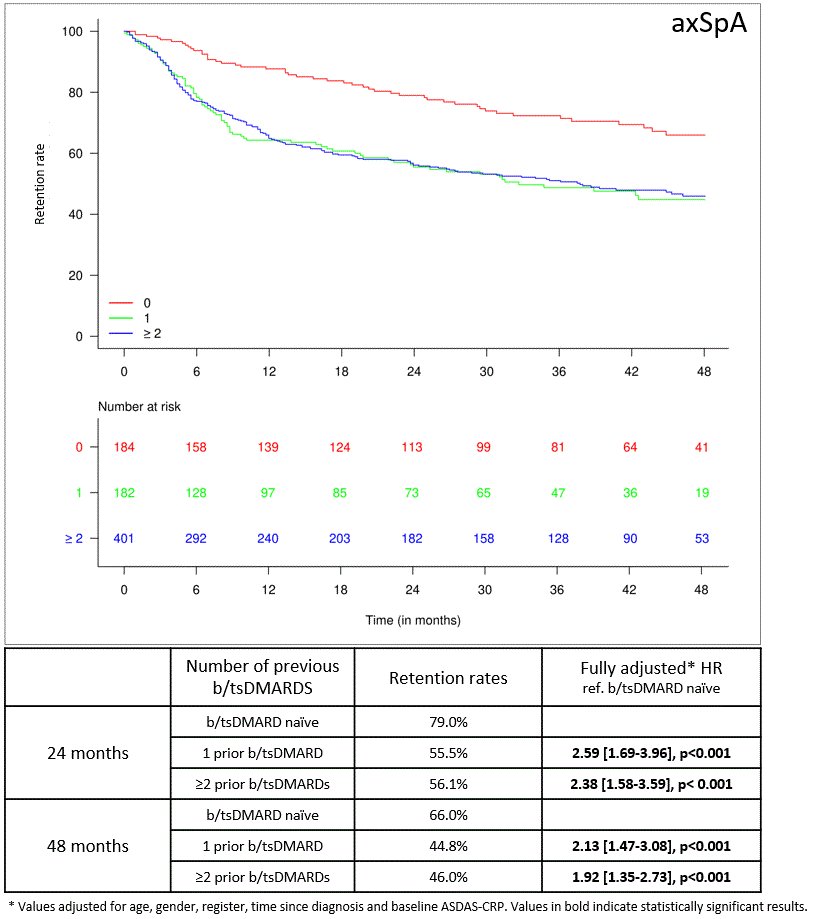
#ACR23 Abs #2199 large RL study: SEC retention rates after 4 yrs approx. 50% in axSpA and PsA pts. Bio-naïve pts had higher retention, remission & response rates than pts with prior b/tsDMARD exposure, particularly in axSpA. https://t.co/Eq5BwILK3D @rheumnow https://t.co/slho6yAwtQ
Dr. Rachel Tate ( View Tweet)
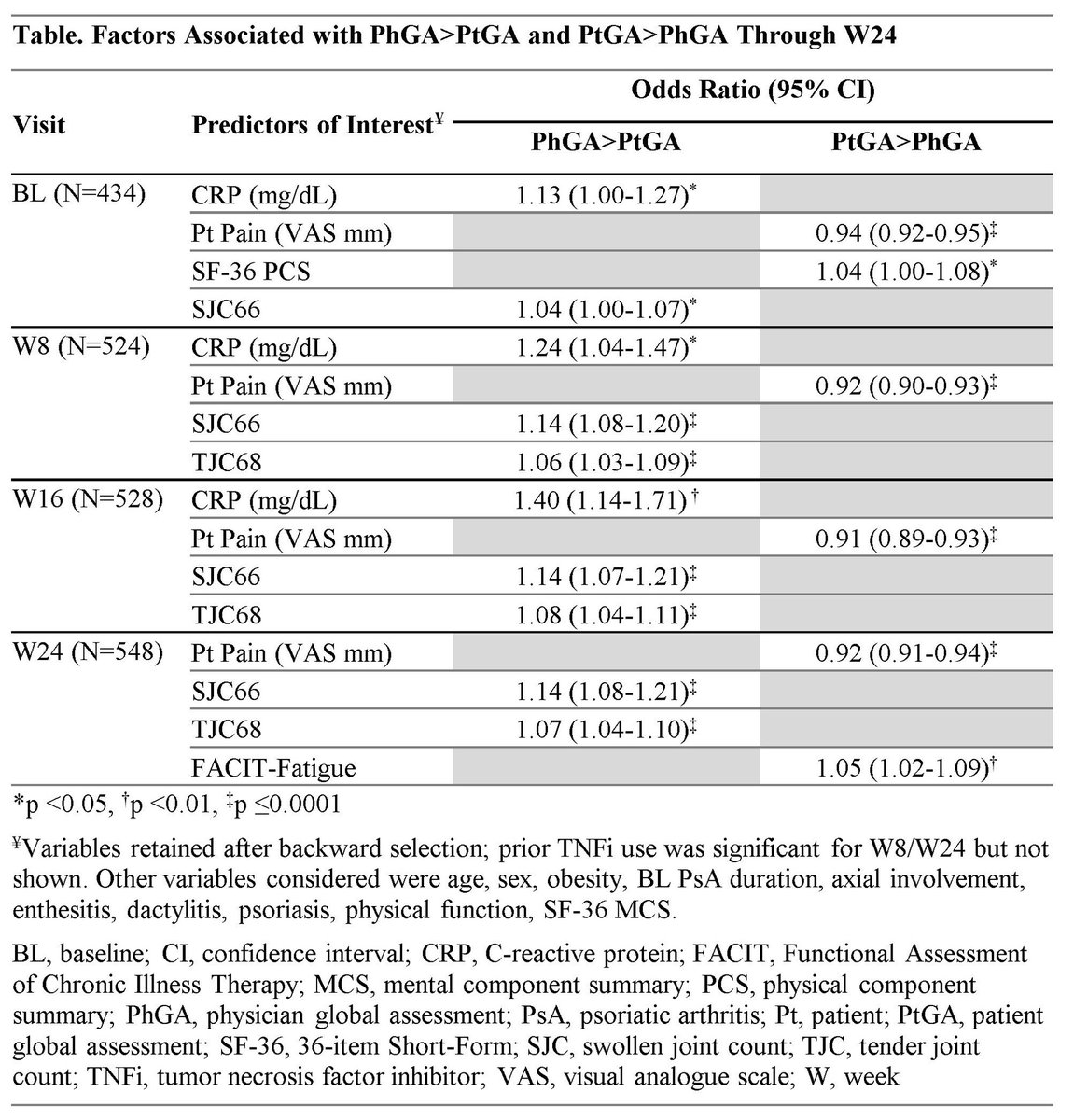
PtGA and PhGA were aligned in most encounters in PsA. PtGA >PhGA disagreement was driven by pain, fatigue, and physical health being weighed more by Pts than Phs. PROs matter! #ACR23 Abs #2234 https://t.co/0r7gjx0JS6 @rheumnow https://t.co/BuGDicwBiB
Dr. Rachel Tate ( View Tweet)
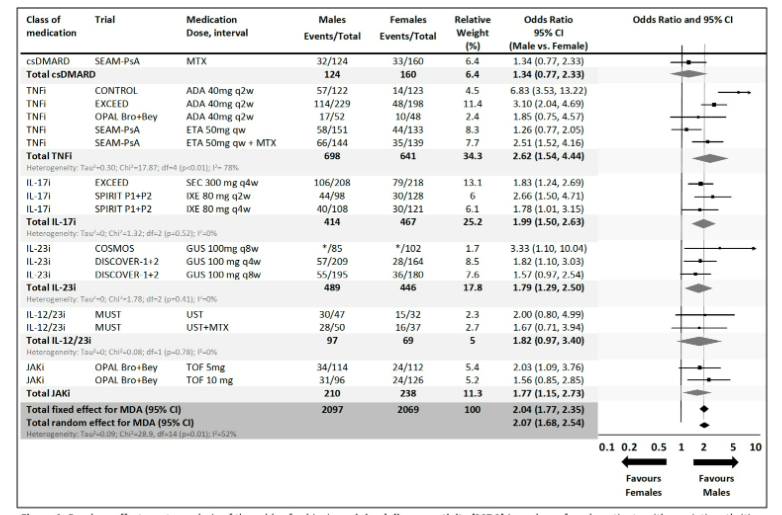
Eder et al. Women with PsA have worse outcomes with advanced therapies. OR favours men for ACR 20, IL-17i (OR 1.76), IL-23i (OR 1.46), IL-12/23i (OR 2.66) and TNFi (OR 1.67). Maybe not JAKi (OR 1.09). Placebo OR 1.04. Abstr#1687 #ACR23 @RheumNow https://t.co/bkDmmmYECF https://t.co/VBLnJzhcaY
Richard Conway ( View Tweet)
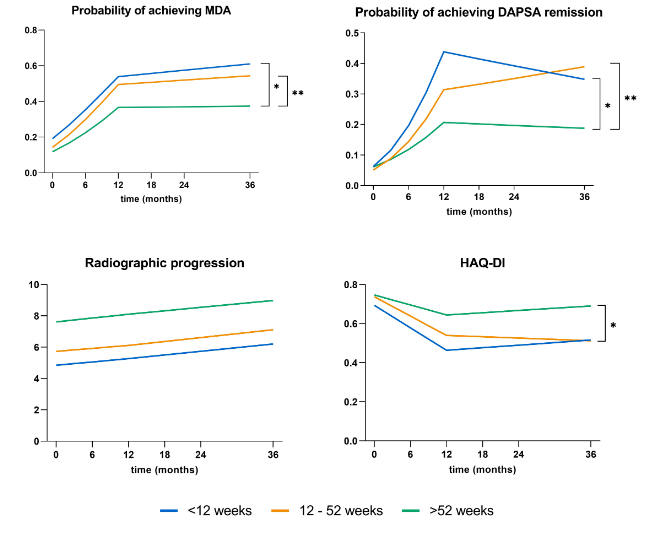
Evidence of window of opportunity concept in PsA. Certainly >52 weeks delay associates with worse outcomes. <12 weeks and 12-52 weeks similar. Abstr#1641 #ACR23 @RheumNow https://t.co/fMb3D9zl8B https://t.co/rHu29Eflo0
Richard Conway ( View Tweet)
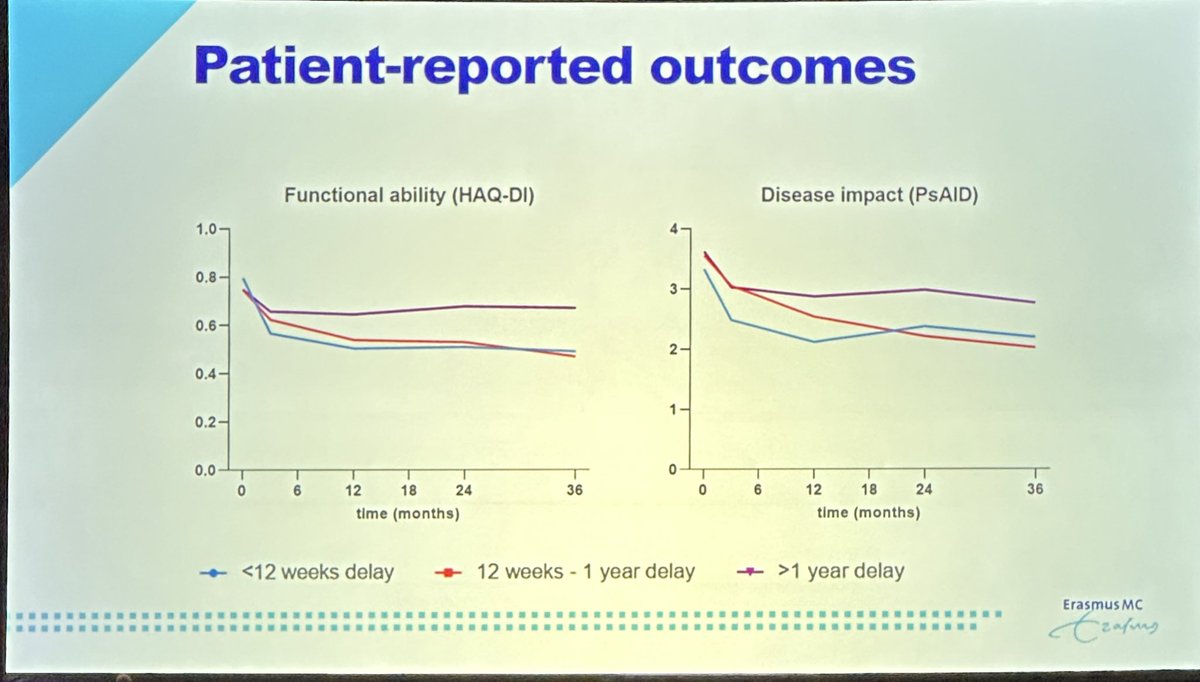
Window of opportunity in PsA
Higher time to diagnosis in
-female
-higher enthesitis
-less swollen joints
-lower CRP
If diag > 52 wks, over 3 yrs
Less MDA, less remission
Worse HAS-DI, PSAID
Same Rx progression
No diff between <12 wk & 12-52 wk
@RheumNow #ACR23 ABST1641 https://t.co/Ek1CDFwENg
Aurelie Najm ( View Tweet)
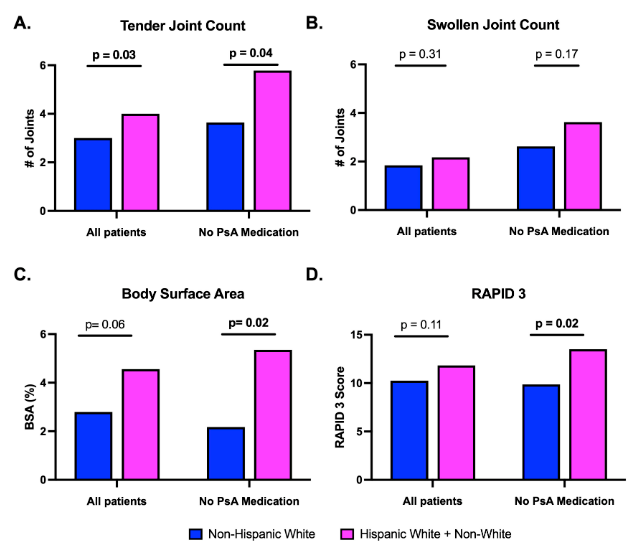
Haberman et al. In PsA non-white patients have higher tender (but not swollen) joint counts, higher radiographic axial disease, worse skin disease. Women have higher RAPID-3 scores. Abstr#1639 #ACR23 @RheumNow https://t.co/4SL7FLzNuE https://t.co/sVwk1VaSLS
Richard Conway ( View Tweet)
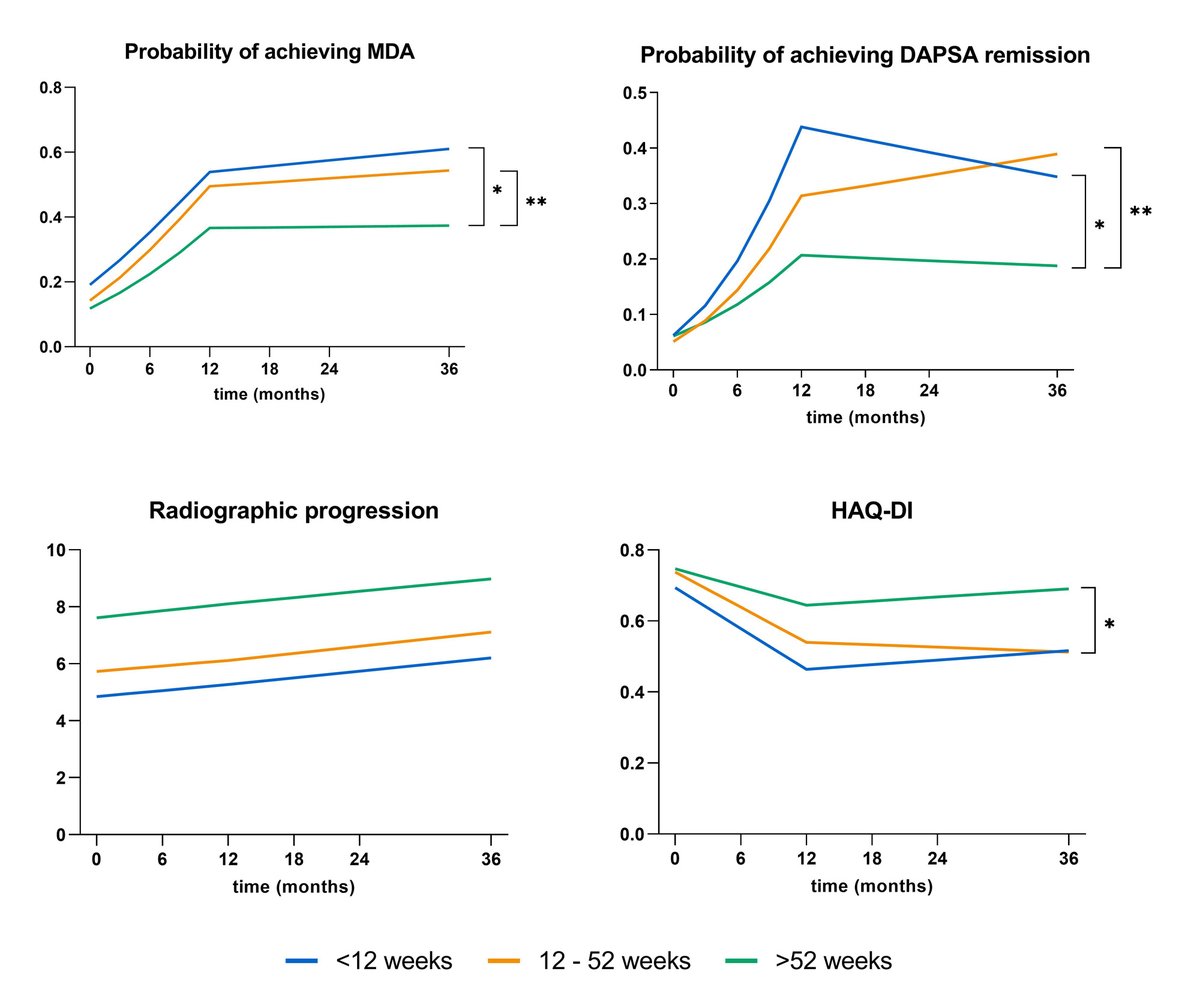
#ACR23 Abs #1641 found early referral & dx in PsA associated w/ better clinical outcomes. MDA & DAPSA remission over 3 years less likely after > 52 weeks from symptom onset to dx. Likely delays in females w/ less swollen joints & lower CRP/ ESR https://t.co/meVQ1UisKY @rheumnow https://t.co/EBN7wJfjzK
Dr. Rachel Tate ( View Tweet)
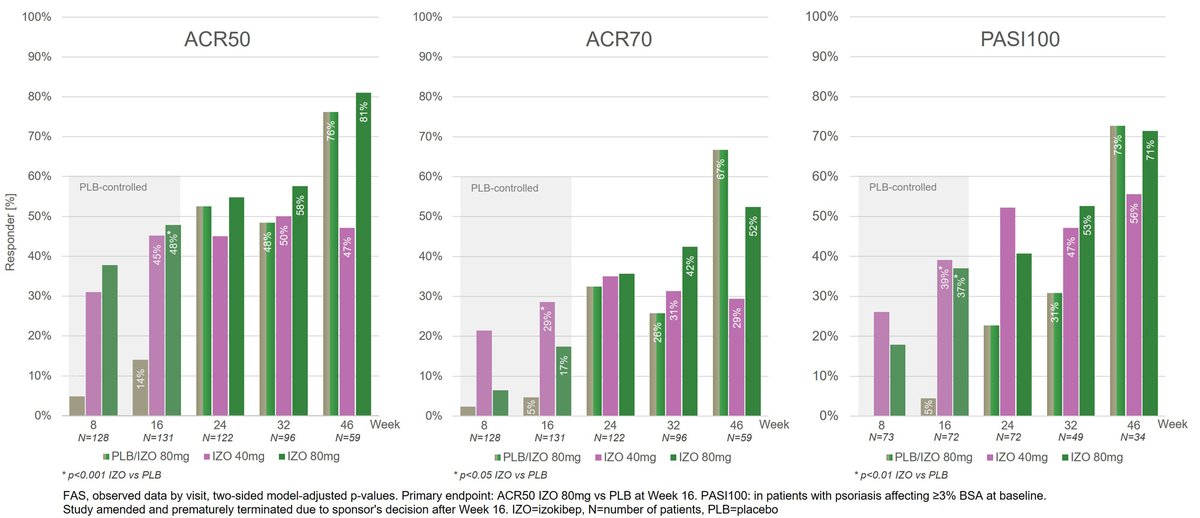
Izokibep, IL-17Ai, #ACR23 abs #1688 demonstrated ACR70 in 52%, PASI100 in 71% and enthesitis complete resolution in 89% at week 46. Well tolerated, no dose-related AEs, similar safety with other IL-17Ai https://t.co/TQAIVa9H2j @rheumnow https://t.co/ihzxnuAsWw
Dr. Rachel Tate ( View Tweet)
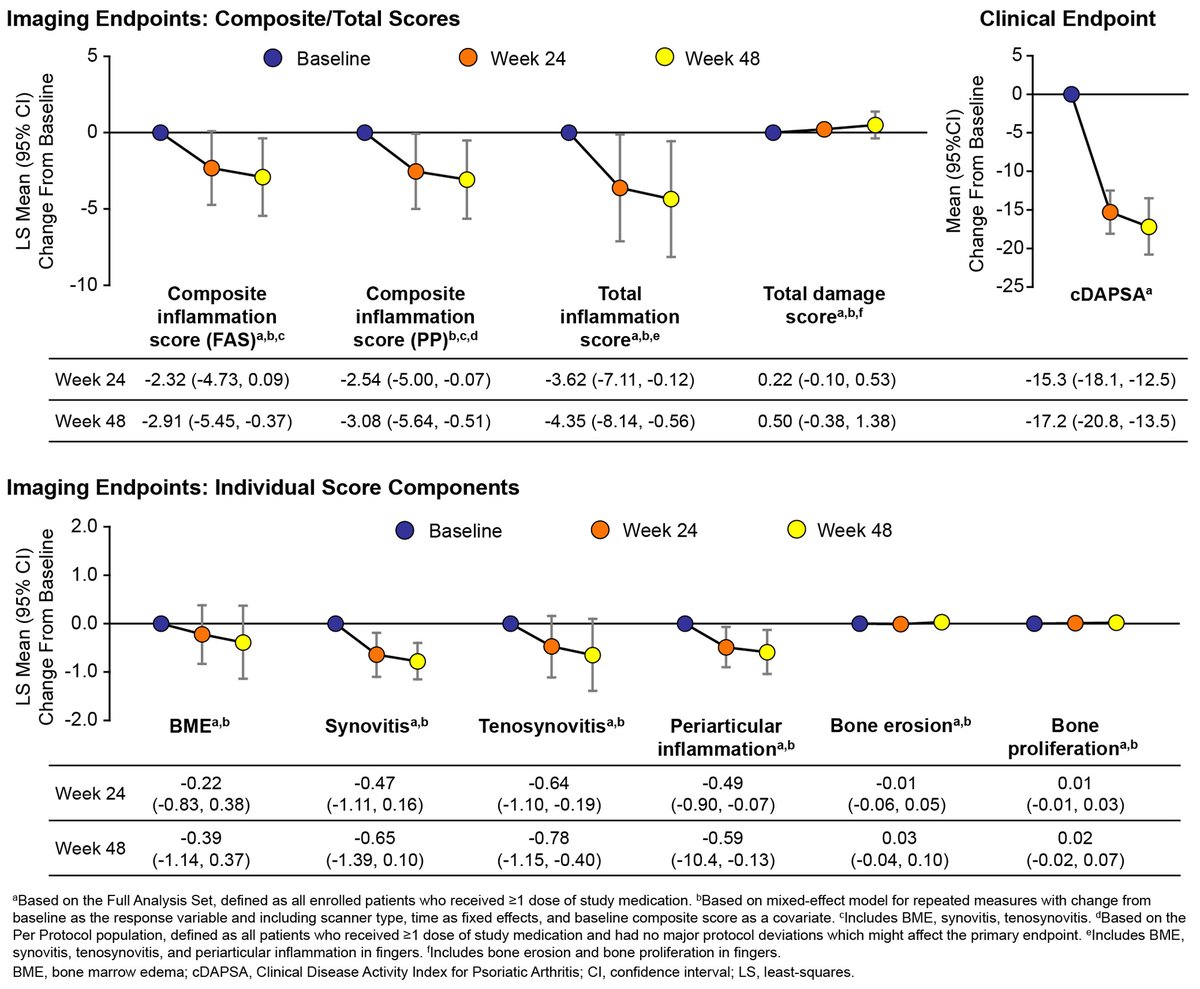
MOSAIC study: #ACR23 Abs #1690 finds APR reduces clinical and objective MRI indices in PsA, confirming an effect of APR on clinical and inflammatory manifestations of PsA. https://t.co/F5D81FF1tj @rheumnow https://t.co/rGglgiOyDg
Dr. Rachel Tate ( View Tweet)
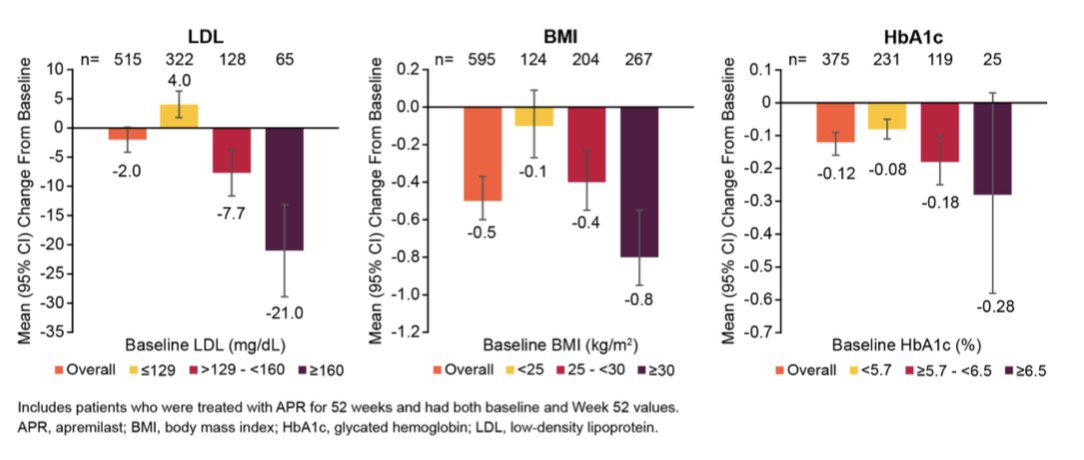
Apremilast associated with improvement in LDL, obesity and diabetic A1c in PsA pts, especially in those with worse levels at baseline!
Can consider apremilast use in PsA with high burden of comorbid cardiometabolic diseases
@RheumNow #ACR23 Abs#1414 https://t.co/fL9UWcaZgG
Robert B Chao, MD ( View Tweet)
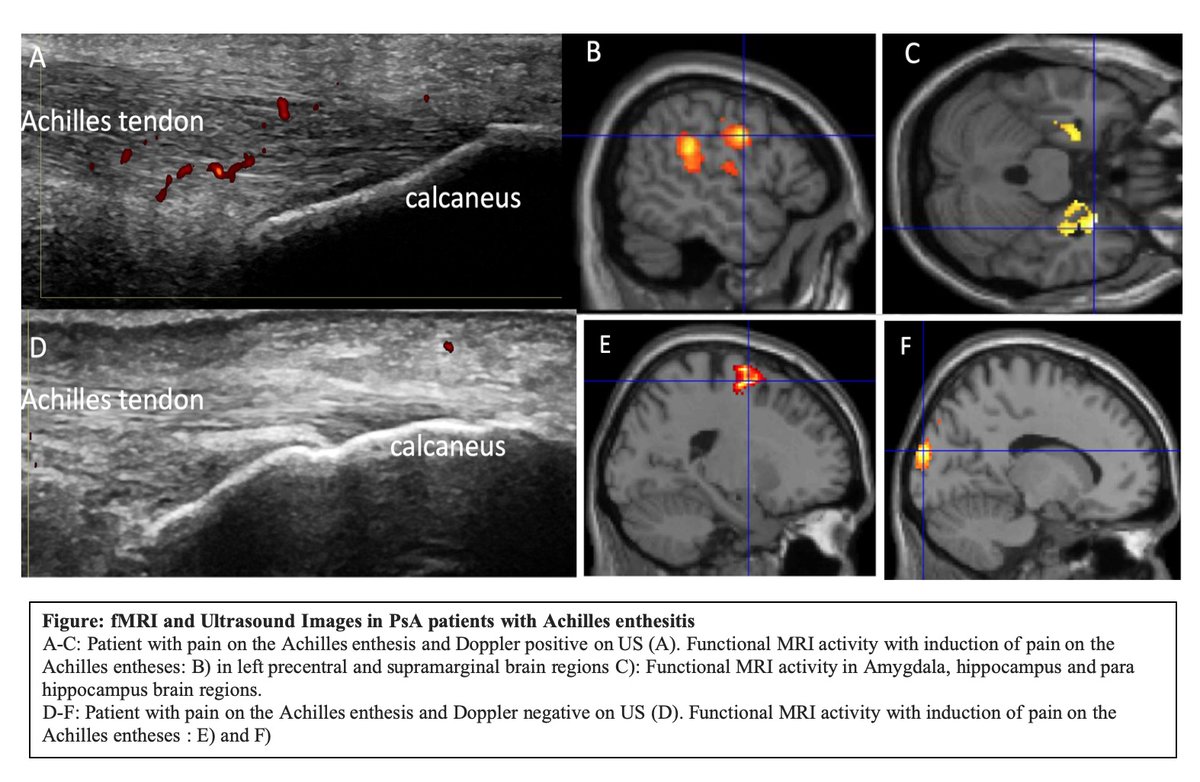
Can US differentiate pain? In #ACR23 Abs. #1388 PsA pts who have pain & inflammatory enthesitis on US, process pain differently than the US negative patients, despite the induction of pain or discomfort on all groups. Interesting finding. https://t.co/YcccLoQCBj @rheumnow https://t.co/o94bMwndxX
Dr. Rachel Tate ( View Tweet)
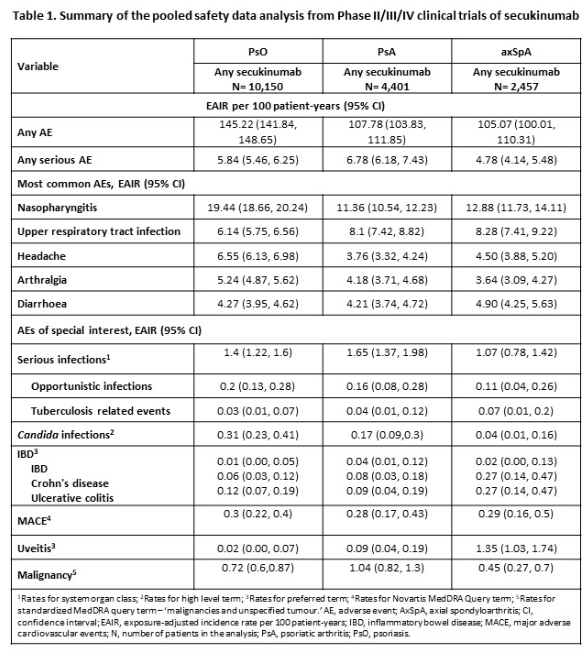
In this updated pooled safety analysis from clinical trials of PsO, PsA & axSpA pts given SEC 150 &/or 300mg SC (ADeodhar et al)
⬆️freq AEs: nasopharyngitis & URTI
Low EAIRs/100pt yrs for IBD, malignancies & MACE
No new safety signals
Reassuring data.
#ACR23 ABST1436 @RheumNow https://t.co/guF0gC4hQM
sheila ( View Tweet)
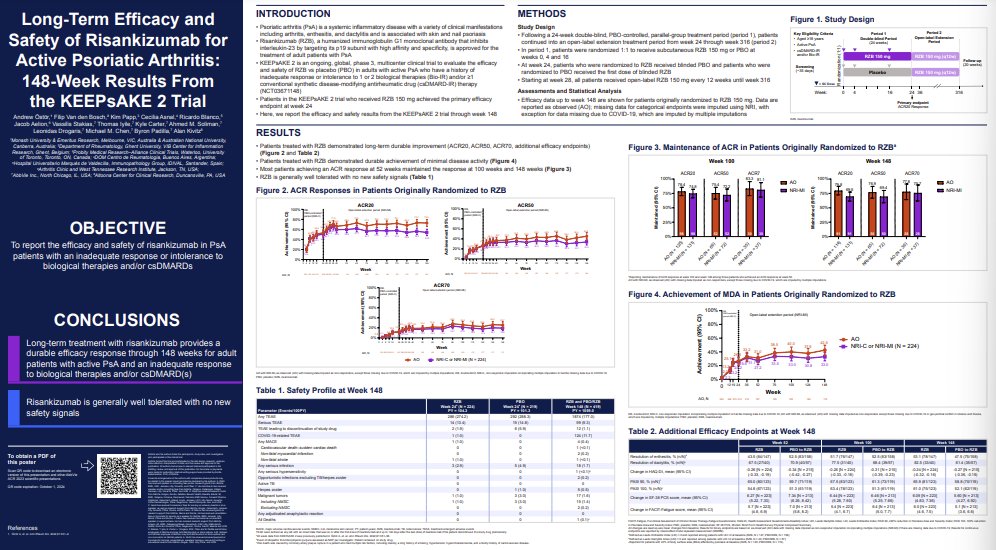
Quick curmudgeonly complaint
WHY are we doing 316 week extensions? That's 292 weeks of $$$ data... for what?
1. Insufficient N to assess meaningful safety signals
2. Open label, no comparator
It's just a very very expensive observational study
@RheumNow #ACR23 Abstr1434 https://t.co/Thj1XjeAn1
Mike Putman EBRheum ( View Tweet)