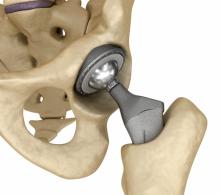
Need for Pre-operative Hyperglycemia Testing Prior to Total Joint Replacement
ICYMI: Some Good Things, During the Time of COVID-19
Best of 2020: Some Good Things, During the Time of COVID-19
Risk of Sepsis or Death Lower with Biologics in Rheumatoid Arthritis
Researchers from Germany have analyzed their large prospective rheumatoid arthritis (RA) registry to address whether being on biologic therapies leads to poorer outcomes - namely sepsis or death, following a serious infection (SIE).
They examined the outcomes of SIEs in 947 RA patients enrolled in the German biologics RABBIT registry, specifically noting the following outcomes (1) recovery, (2) sepsis following SIE (≤30 days), or (3) death after SI, without known sepsis (occurring in ≤90 days).
Lupus Hospitalizations are Common
Patients with systemic lupus erythematosus (SLE) incur substantial morbidity and complications that may lead to hospitalizations and increased cost of lupus care. Researchers from the University Health Network in Toronto have published a review of SLE hospitalizations showing thta while commone (for either infection or lupus activity), only 2.8% of hospitalizations resulted in death.
They identified all SLE hospitalizations at University Health Network between 2011–2012 and 2013–2015 to assess cause, extent of hospitalizations, and outcomes.
Cardiovascular Disease Increased in Hospitalized Lupus Patients
Systemic lupus erythematosus (SLE) patients who are hospitalized have an increased prevalence of atherosclerotic cardiovascular disease (ASCVD) and its individual phenotypes of coronary artery disease (CAD), peripheral artery disease (PAD), and cerebrovascular disease.
A nested case-control study drawn from the National Inpatient Sample, examined SLE patients (and adult controls) who were hospitalzed between 2008 and 2014. Hospitalized SLE patients (n=252,676) were matched (1:3) with non-SLE adults (n=758,034).
Anakinra Use in Hospitalized Gout Patients
Poor Outcomes for Dermato/Polymyositis Admitted to ICU
Idiopathic inflammatory myopathies (IIMs) may be complicated with life-threatening conditions requiring intensive care unit (ICU) admission. The outcomes of such complications may be dire, but there are few series addressing the outcomes of those admitted to the ICU.
In a retrospective study of IIM patients from a tertiary referral center in China, Peng and colleagues recount the clinical features and outcomes and risk factors for mortality among 102 patients admitted to the ICU.
RABBIT Risk Scores are Higher in ICU-Admitted RA Patients
The German Rheumatoid Arthritis Biologics Registry (RABBIT) has developed an infectious risk calculator that can project a patient's risk of serious infection in the next 6 months based on several key factors - age, Prior DMARDs, prednisone dose, comorbidities and the biologic intended for use. (This can be found at http://www.biologika-register.de)
Predicting Inpatient Gout Flares
Analysis of New Zealand hospitalized patients revals nine predictors of inpatient flare for people with comorbid gout.
This retrospective cohort study of hospitalised patients with comorbid gout included 625 hospitalised patients, 87 experienced inpatient gout flare.
There were 9 predictors of an inpatient gout flare:
The House of God After 40 Years: A Rheumatologist's Reflection
Kids' COVID-Linked Ailment Is Not Your Typical Kawasaki Disease
As data continue to emerge about a multi-system inflammatory disorder in children apparently connected to COVID-19, evidence is growing that this is not your typical Kawasaki disease.
In New York, up to 102 children have reportedly developed this inflammatory syndrome, and three children have died from it in the state as of Wednesday. Other cases have been reported in Washington, California, and elsewhere in the U.S. as well as in Europe.
Psoriasis and Psoriatic Arthritis Have an Increased Risk of Gout
The frequency of gout among patients with psoriatic disease was studied in two cohorts of 98,810 patients from the Health Professionals Follow-up Study (1986-2010) and the Nurses' Health Study (1998-2010). (Citation source http://buff.ly/1U1wchB). Psoriasis and PsA were associated with an inceased risk of gout. Incident gout cases were higher in patients with psoriasis (HR 1.71) and also in patients with psoriatic arthritis (HR 4.95).
Psoriasis Patients Satisfied with Biologics
A recent study published in the journal Patient Preference and Adherence examined insured patients from the Optum Research Database who had moderate to severe plaque psoriasis and queried them about their satisfaction with therapy. (Citation Source http://buff.ly/1MpWMQg)
Ustekinumab Effective in Adolescents with Psoriasis
Biologic and new drug development seldom targets children and adolescents. This study evaluated the efficacy and safety of ustekinumab in adolescents age 12 to 17 years with moderate-to-severe psoriasis,
Modest Efficacy for Methotrexate in Psoriasis
Get Ready for ICD-10
With three months until the switch from ICD-9 to ICD-10 coding, CMS and the AMA have announced efforts to continue to help physicians get ready ahead of the October 1 deadline. They will offer webinars, on-site training, educational articles and national provider calls to help physicians and other health care providers learn about the updated codes and prepare for the transition.
ICD-10 Tips for Procrastinators
On October 1st, your coding memory will be getting a big and unwelcomed upgrade.
Even if the goverment shuts down, ICD-10 implementation goes forward.
Below are several sources to review what's ahead and what you should be focused on at this point.
More Knee Replacements at Younger Ages
The National Hospital Discharge Survey shows that between 2000 and 2010, more than 5.2 million total knee replacements were performed in the United States. By 2010, the operation had become the leading inpatient surgery performed on adults aged 45 and over. Moreover, the rate at which middle-aged and older Americans got their knees replaced almost doubled over the study period.
Checkpoint Inhibitors Causing Rheumatic Disease
Calabrese and Velcheti have reviewed the current understanding that underlies a new drug-induced rheumatic disease - checkpoint inhibitor arthritis and autoimmune disease.
The approval and use of new cancer drugs in solid tumors has focused on key checkpoints, including the programmed death-1 (PD-1) pathway (pembrolizumab, nivolumab and atezolizumab) and cytotoxic T-lymphocyte-associated protein 4 (CTLA4) (ipilimumab) activity. While these agents have proven benefits, the down-side includes the development of several autoimmune inflammatory conditions.
Interferon Blocker Disappoints in SLE
Yet another setback has occurred in the efforts to develop new medications for treating systemic lupus erythematosus (SLE), as anifrolumab failed to meet the primary endpoint in a phase III trial, according to AstraZeneca and MedImmune.
Only one new drug, belimumab (Benlysta), has been approved for use recently in SLE. When belimumab was licensed in 2011, it was the first drug specifically approved as a lupus treatment in more than 50 years. Since that time, other agents that have had negative results included tabalumab, epratuzumab, and atacicept.
Dramatic Results for Interferon Blocker in SLE
Blocking the type 1 interferon receptor with the monoclonal antibody anifrolumab shows promise as a treatment for moderate-to-severe systemic lupus erythematosus (SLE), according to a phase IIb study presented here.
SynBioSe: Combo Rituximab and Belimumab Succeeds in Severe Refractory Lupus
One of the driving pathogenic mechanisms in systemic lupus erythematosus (SLE) is the generation of immune complexes capable of inducing netosis (NET formation) and NET-derived DNA that may be an amplifying autoantigen and give rise to anti-nuclear autoantibodies (ANAs).
Researchers from Leiden University Medical Center in The Netherlands sought to target autoreactive plasma cells and interfere with immune complex formation and netosis in SLE by treating patients with a combination of rituximab (RTX) and belimumab (BLM).
The Unmet Need in Rheumatoid Arthritis Therapy
Not all patients respond to methotrexate (MTX) or their intial therapy for rheumatoid arthritis (RA). The Norwegian DMARD (NOR-DMARD) registry assessed the outcomes of MTX and bDMARD treated patients and found a signfificant unmet need still for patients experiencing inadequate response to MTX monotherapy and bDMARDs 12 months of therapy.
To describe the outcomes of MTX and biologic DMARD (bDMARD) treatment in patients with RA and assess unmet needs in patients who fail treatment, using real-world data from the Norwegian DMARD (NOR-DMARD) registry.
Infliximab Use Near Surgery is Safe
Rituximab Safety Concerns when Used in anti-TNF Refractory RA
The SUNSTONE study evaluated the long‐term safety of rituximab in rheumatoid arthritis (RA) previously exposed to ≥1 anti–tumor necrosis factor inhibitors (TNFi) and showed a stable, but high, rate of serious infections, opportunistic infections and an overall higher mortality rate.
DMARD Inertia by Registry Rheumatologists
A registry study of metric use (primarily RAPID3 and CDAI) in the treatment of rheumatoid arthritis (RA) patients shows that, even in the face of moderate or high disease activity, treatment changes by rheumatologists were relatively low (35.6–54.6%).
Researchers used data from the ACR supported Rheumatology Informatics System for Effectiveness (RISE) registry to assess the influence of disease activity measuress on treatment use over 12 months.
Infusions in the Time of Coronavirus
As they say, necessity is the mother of invention. After years of bemoaning the challenges of telemedicine, our rheumatology clinic transition entirely to a remote clinic in the space of a week. One of the few good things to come out of this crisis is that we may learn that in-person visits are not as critical as we thought, which may in turn help our specialty’s access issues.
The only thing we can’t do remotely, however, are infusions.