All News
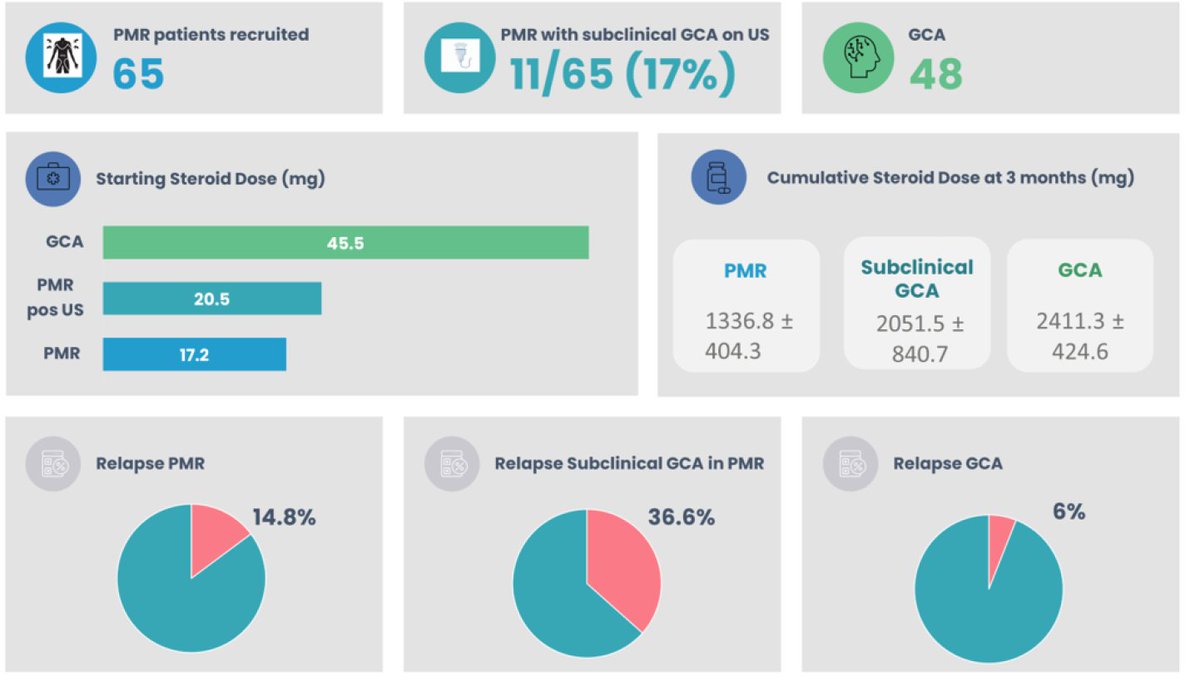
Baseline vascular ultrasound predicts clinical outcomes @ 3 months. Subclinical GCA = relapse 37% vs 15%. Higher cumulative steroid dose. @sharoncowley01 @DrTrishHarkins Abstr#1565 #ACR23 @RheumNow https://t.co/b35CkFS0lz https://t.co/suBGR1ByDK
Richard Conway ( View Tweet)

So firstly the no case, and Rob Spiera takes up the case, dictated by the electronic coin toss.
No-one disagrees that we need steroid-sparing options, or that IL-6Ri work in PMR and GCA. But it’s the strategy questions which remain in play:
#ACR23 @RheumNow https://t.co/I2QDU7l6DE
David Liew drdavidliew ( View Tweet)

@RheumNow #ACR23 #GreatDebate
Use Advanced Rx for GCA 1st line?
Spiera: No
No ev for disease modification with early Rx
Lose only reliable biomark of dis activity w IL-6 inhib
No evid of reduced major GC AEs
$$
GCA: treat by GC alone, taper off by 6 m, low threshold to escal https://t.co/QxgAlVKitd
Eric Dein ( View Tweet)

@RheumNow So what might early steroid-sparing therapy in PMR/GCA achieve?
Cure? Superior disease activity control? Minimize damage? Improve QoL/function?
Well, sadly we have a long way to go in defining a lot of this:
#ACR23 @RheumNow https://t.co/QeidAHHm8x
David Liew drdavidliew ( View Tweet)

@RheumNow So in GCA, we don’t know if therapies can truly disease modify at all. There’s a lot of grumbling disease, and it’s unclear whether we can stop long-term vascular issues. And in PMR, we have very little data on early therapy at all.
So what’s the justification?
#ACR23 @RheumNow https://t.co/spAMqfSOy2
David Liew drdavidliew ( View Tweet)

#ACR23 @RheumNow #GreatDebate
Treatment for PMR by Spiera
- Plan rapid GC taper. It is OK to flare, prepare pt!
- Low threshold to introduce anti-IL-6 for GC intolerance or AEs
No need for initial biologic treatment for PMR/GCA
@philseo rebuttal upcoming... https://t.co/A0f3b0fMOr
Eric Dein ( View Tweet)

Should IL-6i be first line in GCA/PMR? Dr. Spiera says steroids work, are cheap; no evidence of using IL6i early in disease. there had been cases where pts still had active vasculitis while on IL-6i. He starts with steroids first then add IL6i #GreatDebate #ACR23 @rheumnow https://t.co/Oq5Q9HFtW3
TheDaoIndex KDAO2011 ( View Tweet)

#ACR23 #Debate Dr Spiera says NO need to up front use #glucocorticoid #sparing drugs in PMR - maybe only if flaring. Esp in PMR vs #GCA where maybe bDMARD in GCA in some Pts (my opinion) but for sure if failing #ACRbest #ACR23 @RheumNow @ACRheum https://t.co/Rt7rGZv3fW
Janet Pope ( View Tweet)

1-Can we prevent RA ? Vagotomy?
2-CV events in auto immune rheumatic disease pregnancies.
3-CVS vasculitis , challenges and role of Brain biopsy
And others……..
https://t.co/BX8bDSX1M3
@RheumNow , daily recap
#ACR23
Nouf Al hemmadi ( View Tweet)

⭐️Real world data on use of #avacopan presented by @zach_wallace_md
#vasculitis
Important observations to inform the practice and management of #AAV https://t.co/gtZORcnt9t
KenWarringtonMD MdWarrington ( View Tweet)

Real-life data about the PEXIVAS reduced-dose glucocorticoid regimen in #granulomatosis with polyangiitis and microscopic #polyangiitis (Abstract 0725 https://t.co/7x34Hr0OMP)
@TerrierBen
#ACR23
#ACRambassador https://t.co/D8UfZvXQCl
Alessia Alunno ( View Tweet)

Reduced-dose GC regimen in severe GPA or MPS (creatinine >300 umol/L, RTX as induction) associated with increased risk of death, ESKD, progression before remission requiring treatment modification or relapse, Nagle S Abst#0725 #ACR23 #ACRBest @RheumNow https://t.co/ZVZYRnSy3n
Dr. Antoni Chan ( View Tweet)
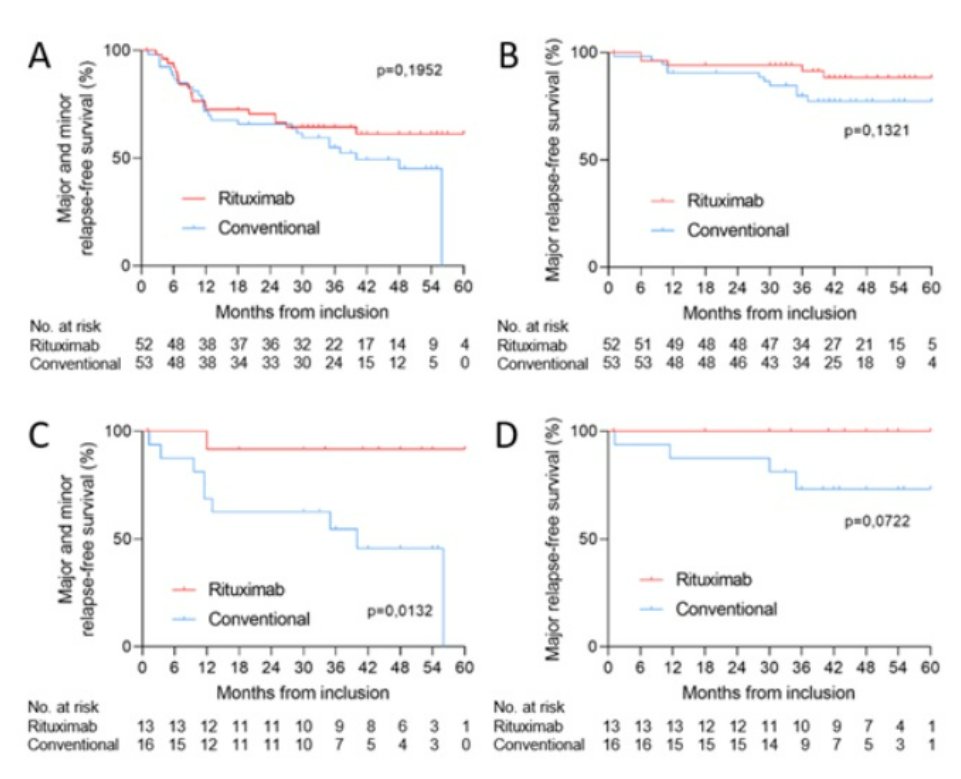
LTE of REOVAS of RTX in EGPA. Relapse free survival 64% vs 51%, major relapse free 90% vs 79%. If MPO+ relapse free survival 92% vs 50%. Abstr#0854 #ACR23 @RheumNow https://t.co/76hlYRxWhY https://t.co/RSsgxxQKVC
Richard Conway ( View Tweet)

Clinical pearls in #CNS vasculitis: Dr. R.Hajj-Ali
🧠Clinical dx is difficult bec it presents w/ an array of clinical features
🧠CSF analysis essential in dx; can r/o infexns
🧠Nonvasc imaging highly sensitive
🧠biopsy is valuable esp when alt dx is considered
#ACR23 @RheumNow https://t.co/QOAfSHn8ND
sheila ( View Tweet)
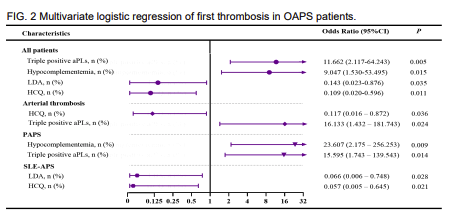
Risk factor for 1st Thrombosis in OB APS
Ab#0115 #ACR23 @RheumNow
186 OAPS pts, followed mean 5.4 yrs. 11 thrombotic events
Risk factors: Triple pos APS Abs (OR 11.6), hypocomplementemia (OR 9)
Low dose Aspirin (OR 0.14), HCQ (OR 0.11) reduced thrombosis
#ACRBest https://t.co/y4KaEAZzA7
Eric Dein ( View Tweet)

Important plenary re:reduced vs standard GC for AAV... IRL
PEXIVAS & recent guidelines supported low dose taper
Real world data w/severe dx? Increased risk of death & ESKD for REDUCED pts
Need full data but yikes...
@RheumNow #ACR23 #ACRBest https://t.co/3S23O9d1ok
Mike Putman EBRheum ( View Tweet)
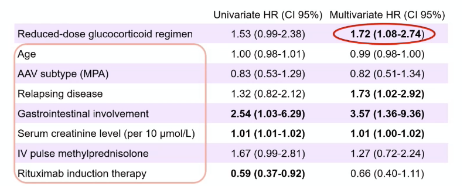
Abst#0725 #ACR23 @RheumNow
PEXIVAS Real life data!
GPA & MPA pts - Retrosp observ study
⭐️Reduced-dose GC regimen ass w/ INCREASED risk of death, ESKD, progression
Greatest risk: pt w Cr levels >300 umol/L, RTX induction Rx
⚠️Caution w/ reduced GC, RTX, severe kidney dis
#ACRBest https://t.co/7qI5c1ZiqO
Eric Dein ( View Tweet)
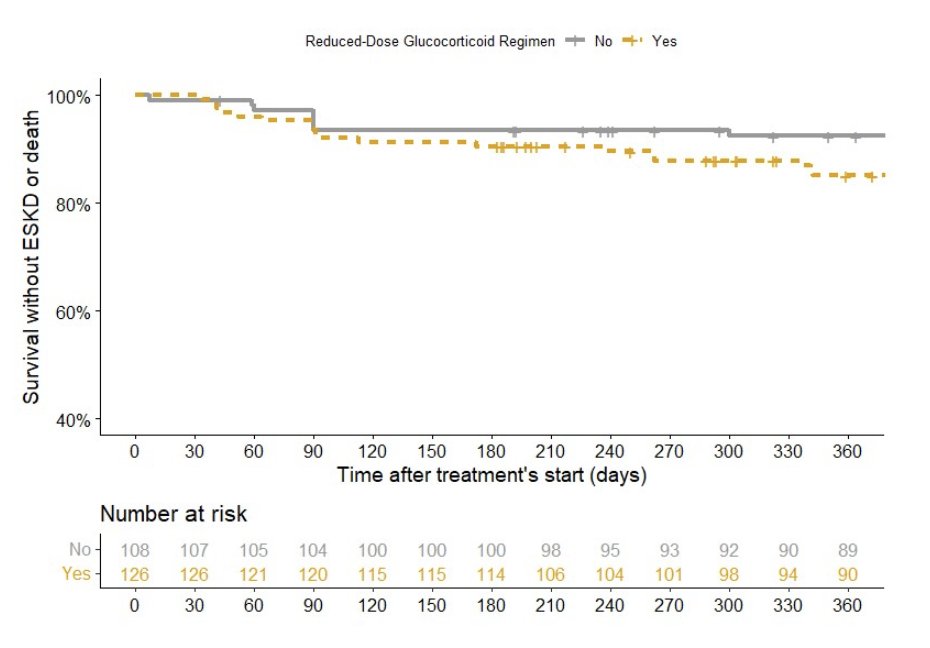
Interesting study on PEXIVAS reduced steroid use from today's plenary session!
Reduced steroid dose in GPA/MPA pts associated w/
INCREASED risk of death, ESKD, progression of dz
Even greater risk in pts with higher Cr lvls or RTX induction use
@RheumNow #ACR23 Abs#0725 #ACRbest https://t.co/frsOrANKhf
Robert B Chao, MD ( View Tweet)
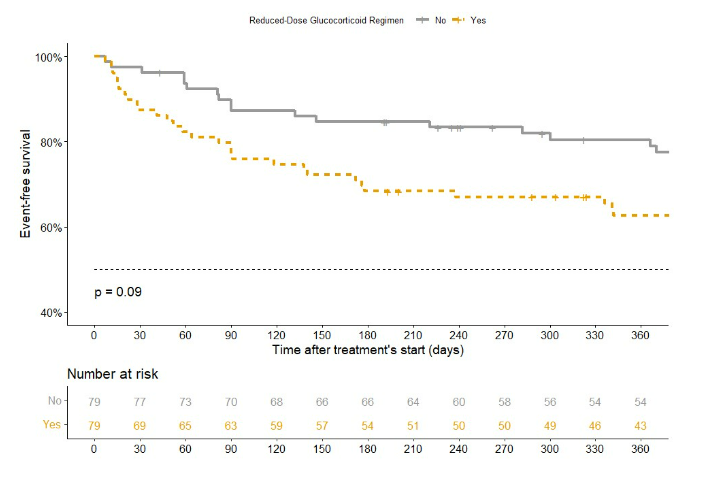
Real world data on low dose PEXIVAS steroid by Nagle et al. Increased risk of progression/relapse/death/ESKD in those with severe GPA/MPA HR 1.72. More marked in those with creat>300 or with RTX induction Abstr#0725 #ACR23 @RheumNow https://t.co/vTXVZfjbXx https://t.co/4FuMjxOuyB
Richard Conway ( View Tweet)
ACR Convergence Preview (11.10.2023)
Dr. Jack Cush reviews this past week's news on RheumNow.com and suggests a learning plan for those wanting to consume the upcoming ACR Convergence 2023 meeting.
Read Article
