All News
Belimumab Effective in Lupus Nephritis
Dr. Rich Furie has lead a group of investIgators in reporting the significant efficacy of intravenous belimumab when added to standard of care induction therapy in patients with active lupus nephritis. This phase 3, 2-year study included 448 systemic lupus erythematosus patients with biopsy proven lupus nephritis (class III or IV +/- V) patients who required induction therapy and have a UPCR ≥1 g/g.
Read ArticleUpdated List of Drugs Inducing Lupus
Drugs inducing lupus may account for nearly 30% of all subacute cutaneous lupus erythematosus (CLE) and up to 15% of systemic lupus erythematosus (SLE) cases. Moreover there are over 100 drugs capable of inducing drug-induced lupus erythematosus.
Read ArticleACR 2020 Reproductive Guidelines - Contraception & Counseling
The American College of Rheumatology established a guidelines committee that consisted of both patients, rheumatologists and maternal-fetal health experts. After a a systematic review of the medical literature regarding contraception, assisted reproductive technology, fertility preservation, hormone replacement therapy pregnancy, lactation, and medication use in rheumatic disease patients, they published 12 good practice statements and 131 recommendations for reproductive health care in RMD patients.
Read ArticleCDC: COVID Seroprevalence in Health Care Workers
CDC reports that gmong 3,248 healthcare personnel (HCP) observed, 6% had antibody evidence of previous SARS-CoV-2 infection; 29% of personnel with SARS-CoV-2 antibodies were asymptomatic in the preceding months, and 69% had not previously received a diagnosis of SARS-CoV-2 infection.
Read ArticleIncreased Lupus Anticoagulant Activity in COVID-19 Infection
JAMA Network Open reports that after adjusting for inflammation, lupus anticoagulant (LA) is significantly increased (positive) in COVID-19 patients and that LA positivity was associated with incidence risk of thrombotic events.
Read ArticleRheumNow Podcast - Top 13 Rheumatology Centers (7-31-20)
Dr. Jack Cush reviews the news and TOP 13 list of Best Rheumatology Hospitals.
Read ArticleLow Risk of COVID in Biologic Treated Rheum Patients
In an Annals of Rheumatic Disease report, Italian investigators performed consecutive testing for SARS-CoV-2 (IgM and IgG) between 25 March to 25 May 2020 and compared test results between rheumatic disease (RMD) patients and the general population.
Read ArticleHigher Rates of SARS-CoV-2 Seropositivity in the USA
The number of reporting cases of COVID-19 infection tends to underestimate the true prevalence of infection as only the more severe cases (e.g.,acute respiratory syndrome) get tested or go to the hospital. JAMA Internal Medicine reports that a cross-sectional seroprevalence study from the U.S. shows that COVID-19 is underreported and that actual infection rates can be 6 to 24 times more prevalent than currently reported infections due to SARS-CoV-2.
Read ArticleSteroids and Tocilizumab in Cytokine Storm Syndrome
A recent study from the Netherlands has shown that patients with severe COVID-19-associated cytokine storm syndrome (CSS) with high dose steroids and tocilizumab had a faster recovery, less need for invasive mechanical ventilation and fewer deaths when compared to CSS patients receiving supportive care only.
They studed COVID-19 patients with CSS, defined as rapid respiratory deterioration plus at least two of the following biomarkers: a) C-reactive protein >100mg/L; b) ferritin >900 µg/L; or c) D-dimer >1500 µg/L.
RheumNow Podcast – LTF – Listen to Fauci (7.17.20)
Dr. Jack Cush reviews the news, tweets and journal articles from the past week on RheumNow. Let's dig into this week's 14 highlights.
PRIME Cells Predicting Rheumatoid Arthritis Flares
The current issue of NEJM reports a novel cell type that may be used to identify rheumatoid arthritis (RA) patients who may flare.
Investigators prospectively collected blood samples from 4 patients for longitudinal RNA sequencing (RNA-seq) for discovery of moleculartranscripts that were differentially expressed before flares.
Anti-Rheumatic Therapies for COVID-19 Infection
Since the onset of the COVID-19 pandemic numerous anti-rheumatic therapies have been proposed as being potentially beneficial. The mechanistic effects of these agents, either presumed antiviral, anti-inflammatory and anti-thrombotic effects, may benefit mitigate the damage seen with COVID-19 infection.
This review will examine the potential benefits and existing evidence for treating suspected or proven COVID-19 infection with antimalarials, inhibitors of interleukin-6 (IL-6) or interleukin-1 (IL-1) Janus kinase (JAK) inhibitors, TNF inhibitors or colchicine. There are many other antirheumatic and immunosuppressive therapies that are in clinical trials that will not be reviewed here including IVIG, rituximab, calcineurin inhibitors (sirolimus, etc.), apremilast, emapalumab (anti-IFN gamma), etc.
COVID's Multisystem Inflammatory Syndrome in Children
Two recent reports further characterize the newly described, Kawasaki-like, syndrome affecting children with COVID-19 infections.
The NEJM describes the childhood syndrome as having Kawasaki’s disease, fever, toxic shock syndrome, acute abdominal conditions, and encephalopathy; hence the label Childhood Multisystem Inflammatory Syndrome. The disorder emerged in late April 2020, first in the U.K., and then similar cases were reported from many other countries. The CDC named this multisystem inflammatory syndrome in children (MIS-C).
Methotrexate May Enhance Pegloticase Response in Gout
For patients with gout exacerbations while on pegloticase (Krystexxa), adding methotrexate may help reduce uric acid levels, researchers suggested at the European League Against Rheumatism (EULAR) virtual meeting.
In a small open-label study of 14 patients experiencing acute gout attacks, use of the pegloticase/methotrexate combination reduced uric acid levels to near undetectable levels in 11 patients, reported John Botson, MD, medical director of Orthopedic Physicians Alaska in Anchorage. He noted that this was far below the 5 mg/dL level recognized as the threshold for development of inflammation that causes gout attacks.
Day 3 - Top 5 from EULAR 2020
These were my top abstracts from Thursday, 4th of June at EULAR 2020:
Read ArticleFDA Approves Taltz for Non-Radiographic Axial Spondyloarthritis
Today Eli Lilly announced that Taltz (ixekizumab) has received FDA approval for the treatment of adults with active non-radiographic axial spondyloarthritis (nr-axSpA).
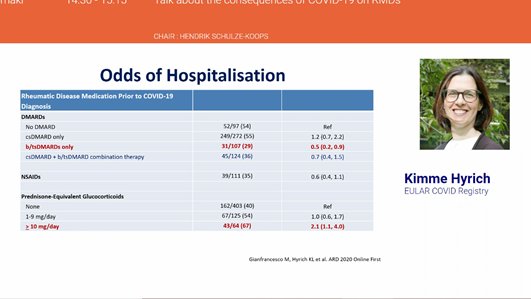
Read ArticleFirst Look at COVID-19 Global Rheumatology Alliance Registry
Gianfresco et al have published the first peer-reviewed analysis of COVID-19 infected, rheumatic disease patients entered into the Rheumatology Global Alliance registry; showing that a) rheumatic disease patient can be infected with COVID-19, b) that DMARD and biologic use has no apparent effect on outcomes and c) steroid increase and TNF inhibitor decrease the odds of hospitalization.
Read Article
Links:
Dr. John Cush RheumNow ( View Tweet)

Dr. John Cush RheumNow ( View Tweet)