The Red Eye in the Rheumatology Patient Save
Professor Rosenbaum is well known for his expertise in rheumatic eye disease and he gave a great summary of how to approach your patient having a red eye.
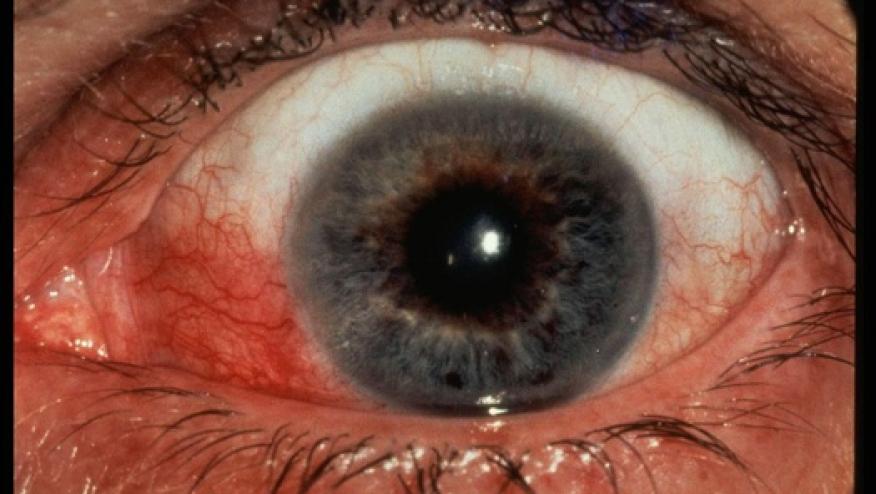
The differential diagnosis for the red eye includes conjunctivitis, keratitis, acute anterior uveitis, episcleritis, scleritis and acute closed angle glaucoma.
An easy mnemonic to use with your patients with red eye is R-S-V-P. You need to ask if patients have persistent Redness (R), Sensitivity to light (S), reduced Visual acuity (V) or Pain (P). If patients have any of these symptoms then the patient needs to have an ophthalmological consult.
It is important to remember that the most frequent cause of red eye in rheumatoid arthritis is dry eye. Episcleritis and scleritis can occur in RA but it is much less common. When thinking about dry eye the obvious cause to a rheumatologist is Sjogren Syndrome, but it important to exclude other causes which include previous radiation, hepatitis C, HIV, sarcoidosis, amyloidosis, IgG4 disease and graft versus host disease.
Important things to think about treating patients with dry eye include minimising eye drying medications including anti-depressants and anti-histamines. Humidification is helpful, even a pan of water in the bedroom can be helpful to provide humidification. Blinking is also important to remind your patients about. Tear film replacement is important. Preservative free artificial tears are preferable for patients who require regular tear replacement. Jim mentioned that patients can arrange for autologous serum tears from their blood bank which doesn’t cause reactions to preservatives. Topical cyclosporine (Restasis) and Lifitegrast can be useful medications for dry eye but aren’t that potent. Finally ophthalmologists can occlude the drainage with punctal occlusion or provide a scleral contact lenses.
Scleritis is also a cause of red eye but is much less common. It can be very painful, but this does vary. It is thought that scleritis occurs more commonly in those with rheumatoid arthritis. However the most common cause for scleritis in Professor Rosebaum’s clinic is granulomatosis with polyangiitis (GPA / formerly Wegener’s granulomatosis).
Episcleritis is another cause of red eye. Episcleritis is symptomatically a scratchy problem, but is usually short lived, and it has no complications, and is not associated with systemic disease.
The dogma about the cause of scleritis is that it is a vasculitis. Around 15% of scleritis patients will respond to a topical NSAID. After that fails the additional options are oral corticosteroid eg. starting with 60mg of prednisone. Some can be treated with steroid monotherapy alone however the majority need a steroid sparing agent like methotrexate or mycophenolate. Periocular steroids can be used but are usually avoided by Prof Rosenbaum. Biologics used for systematic disease can also have the side effect of treating the eye disease. Corneal melt is on a continuum with scleritis in rheumatoid arthritis. Previously treated with cyclophosphamide but often respond to systemic treatments used for RA now.









If you are a health practitioner, you may Login/Register to comment.
Due to the nature of these comment forums, only health practitioners are allowed to comment at this time.