Steroids, Not Biologics, Drive Arthroplasty Infections in RA Save
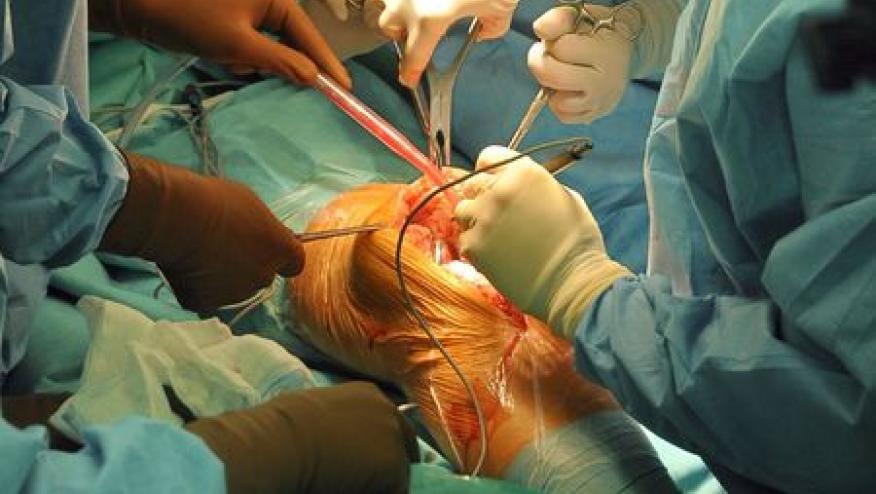
Medicare and Truven MarketScan administrative data study (2006 through 2015) of rheumatoid arthritis (RA) undergoing arthroplasty found that while that the risks of perioperative infection was similar across biologics, the infection risk with glucocorticoid use, especially at > 10 mg/d, was significantly greater.
Retrospective analysis of RA patients having elective knee or hip arthroplasty, looked at the influence of recently infused biologic therapies, including abatacept, adalimumab, etanercept, infliximab, rituximab, or tocilizumab.
A total of 9911 biologic-treated patients had 10,923 surgical procedures were identified.
The risk of hospitalized infection did not vary significanly with biologic use and ranged from:
- 6.87% with adalimumab
- 8.16% with abatacept
- 8.90% with rituximab C
The 1 year prosthetic joint infection (PJI) rates were:
- 2.14% with abatacept
- 0.35% with rituximab
- 3.67% with tocilizumab.
However glucocorticoids were associated with a dose-dependent increase in postoperative risk for all outcomes, including hospitalized infection (13.25%;CI, 9.72% to 17.81%) (vs. 6.78% on no steroids) and a predicted 1-year cumulative incidence of PJI of 3.83% (CI, 2.13% to 6.87%) (vs. 2.09%).









If you are a health practitioner, you may Login/Register to comment.
Due to the nature of these comment forums, only health practitioners are allowed to comment at this time.