Choices in GCA Save
It has been easy over time to presume that all advanced therapies in a disease area will work as well as each other. We have been so used to the idea that all b/tsDMARDs in rheumatoid arthritis are as effective as each other, given enough time, and that they all modify the disease to prevent the disability that we had become used to. It’s hard to change our thinking to be any different.
Similarly, in psoriatic arthritis, the arthritis scores have been hard to separate between the different agents. We are sufficiently convinced by this paradigm that we almost ignore the fact that there is a very clear hierarchy of effectiveness in psoriasis, guided by head-to-head comparisons.
I don’t think we can presume this applies to every disease.
There are a number of diseases where new biologic and targeted synthetic therapeutic options are coming online, and the temptation will be to consider them all equally. This will be made harder by the fact that the endpoint science in these diseases is not as well developed as it is for rheumatoid arthritis, psoriatic arthritis, or axial spondyloarthritis. Long-term implications for organ damage will have to be considered, and will have to be considered when agents are considered.
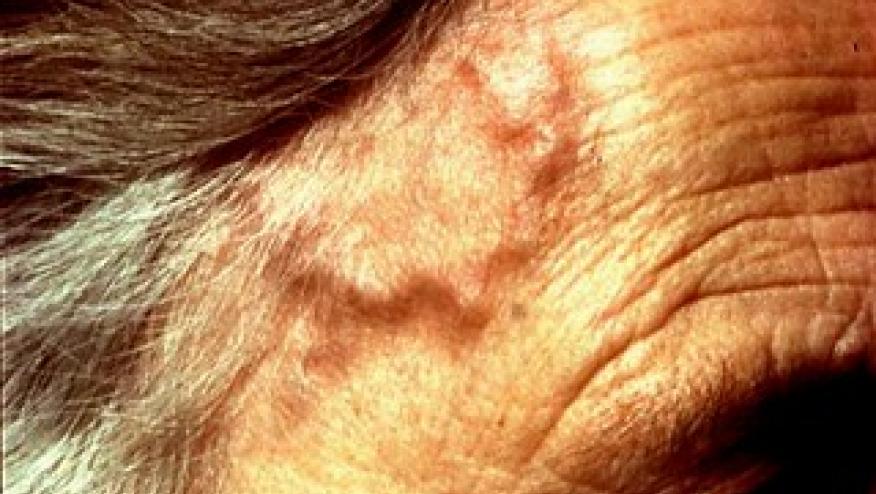
GCA is one of those diseases. Currently we only have one option, tocilizumab, and a well-designed clinical trial to support it, showing its clear steroid-sparing effect in the first 52 weeks. We had nothing like that before that, and the steroid burden on GCA patients was, at best, tragic. It was a welcome oasis in a desert of pain.
Now, however, we have had longer experience with it, and we are starting to really need to know what the endgame is for these patients, and exactly how far this benefit persists. What happens if we stop tocilizumab? Are we allowing smouldering inflammatory disease activity at the cellular level? Based on longstanding concerns re: Th1 versus Th17, are we leading to benefit in vessels, or just wiping the inflammation off the top? Are we actually disease modifying, or is it just steroid sparing?
At this EULAR 2024, two abstracts were presented from Carlo Salvarini’s group in Reggio Emilia, Italy, addressing this issue. The first looked at second temporal artery biopsies on patients still on tocilizumab for a median of 2.4 years, and showed a third of patients with serological disease control with ongoing positive temporal artery biopsy changes, despite PET improvements (OP0233). Additionally, in the TOPAZIO study, they showed patients who had tocilizumab with only three doses of pulse metyhlprednisolone at treatment initiation and no glucocorticoid after that, that after 52 weeks of tocilizumab, that PET uptake increased and there was a statistically significant increase in ascending aortic size after six months. Furthermore, in two patients who needed aneurysmal surgical repair, active granulomatous aortitis was noted (OP069).
These questions only come about because other options on the way. At EULAR 2024 we saw the late-breaking results of the SELECT-GCA study, a registration study for upadacitinib in GCA (LBA0001). It definitely seems to work, with better disease control with upadacitinib + a 26 week taper versus placebo + a 52 week taper, and appeared safe over the study period. I argued in my debate on JAK inhibitor safety with Janet Pope that safety needs to be contextual to the disease and the comparator, and in that context then upadacitinib might be a good option for many GCA patients.
Secukinumab in GCA is being tested in the G-CAPTAIN study and, while we have no idea what the results are going to be, I will be so shocked if it misses its primary that I promise that, if it does, I will buy beers for the whole bar at the relevant conference. It is also being tested in PMR in the REPLENISH study, and that could also help to guide decision-making.
It is possible that this conundrum is solved with cheap tocilizumab biosimilar for some longer duration of time, and studies will have to determine whether 24 months of tocilizumab confers an advantage over 12 months. However, it may well be that different therapeutic choices in GCA might not all be equal, and that some are used in preference to others, or that disease phenotyping will direct therapy selection. We should not assume that they all will be the same, and need to keep asking these questions and looking for the answers.









If you are a health practitioner, you may Login/Register to comment.
Due to the nature of these comment forums, only health practitioners are allowed to comment at this time.