Coccyx and Sacrococcygeal Joint Disorders Save

Pain from coccygeal or sacrococcygeal disorders is rare, often presenting as a diagnostic challenge. Coccygeal pain is often mistaken for lumbosacral, pelvic, or gastrointestinal disorders. This review presents the epidemiology, anatomy, biomechanics, presentations, diagnostic evaluation, imaging and management of coccygeal disorders, including surgery.
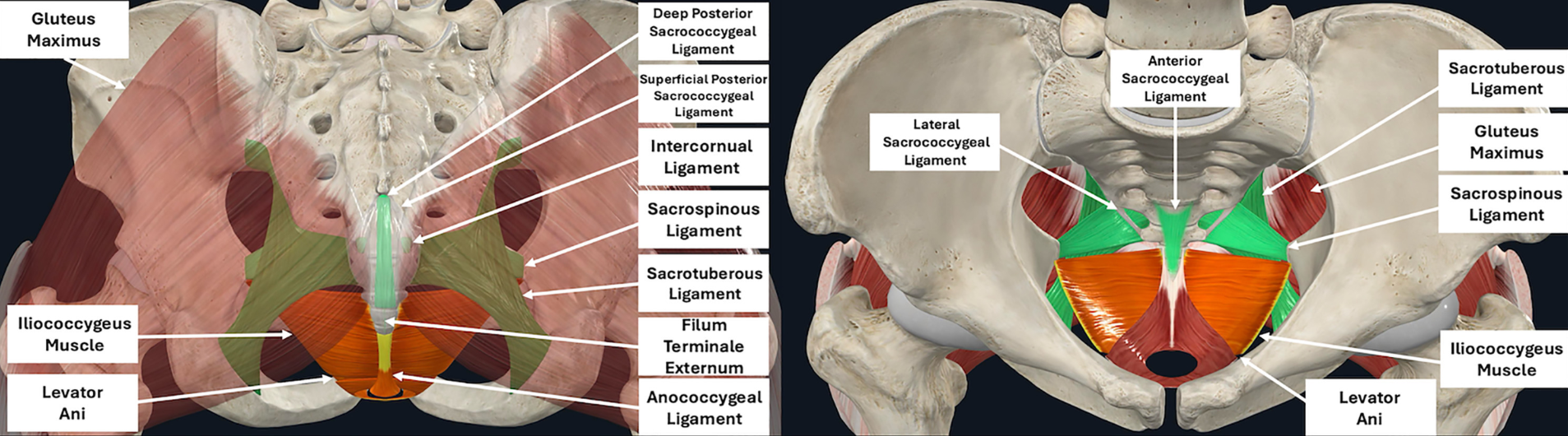
Disorders of the coccyx and sacrococcygeal joint lie at an intersection of spinal biomechanics, pelvic floor function, and chronic pain physiology. Although frequently regarded as minor or self-limiting, these conditions can cause disability comparable to more familiar spinal pathologies. A clear understanding of anatomic variation, joint motion, and the relationship between mechanical, inflammatory, and sympathetic pain mechanisms is essential for accurate diagnosis and appropriate treatment selection.
Pain in disorders of the coccyx and sacrococcygeal joint arises from mechanical overload, inflammation, and neural sensitization. Common initiating factors include direct trauma, repetitive microtrauma from sitting, degenerative change, or instability at the sacrococcygeal or intercoccygeal joints.
Hypermobility is another frequent cause of chronic coccydynia. Normally, the coccyx flexes slightly during sitting and returns to neutral on standing. When motion exceeds ∼25° of flexion or anterior subluxation occurs, repetitive shear stress induces inflammation and pain. Dynamic sitting–standing radiographs are essential to diagnosis.
Infection (eg, osteomyelitis) is rare but may present as coccydynia. Risk factors include diabetes, immunosuppression, prior procedures, or injections. Diagnosis relies on MRI, which shows marrow signal change and soft-tissue enhancement. Neoplastic lesions are also uncommon, presenting as chordoma (a primary malignancy) or metastases from colorectal, prostate, or gynecologic cancers.
Coccygeal disorders typically present with midline tailbone pain worsened by sitting or during sit-to-stand transitions and are relieved by leaning forward or using cushions, suggesting a mechanical pain source. Point tenderness over the coccyx is characteristic, as is pain with defecation, intercourse, or prolonged driving.
Key Points
- Coccydynia accounts for only 1–3% of back pain
- 5 times more common in women
- 3 times more common in obese individuals
- Image-guided interventions, especially ganglion impar and sacrococcygeal joint injections, can be both diagnostic and therapeutic
- Contributors include:
- trauma
- Obesity or significant changes in weight
- degenerative disease (with hypermobility or dislocation)
- obstetric injury (posterior dislocation or fracture reported in 5–15% of multiparous women with postpartum pain.
- Uncommon causes - infection, neoplasm, systemic inflammatory disease, and pelvic floor dysfunction
- Dynamic seated and standing radiographs are the preferred initial imaging modality
- Secondary CT and MRI may help delineate structural, degenerative, or inflammatory pathology
- Prognosis is best influenced by phenotype (mobility/instability, spicule, degeneration), BMI/trauma history, and response to diagnostic injections
- Worse prognosis seen with obesity
Treatment
- Non-operative management: includes education/off-loading, cushions, NSAIDs/analgesics, pelvic-floor–aware PT
- Interventions:
- Image-guided ganglion impar block (GIB) has the strongest signal for refractory coccydynia.
- Surgery: in select refractory cases, coccygectomy yields high satisfaction and durable pain relief
- traumatic cases may derive greater benefit from coccygectomy than atraumatic cases









If you are a health practitioner, you may Login/Register to comment.
Due to the nature of these comment forums, only health practitioners are allowed to comment at this time.