Infections Rheums Should Worry About Save
With the increasing development and use of new biologics and oral targeted therapies to treat RA and other immune mediated inflammatory diseases (IMIDs), an awareness of infection risk and prevention has become of increasing interest as well. While our patients may be susceptible to many different types of infections depending on immunosuppressive regimen, age and co-morbidities, I’ll highlight a few of the “usual suspects”.
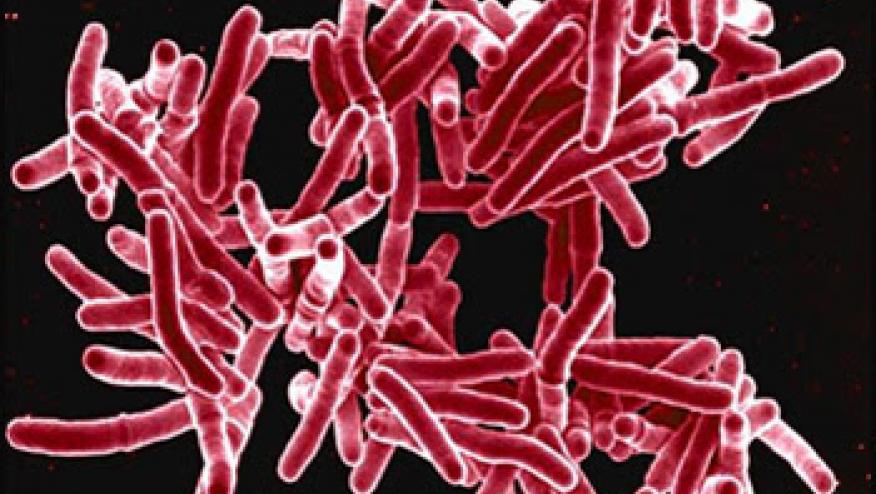
Latent TB infection (LTBI) – not technically a “usual suspect” and relatively uncommon in the U.S., however LTBI screening remains of interest (in particular to insurance companies) due to risk of reactivation of LTBI with certain biologics, most notably TNF inhibitors. In realty, it is far more common in the U.S. for TNFi to be complicated by an endemic fungal infection (e.g. histoplasmosis), but regardless patients should be screened for LTBI prior to biologic therapy, preferably with an interferon gamma release assay. A note of caution - a positive IGRA or TST dose not differentiate between LTBI and active TB, and a negative test does not rule out active TB, if there is concern for this.
Chronic hepatitis B (and C) – this is a free kick at the ball. EVERY patient should be screened for hepatitis B prior to starting any immunosuppression, and since every adult should be screened for hepatitis C at least once, this is a great opportunity to test, especially because there now exist curative treatments. Recommended testing: HBsAg, HBsAb (to determine need for vaccination), HBcAb and Hep C antibody.
Herpes Zoster – reactivation of varicella zoster virus can be associated with substantial morbidity beyond that of the acute pain or post herpetic neuralgia, including disseminated infection and stroke. Age remains the number one risk factor for zoster, although risk is significantly increased by certain immunosuppressants, most notably JAK inhibitors, and prevention is key. Fortunately, there is a highly effective vaccine, the recombinant zoster vaccine (RZV), that as of 2021 is approved and recommended for anyone 18 years and up who is immunocompromised. Not every IMIDs patient < 50 years needs RZV quite yet but think higher risk patients such as those on JAK inhibitors or anifrolimab.
Pneumocystis jirovecii pneumonia – the decision to prophylax against this notable infection is complex given its low frequency but high mortality rate in patients with IMIDs, and use remains variable with lack of consensus guidelines. Data support a risk stratified approach, considering risk factors such as dose and duration of steroids (#1 risk factor), concomitant agents (rituximab), lymphocyte count, increasing age and presence of chronic lung disease. Contradictory data regarding rituximab do exist. A recent study by Jeff Curtis and colleagues suggests that not all rituximab patients need PJP prophylaxis, but those on high dose steroids likely do with favorable NNT Primary Prophylaxis for Pneumocystis jirovecii Pneumonia in Patients Receiving Rituximab - PubMed (nih.gov)
At every patient visit identify and quantify patients’ infection risk based on disease, drug, comorbidities and age. Think of the above infections in particular. Do they need prophylaxis? Are immunizations and screening up to date? And most important of all, systemic glucocorticoids remain the biggest risk factor for infection, and the risk is dose dependent.










If you are a health practitioner, you may Login/Register to comment.
Due to the nature of these comment forums, only health practitioners are allowed to comment at this time.