Should We Screen Younger Postmenopausal Women for Osteoporosis? Save
Do postmenopausal women, under age 65 years, need a baseline BMD testing? A JAMA Insights review suggests that the absolute risk of fracture is low in this group and that USPSTF guidelines should be considered - that we should be screening women younger than 65 years who are at increased risk of osteoporosis and we should be using a formal risk assessment tool to identify candidates for bone density testing.
In the absence of a history of hip or vertebral fracture, osteoporosis screening is aimed at identifying individuals with a BMD T-score of −2.5 or lower because those individuals may be candidates for osteoporosis pharmacotherapy.
Studies have clearly demonstrated the benefits of treating postmenopausal women with existing vertebral fractures or bone mineral density (BMD) T-scores of −2.5 or lower and among adults aged 50 years and older with recent hip fracture. Also, the US Preventive Services Task Force (USPSTF)1 recommends routine osteoporosis screening with BMD testing among women aged 65 years and older. But what about those who are postmenopausal but under age 65 yrs.?
The absolute fracture risk for any given BMD is much lower in younger postmenopausal women than in older women. The estimated 5-year probability of spinal fracture among postmenopausal women according to age groups:
- 50-54 yrs: 0.3%
- 55-59 yrs: 0.5%
- 60-64 yrs: 1.0%
There is no consensus regarding osteoporosis screening in younger postmenopausal or what risk factors that should drive this decision.
The USPSTF recommends osteoporosis screening in postmenopausal women under age 65 years who are increased risk of osteoporosis (low body weight, parental history of hip fracture, smoking) and tht a formal risk assessment tool should be used, including
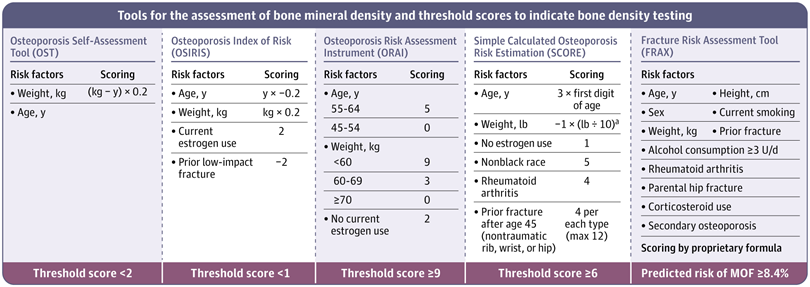
- Osteoporosis Self-Assessment Tool [OST]
- Osteoporosis Risk Assessment Instrument [ORAI]
- Osteoporosis Index of Risk [OSIRIS]
- Simple Calculated Osteoporosis Risk Estimation [SCORE])
There were specifically designed to identify individuals with a BMD T-score of −2.5 or lower.
In contrast the FRAX (Fracture Risk Assessment Tool), was designed to estimate 10-year probabilities of hip and major osteoporotic fracture using clinical risk factors with or without femoral neck BMD. Using the FRAX, the USPSTF recommends a treatment threshold of 8.4% (for 10-year probability of major osteoporotic fracture).
This review compares sensitivity, specificity and thresholds for treatment using OST, ORAI, OSIRIS anf FRAX in younger postmenopausal women.










If you are a health practitioner, you may Login/Register to comment.
Due to the nature of these comment forums, only health practitioners are allowed to comment at this time.