2023 EULAR Recommendations for Imaging in Large Vessel Vasculitis Save
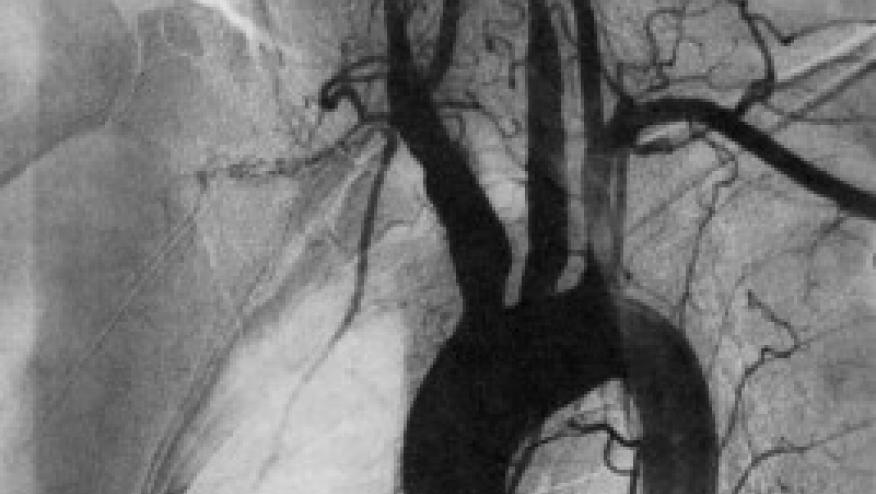
EULAR has published its expert consensus regarding the recommendations for imaging in the most common types of large vessel vasculitis (LVV) -- giant cell arteritis (GCA) and Takayasu arteritis (TAK). Imaging facilitates diagnosis and rapid management to prevent vascular damage and ischemic consequences (eg, blindness, aneurysm).
EULAR recommendations for the management of LVV covering assessment, investigation, and treatment were first developed in 2008.1 The 2018 update noted that one of the key points of management is that LVV diagnosis should be confirmed by imaging or histology. To support this, specific recommendations around the use of imaging were developed alongside the management guidelines in 2018. Since then new studies have been published, and in 2021 the American Rheumatology Association (ACR) expressed a preference for biopsy over ultrasound.
The updated 2023 EULAR recommendations were developed by a multidisciplinary task force of patient representatives and health care professionals from rheumatology, as well as experts in radiology and imaging. The work was completed in line with EULAR standardized operating procedures, and based on a systematic literature review.
Overall, three overarching principles and eight recommendations were developed (see below) The principles state that for people with with suspected GCA, early imaging is recommended to support the clinical diagnosis, but imaging should not delay treatment being started. Imaging should be done by a trained specialist using appropriate equipment, standardized operational procedures, and settings – and for those with positive results on imaging, the diagnosis of GCA may be made without a biopsy or further tests. In people with a low clinical probability and a negative imaging result, the diagnosis of GCA can be considered unlikely. In all other situations – including inconclusive imaging – additional steps will need to be taken to reach a diagnosis.
The individual recommendations make specific points around the optimal use of ultrasound, MRI, CT, and FDG-PET for imaging. The recommendations are based on evidence and expert consensus, and the full text of each can be found in the August 2023 issue of the Annals of the Rheumatic Diseases.
With reference to the current technical differences between Europe and the United States, EULAR acknowledges that it does not intend to dismiss the role of temporal artery biopsy in GCA; however, when imaging is rapidly available the added value of a biopsy is uncertain, and may expose patients to an unnecessary risk of complications. EULAR hopes these updated recommendations will help to standardize and optimize the use of imaging in the diagnosis and assessment of people living with GCA and TAK in Europe, and may prove aspirational for other regions who may wish to promote a change of clinical routine.
OVERARCHING PRINCIPLES
- In patients with suspected GCA, an early imaging test is recommended to support the clinical diagnosis of GCA, assuming high expertise and prompt availability of the imaging technique. Imaging should not delay initiation of treatment.
- Imaging examination should be done by a trained specialist using appropriate equipment, standardised operational procedures and settings.
- In patients in whom there is a high clinical suspicion of GCA and a positive imaging result, the diagnosis of GCA may be made without an additional test (biopsy or further imaging). In patients with a low clinical probability and a negative imaging result, the diagnosis of GCA can be considered unlikely. In all other situations (including the case of an inconclusive imaging result), additional efforts towards a diagnosis are necessary.
RECOMMENDATIONS
-
Ultrasound of temporal and axillary arteries should be considered as the first imaging modality to investigate mural inflammatory changes in patients with suspected GCA.
-
High-resolution MRI or FDG-PET* can be used as alternatives to ultrasound for the assessment of cranial arteries† in patients with suspected GCA.
-
FDG-PET*, alternatively MRI or CT, can be used for the detection of mural inflammation or luminal changes of extracranial arteries in patients with suspected GCA.
-
In patients with suspected TAK, MRI to investigate mural inflammation or luminal changes should be used as the first imaging test to make a diagnosis of TAK.
-
FDG-PET, CT or ultrasound may be used as alternative imaging modalities in patients with suspected TAK. Ultrasound is of limited value for assessment of the thoracic aorta.
-
Conventional angiography is not recommended for the diagnosis of GCA or TAK as it has been superseded by the previously mentioned imaging modalities.
-
In case of a suspected relapse of GCA or TAK, particularly when laboratory markers of disease activity are unreliable, ultrasound, FDG-PET or alternatively MRI may be considered for the assessment of vessel abnormalities. Imaging is not routinely recommended for patients in clinical and biochemical remission.
-
In patients with GCA or TAK, MRA, CTA or ultrasound of extracranial vessels may be used for long-term monitoring of structural damage, particularly at sites of preceding vascular inflammation. The frequency of screening as well as the imaging method applied should be decided on an individual basis.










If you are a health practitioner, you may Login/Register to comment.
Due to the nature of these comment forums, only health practitioners are allowed to comment at this time.