Behçet’s Syndrome Save
A comprehensive overview of Behcet's syndrome appeared in last week's NEJM, reviewing the numerous advances in the immunogenetics, syndrome recognition, and targeted therapeutic approaches. Despite certain advances, there remains a need for better clinical trials, better diagnostic tools, and biologic treatments to afford better outcomes.
Behcet's is systemic vasculitis affecting veins and arteries of all sizes and manifesting as chronic, multisystem, inflammatory condition with a relapsing and remitting course. Highlights from this review article include:
- Affects adults between the ages of 15 and 45 years (mean age at diagnosis is 30 years).
- Prevalence: ranges from 0.3 to 4.9 cases/100,000 persons in northern Europe to 1.5 to 15.9 cases/100,000 persons in southern Europe. In the USA, the prevalence is 5.2 cases per 100,000 persons. Prevalence is highest in Turkey - 420 cases per 100,000 persons
- It has both autoimmune and autoinflammatory features.
- Environmental triggers include: microorganisms (bacteria, viruses, and their byproducts), histamine-releasing foods (e.g., citrus fruits, nuts, and cheese), poor oral hygiene, and stress. There are theories of an altered gut and salivary mucosal microbiome contributing to the onset of Behçet’s syndrome
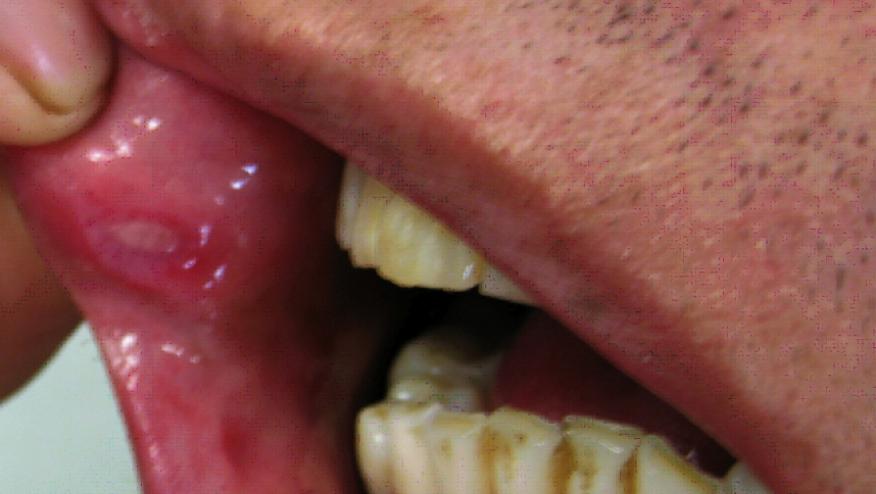
- Clinical manifestations affect the skin, mucosa, joints, eyes, vascular system, central nervous system, and gastrointestinal tract.
- Genital ulcers occur two thirds of cases, tend to be larger, deeper, and longer-lasting than oral ulcers. Most appear on the scrotum or labia.
- Monoarthralgia or oligoarthralgia is more common than arthritis or enthesitis
- Venous involvement includes superficial thrombophlebitis and deep-vein thrombosis (15 to 40% of patients)/
- There is no diagnostic test or genetic marker. Use of the revised 2014 Classification Criteria in practice may be limited.
- Treatment needs to be tailored to the organ system involved
- Skin/Oral/Joints: may require topical glucocorticoids, intraarticular glucocorticoids, colchicine and apremilast. Less commonly utilized and poorly studied agents include azathioprine, thalidomide, interferon alfa, and etanercept.
- Major organ involvement (for ocular and CNS disease) may azathioprine, interferon alfa, TNF inhibitors, or cyclosporine.










If you are a health practitioner, you may Login/Register to comment.
Due to the nature of these comment forums, only health practitioners are allowed to comment at this time.